Layout


E,RISKINGDEATHM LIFE,
GIVING LIFE, RISKING DEATH
MATERNAL MORTALITY IN BURKINA FASO
More than 2,000 women die in Burkina Faso every year from
complications of pregnancy and childbirth. Most of these deaths
could be prevented.
Some women die because they cannot reach a health facility capable
of treating them, or because they arrive too late. Many lose their livesbecause their relatives cannot pay the fees demanded by medical
personnel. Others die because of shortages – of blood, drugs,
equipment or qualified medical staff. Maternal mortality takes itsmajor tol on the poorest and the least educated women and those
who live in rural areas, home to 80 per cent of the population.
The authorities in Burkina Faso have devoted effort and resourcesto reducing maternal mortality, with the help of the donor community.
However, many pregnant women stil cannot obtain the health carethey need in time, and pregnancy al too often ends in tragedy.
Amnesty International cal s for better information and services for
family planning, for the government to remove financial barriers to
maternal health care and for improvements in access to care. To do
less is to violate the right to health of the women of Burkina Faso.
ISBN 978-0-86210-457-3
MATERNAL MORTALITY
170 x 244 mm
170 x 244 mm
GIVING LIFE, RISKING DEATHMATERNAL MORTALITY IN BURKINA FASO
AMNESTY INTERNATIONAL IS A GLOBAL MOVEMENT OF 2.2 MILLIONPEOPLE IN MORE THAN 150 COUNTRIES AND TERRITORIES WHOCAMPAIGN TO END GRAVE ABUSES OF HUMAN RIGHTS. OUR VISIONIS FOR EVERY PERSON TO ENJOY ALL THE RIGHTS ENSHRINED INTHE UNIVERSAL DECLARATION OF HUMAN RIGHTS AND OTHERINTERNATIONAL HUMAN RIGHTS STANDARDS. WE ARE INDEPENDENTOF ANY GOVERNMENT, POLITICAL IDEOLOGY, ECONOMIC INTERESTOR RELIGION – FUNDED MAINLY BY OUR MEMBERSHIP ANDPUBLIC DONATIONS.
Published byAmnesty International SecretariatPeter Benenson House1 Easton StreetLondon WC1X 0DWUnited Kingdom
Amnesty InternationalPublications 2009Index: AFR 60/001/2009
ISBN: 978-0-86210-457-3Original language: EnglishBritish Library Cataloguing in Publication Data.
A catalogue record for this book is available from the British Library.
Cover photo, front:Women crack nuts surrounded by their children. Despite equal status in law, many women are subordinateto the men in their lives and are unable to make decisions about their own health. Anna KariCover photo, back:Ramatoulaye and her baby daughter by the Nakambe river close to Wonko, Burkina Faso.
Four months earlier she was forced to give birth on the river bank because there was no boat availableto take her across. Anna Kari
Printed on 100 per cent recycled post-consumer waste paper byLightning SourceMilton Keynes, United Kingdom
Al rights reserved. This publication is copyright, but may be reproduced by any method without fee for advocacy,campaigning and teaching purposes, but not for resale. The copyright holders request that al such use beregistered with them for impact assessment purposes. For copying in any other circumstances, or for re-use inother publications, or for translation or adaptation, prior written permission must be obtained from thepublishers, and a fee may be payable.

GIVING LIFE, RISKING DEATHMATERNAL MORTALITY IN BURKINA FASO
Amnesty International Publications
OBJECTIVES OF THIS REPORT
2/WOMEN'S STATUS IN BURKINA FASO
WOMEN'S STATUS IN THE FAMILY
‘THE FIRST TO GET UP IN THE MORNING AND THE LAST TO GO TO SLEEP'
FEMALE GENITAL MUTILATION
EARLY MARRIAGES AND PREGNANCIES
POLYGAMY AND FORCED MARRIAGE
WOMEN'S LACK OF POWER
3/GOVERNMENT POLICIES
INCREASING BUDGET ALLOCATION
ORGANIZATION OF THE HEALTH SYSTEM
TRADITIONAL BIRTH ATTENDANTS AND AUXILIARY MIDWIVES
4/THE HUMAN RIGHTS FRAMEWORK
THE RIGHT TO HEALTH
PREVENTABLE MATERNAL MORTALITY IS A VIOLATION OF THE RIGHT TO LIFE
MATERNAL HEALTH IS A RIGHT
THE RIGHT TO NON-DISCRIMINATION
SEXUAL AND REPRODUCTIVE RIGHTS
5/FAMILY PLANNING
USE OF CONTRACEPTIVES REMAINS LOW
BARRIERS TO THE USE OF CONTRACEPTIVE SERVICES
INADEQUATE INFORMATION ON SEXUAL AND REPRODUCTIVE RIGHTS
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
QUALITY CONCERNS IN FAMILY PLANNING SERVICES
CONTRACEPTIVE PRODUCTS NOT ALWAYS AVAILABLE
COSTS ARE AN OBSTACLE TO CONTRACEPTIVE USE
RESISTANCE FROM HUSBANDS OR OTHER RELATIVES
INADEQUATE FINANCING OF FAMILY PLANNING
CLANDESTINE AND UNSAFE ABORTIONS
ABORTION: THE LEGAL FRAMEWORK
MNESTY INTERNATIONAL'S POSITION ON ABORTION
6/HEALTH FACILITIES HARD TO REACH
DIFFICULT JOURNEYS
7/COSTS AS A BARRIER TO HEALTH CARE
THE 2006 SUBSIDY POLICY
LACK OF INFORMATION ON THE SUBSIDY POLICY
NO FREE TRANSPORT BETWEEN HEALTH FACILITIES
NO CRITERIA TO IDENTIFY WOMEN ENTITLED TO FREE CARE
UNOFFICIAL PAYMENTS
THE DEBATE AROUND TOTAL FEES EXEMPTION
PILOT PROJECTS PROVIDING FREE CARE
REMOVING FINANCIAL BARRIERS TO MATERNAL HEALTH CARE
THE RIGHT TO HEALTH AND FINANCIAL BARRIERS
8/SHORTAGES OF STAFF AND SUPPLIES
INADEQUATE HEALTH INFRASTRUCTURE
DILAPIDATION AND INSANITARY CONDITIONS IN HEALTH PREMISES
ELECTRICITY SUPPLY
WORKING CONDITIONS
SHORTAGES OF DRUGS AND MEDICAL EQUIPMENT
SHORTAGES OF EQUIPMENT AND DISREPAIR
SHORTAGES AND POOR QUALITY OF MEDICAL SUPPLIES
SHORTAGES OF DRUGS
RECURRING BLOOD SHORTAGES
LACK OF TRAINED MEDICAL PERSONNEL
LACK OF SKILLED BIRTH ATTENDANTS
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
9/SUB-STANDARD CARE
SERIOUS FAILURES IN THE REFERRAL SYSTEM
DELAYS IN REFERRAL DECISIONS
LACK OF EMERGENCY CAPACITY IN DISTRICT AND REGIONAL HOSPITALS
BLOOD SHORTAGES IN DISTRICT AND REGIONAL HOSPITALS
LACK OF AMBULANCES FOR TRANSFERRING PREGNANT WOMEN
NO COMMUNICATIONS BETWEEN HEALTH FACILITIES
PATIENTS AND MEDICAL PERSONNEL: RELATIONSHIP DIFFICULTIES
LOW MORALE AMONG HEALTH STAFF
NEGATIVE ATTITUDES TOWARDS PATIENTS AND THEIR FAMILIES
NEGLIGENCE AND VIOLENCE DURING LABOUR
LACK OF MONITORING OF POLICY IMPLEMENTATION
FAMILY PLANNING: THE UNMET NEED FOR CONTRACEPTION
SHORTAGES AND MISAPPROPRIATION OF DRUGS AND MEDICAL SUPPLIES
ACCOUNTABILITY OF MEDICAL PERSONNEL
CHARTER OF PATIENTS' RIGHTS
LACK OF SANCTIONS
INVESTIGATING MATERNAL DEATHS AND NEAR-MISSES
ABSENCE OF EFFECTIVE REMEDIES
LACK OF POLITICAL WILL TO COMBAT CORRUPTION
11/ROLE OF DONORS
SOURCES OF DEVELOPMENT ASSISTANCE
GENERAL BUDGET SUPPORT
POOLED DONOR FUNDING FOR THE HEALTH SYSTEM
DIRECT SUPPORT FOR PROJECTS OR SPECIFIC PARTNERS
AN APPROACH BASED ON GENDER EQUALITY
FACTORS REDUCING THE EFFECTIVENESS OF INTERNATIONAL AID
PROBLEMS OF COORDINATION
INADEQUATE OUTCOME EVALUATION
12/CONCLUSION AND RECOMMENDATIONS
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
ABBREVIATIONS USED IN THIS REPORT
Association burkinabè pour le bien-être familial, BurkinabèAssociation for Family Welfare
African Charter on Human and Peoples' Rights
African Development Bank
Acquired Immune Deficiency Syndrome
Amélioration de la qualité et de l'accès aux soins obstétricauxd'urgence, Improvement of the quality of and access toemergency obstetric care
Autorité supérieure de contrôle de l'État, Superior Authority ofState Control
Association Songui Manégré / Aide au développementendogène, Songui Manégré Association / Aid to EndogenousDevelopment
Attaché(e) Soins Santé en Obstétrique et Gynécologie,Obstetric and Gynecological Health Care Attaché
Centrale d'achats des médicaments essentiels génériques etdes consommables médicaux, Purchasing centre for essentialgeneric drugs and medical goods
Cadre de concertation genre, Gender consultation framework
Convention on the Elimination of All Forms of Discriminationagainst Women
UN Committee on the Elimination of Discriminationagainst Women
Certificat d'études primaires élémentaires, Elementary school-leaving qualification
UN Committee on Economic, Social and Cultural Rights
Common currency of 14 countries in West and Central Africalinked to the Euro. CFA stands for Communauté financièred'Afrique (Financial Community of Africa)
Centre hospitalier régional, regional hospital
Centre hospitalier universitaire, university hospital
Centre médical avec antenne chirurgicale, medical centre withsurgical services, district hospital
Comité de gestion des services de santé, health managementcommittee
Convention on the Rights of the Child
Centre de recherche du Centre hospitalier de l'Universitéde Montréal, Research Centre, Montreal University Hospital
Centre de santé et de promotion sociale, community healthcentre
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Demographic and Health Survey
European Commission Humanitarian Office
Economic Community of West African States
Emergency Obstetric and Neonatal Care
Fédération des Associations de Sages-Femmes de l'Afrique duCentre et de l'Ouest, Federation of Associations of Midwivesfrom Central and West Africa
Female Genital Mutilation
International Federation of Gynaecology and Obstetrics
Global Alliance for Vaccines and Immunisation
Deutsche Gesellschaft für Technische Zusammenarbeit,German agency for technical assistance
Haute autorité de coordination de la lutte contre la corruption,High Commission for the Coordination of Anti-CorruptionActivities
Human Immunodeficiency Virus
International Covenant on Civil and Political Rights
International Covenant on Economic, Social and CulturalRights
International Confederation of Midwives
Millennium Development Goals
National blood transfusion centres
National Human Rights Commission
Programme d'appui au Développement Sanitaire, Supportprogramme for the development of the health sector
Plan national de développement sanitaire, National HealthDevelopment Plan
Réseau National de Lutte Anti-Corruption, National Network toFight Against Corruption
Recensement général de la population et de l'habitat, GeneralPopulation and Housing Census
Sexually transmitted infections
Terre des Hommes, an NGO working for the rights of children
Universal Declaration of Human Rights
United Nations Convention against Corruption
United Nations Development Programme
United Nations Population Fund
United Nations Children's Fund
United States Agency for International Development
World Health Organization

GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Mothers and their newborn babies in Kiembara clinic.
Many women in Burkina Faso cannot access the healthservices they need.
‘A PREGNANT WOMAN HAS A FOOT IN THE GRAVE
AND A FOOT ON THE EARTH'1African saying
Every year, more than 2,000 women die in Burkina Faso from complications ofpregnancy and childbirth.2 Most of these deaths could have been prevented.
Many women die because they need blood but none is available. Others die fromobstructed labour, infections or hypertension because they are unable to reach ahealth facility capable of treating them, or because they arrive too late. Many losetheir lives because their relatives cannot pay the fees being asked for by medicalpersonnel. Many more do not even reach health facilities because of geographical,financial or cultural barriers.
There are many reasons why women in Burkina Faso do not receive the health carethey need. These include: lack of information on sexual and reproductive health andrights; women's low status, which undermines their right to decide whether, whenand how many children to have; social and economic barriers, notably the cost ofmedical treatment; geographic barriers obstructing access to health facilities; andpoor quality of treatment due to shortages of medical supplies and qualifiedpersonnel.
Maternal mortality3 takes its major tol on the poorest and the least educated womenand those who live in rural areas, home to 80 per cent of the population.
The maternal mortality ratio4 is high, although according to official statistics it hasdecreased from 566 per 100,000 live births in 1993 to 484 in 1999,5 and to 307 in2008.6
The direct medical causes of maternal deaths in Burkina Faso have been consistentlyidentified as haemorrhage, infection, uterine rupture, post-abortion complications,eclampsia (seizures or coma in a patient with pregnancy-induced hypertension) andplacenta retention.7 These complications are treatable if women have timely accessto the means to prevent unwanted pregnancy and safe abortion services, to a skil edattendant at delivery, to a functioning referral system and to adequate emergencyobstetric care.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
The authorities in Burkina Faso have not ignored this tragedy, a tragedy that deprivesthousands of families of their wives, mothers, daughters and sisters. During the lastdecade the authorities, with the help of the donor community, have devoted effort andresources to reducing maternal mortality.
Ambitious strategies have been developed and partial y implemented. In 2006 thegovernment adopted a subsidy policy based on the principle that 80 per cent of thecost of deliveries and emergency obstetric and neonatal care would be met by thegovernment.
Efforts have also been made to increase the number of trained medical personnel,including midwives and nurses, and to enhance their skil s. In an effort to encouragemore women to give birth in health facilities, rather than at home, the role of traditionalbirth attendants8 has been changed from assisting women in deliveries to promotingmedical y assisted delivery and helping women gain access to these services. Primaryhealth care centres have been built throughout the country. The government has alsoadopted a national strategy for family planning.
However wel elaborated on paper, the policies to combat maternal mortality sufferfrom major flaws in their implementation. Although the cost of deliveries has beenreduced since 2006, access to adequate medical services continues to be a problemand many women remain reluctant to go to health facilities to give birth. This isparticularly the case among poor and rural women who face treatment in healthfacilities which are often unhygienic and understaffed, with medical personnel whoare underpaid and sometimes treat them disrespectful y.
The situation is particularly acute in the area of family planning. Although figuresvary, it is clear that contraceptive use remains low. Despite passing a Law onReproductive Health in 2005 that entitles couples and individuals to decide freelywhether and when to have children, the government stil does too little to ensure thatwomen and girls have safe and confidential access to information and to moderncontraceptive methods. The result is a large number of early, unwanted or life-threatening pregnancies, as wel as unsafe abortions. Family planning is severelyunderfunded, partly because, until recently, international donors and the governmenthave concentrated on other public health priorities, notably the AIDS pandemic, polioand malaria.
Several structural factors continue to prevent women from enjoying their right to healthcare that is available, accessible, acceptable and of good quality.
� Availability of care is undermined by a lack of adequate health facilities as wel asshortages in medical supplies and personnel.
� Accessibility is hampered both by geographical and financial barriers and bywomen's lack of information and decision-making power.
� Acceptability of care is compromised by the disrespectful or even cruel attitudesand conduct of some medical personnel.
� Quality of care is often inadequate, with medical staff not properly monitored orheld accountable, and poor pay and conditions for staff.
Aïcha's story is one of many which il ustrate the obstacles women face on the journeythrough pregnancy to childbirth, the suffering they may endure, and in many cases,the tragic and preventable loss of life.
Aïcha died in April 2008 in Ouagadougou, aged 21.
Aïcha was the only daughter in a family of five children. She met her husband, Abdou,in Ouagadougou and they were engaged for two years before getting married. NeitherAïcha or Abdou went to school. Abdou, who was 25 years old in 2008, works irregularlyas an assistant carpenter, but has been without steady employment for the past year.
Aïcha used to sell benga, a mix of beans and rice, and worked until the very last day ofher pregnancy. She had to fetch wood several kilometres away from their home, andwould wake up at 5am every day to cook the benga. She then went to sell it on the roadnear her home, returning at 4pm to prepare the evening meal. "She worked every day,unless she had something else to do like the laundry", her husband said.
This was her first pregnancy, and she attended the three recommended prenatal visitsat the CSPS (community health centre). Her husband Abdou told Amnesty International:"I never accompanied her on these visits but I thought that it was a good thing that shewas treated there." During her pregnancy, Aïcha was prescribed iron for her anaemiaand maloxine to prevent malaria.
A male nurse at the CSPS where Aïcha was treated told Amnesty International: "Shecould not pay for a single prescription. We even found some of them in her health recordwhich had not been used."
In April 2008, at around 8pm, Aïcha had labour pains. A friend took her to the healthcentre 1km from her home on a small motorcycle and her husband followed on a bicycle.
She gave birth to a boy at 2am. After the delivery, the medical personnel asked the familyto buy bleach to clean up her blood.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Ten minutes after the delivery, the midwife told the family that Aïcha had to be transferredto a district hospital because she was suffering from a haemorrhage. The head of thecommunity health centre told Amnesty International: "We transferred her to a districthospital nearby for transfusion because we don't have blood here."
Although transfers between health centres should be free under the government's subsidypolicy, the family had to pay for transport. Abdou said: "An ambulance had already beencalled to transfer her to the hospital. The ambulance driver insisted on receiving 1,500CFA francs (around US$3.50) before he would start his vehicle. He did not give us areceipt."
Abdou told Amnesty International: "When we arrived at the hospital, Aïcha was stillbleeding. Her clothing was soaked with blood and so was the stretcher. The driver helpedus carry her to the treatment room. We were given a prescription. We had to pay for thegloves and bleach. I went to buy them with a friend. When we came back, a health workergave us a new prescription and I bought medicine and pills for a total of 4,500 CFAfrancs (around US$10). Ten minutes later, a third prescription was given to us for otherpills and bottles for 3,500 CFA francs (around US$8)."
Aïcha's husband was then told to get his wife's blood tested: "I first went to the hospitallab where I was told that they could not do the blood test. I was sent to the lab at anearby health centre specializing in blood tests. It was almost 3am and I had no transport,so I went on foot. It took me an hour to get there. When I reached the health centre, thewatchman was asleep. So I woke him up and spent 2,000 CFA francs (around US$4.50)on the test. I quickly went by taxi to the district hospital: the first one broke down andI had to find another, which charged 1,000 CFA francs (around US$2) – the normal fareis less than 200 (around US$0.50) but when taxis see that people are in a hurry, theycharge higher prices. It was past 5am when I arrived at the hospital and delivered theblood test results. When I arrived, I didn't find my mother and friends. I was told thatthey had already left. I thought that Aïcha had felt better and was cured. Then a doctorcame. He spoke French to me but once he saw that I did not understand, he addressedme in Mooré.9 He told me that my wife was very weak and that ‘her blood was all gone'.
I learnt that she died at 5:18am."
Abdou returned on foot to his home with his newborn baby. Abdou's mother, who usedto live in a village, came to live with her son in order to take care of the baby.
As this story shows, even when a woman lives in Ouagadougou, close to a healthfacility, her access to vital treatment can be undermined by lack of essential medicalservices, including blood, and by unofficial and arbitrary costs. Families are in practicebeing charged significant sums for medicines and other medical services that shouldbe subsidized under the 2006 subsidy policy.
Al the barriers met by pregnant women in Burkina Faso increase the three criticaldelays10 that add to the risk of maternal death: the delay in making the decision toseek care, the delay in reaching the health facility and the delay in receiving treatmentat the health facility.
� Delay in the decision to seek care: in Burkina Faso, women usual y depend ontheir husbands or their in-laws to take the decision to go to a health centre.
� Delay in reaching care in time: the barriers of distance and cost prevent manywomen from reaching the health facility in time. In rural areas, distances betweencommunities and health centres can be very long and roads are poor. Bicycles anddonkey carts are often the only available means of transport.
� Delay in receiving adequate treatment: inadequate provision of health servicesand a frequently poor and slow referral system combine to delay life-saving treatment.
The barrier of cost is often critical as in many emergency cases women and theirfamilies are asked to pay large sums for medicines and supplies that are official yfree of charge or subsidized.
While the government has made efforts to reduce these delays, the high rate ofmaternal deaths in Burkina Faso shows that women are being denied their right tohealth, a right enshrined in international and national law, a right that every state isobliged to respect, protect and fulfil. When women die in pregnancy or childbirthbecause the government fails to address preventable causes of maternal death, thegovernment violates women's right to life.
Poverty is a key factor in maternal mortality. Burkina Faso is ranked as one of thepoorest countries in the world,11 with 46.4 per cent of its population living below thenational poverty line12 and 80 per cent living in rural areas where the infrastructureis often inadequate.
However, this cannot justify the government's failure to meet its obligation to takesteps to the maximum of its resources to realize the right to health (including sexualand reproductive health) for al its population, notably those living in poverty. In its2008 report to the Human Rights Council's Working Group on the Universal PeriodicReview, the government of Burkina Faso recognized its responsibility to respect andrealize fundamental economic, social and cultural rights, while stressing the economicconstraints it faces. It stated, "While underdevelopment should not be considered an
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
excuse for a State not fulfil ing its responsibility to realize human rights, it must beacknowledged as a real brake and genuine constraint on the realization of manyrights."13
In its fight against maternal mortality, the government of Burkina Faso is supportedby the donor community which contributes to the health budget and also supportsspecific projects aimed at improving access to health care. This report acknowledgesthe efforts to address maternal mortality undertaken by the government with the helpof the donor community, as wel as projects led by international and national NGOs.
OBJECTIVES OF THIS REPORT
This report examines preventable maternal mortality as a violation of the right to healthand ultimately of the right to life. It focuses on:
� The need to respect and ensure women's right to gain access to sexual andreproductive services;
� The need to dismantle the barriers that obstruct women's access to adequatehealth care, including barriers of cost that continue to deter or prevent the poorestwomen from benefiting from skil ed assistance at the time of delivery and emergencyobstetric care when necessary;
� The need to improve the quality of care by ensuring skilled attendance atdeliveries, within an environment capable of providing care for normal deliveries andemergency obstetric care when complications arise;
� The need to ensure accountability of the government in respect of its obligationto devote the maximum possible resources to ensure the highest attainable standardof health for al pregnant women, in particular ensuring that emergency obstetric careand skil ed birth attendance are available, accessible, acceptable and of good qualitythroughout the country, including in rural and poor areas.
In conclusion, the report presents recommendations to the government, theinternational community and donors to entrench progress and tackle maternalmortality with greater consistency and, more generally, to enhance respect forwomen's rights. Amnesty International calls for improvements in access to andinformation about sexual and reproductive services and health; the removal offinancial barriers to health services, especial y for the poorest; and improvements inthe quality of care and training of medical personnel so that the right to health forwomen is ful y respected.
This report is based on four fact-finding missions to Burkina Faso since July 2008 andon the work of a consultant who carried out research for three months in the country.
Amnesty International visited health facilities and met medical personnel in severalcities including the capital, Ouagadougou, as wel as Bobo-Dioulasso, Ouahigouyaand Kaya. Amnesty International also visited a dozen rural areas throughout thecountry.
In the course of its research Amnesty International investigated more than 50 casesof women who died during pregnancy and childbirth. Its delegates interviewed familymembers, health care staff, and members of the community, and col ected hospitaland health care records on the cases where available. Amnesty International alsospoke to ministers and staff from the Ministries of Health, of Human Rights, ofPromotion of Women and of Finance, staff from UN agencies, national andinternational NGOs, bilateral and multilateral donors, as well as researchers andpublic health specialists.
This study focuses only on public health facilities – there are also private healthstructures operating in the country.14
Statistics mentioned in this report are drawn mainly from official data sources, notablythe Demographic and Health Survey (DHS), published every five years.15 Every yearthe government publishes detailed statistics on the health sector,16 but these figureshave to be treated with caution since many people, especial y in rural areas, do notuse the formal health system when they are sick and do not declare births and deaths.
Therefore the official statistics (including those based on hospital figures) only give apartial picture of the real situation in the country. This report uses UN statistics onlywhen national figures are not available.17
Several independent specialists have read and commented on this text on a voluntarybasis, including scholars Véronique Filippi from the London School of Hygiene andTropical Medicine, Fabienne Richard from the Institute of Tropical Medicine inAntwerp and Valéry Ridde from the University of Montreal (CRCHUM).
For the sake of confidentiality and to protect witnesses and contacts, al names andlocations have been changed or omitted.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
2/WOMEN'S STATUS IN
‘FOR MEN, A WOMAN IS ONLY A TOOL FOR REPRODUCTION'A woman from the vil age of Gorgaré, June 2009
The government has adopted many laws aimed at improving the status of womenand has ratified the relevant international treaties. However, women in Burkina Fasocontinue to suffer from discrimination in every area of their lives. Particularly in ruralareas, women have little or no say in key domestic decisions.
Burkina Faso's Constitution and laws prohibit al forms of discrimination, including ongrounds of gender. However, there is no specific legislation that defines whatconstitutes discrimination against women and the legal provisions assuring women'sequality have had limited impact, due notably to the continuing influence of religiousand customary laws.18 Religious and customary laws have official y had no legal effectin family relations since the adoption of the 1990 Individual and Family Code (Codedes personnes et de la famille). However, the government has acknowledged:"the persistence of certain traditional and religious practices that put women at adisadvantage, including the levirate [the practice of marrying a widow to her deceasedhusband's brother], under age and/or forced marriage, excision [female genitalmutilation] and the reluctance to send girls to school."19
The 2005 Concluding Comments of the UN Committee on the Elimination ofDiscrimination against Women (CEDAW Committee) stressed the Committee'sconcerns about: "the continuing strong prevalence of patriarchal attitudes and deep-rooted stereotypes and of customs and traditions that discriminate against women,particularly women in rural areas, and constitute violations of their human rights."20
Women are marginalized in many areas of society and have unequal access toeducation, health care and employment. In 2007, the literacy rate for women and girlswas only 21 per cent, compared to 36.7 per cent for men and boys.21

WOMEN'S STATUS IN BURKINA FASO
Ini Damien, who founded an organization that works toimprove women's quality of life in the region of Gaoua,Burkina Faso. This NGO promotes knowledge ofreproductive and health rights, addressing both menand women, using the medium of theatre.
WOMEN'S STATUS IN THE FAMILY
Women are primarily valued as wives and mothers, especially in rural areas.
Unmarried women are seen as il -fated and of little worth. Married women withoutchildren face discrimination and are at risk of being abandoned or rejected by theirhusbands and in-laws.
There are heavy cultural pressures from the community on women to have manychildren, seen as a sign of wealth. This is especial y true in rural areas where thefertility rate is 6.9 children per woman, as compared with 3.7 in urban areas. Thenational average is 6.2.22

GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Ramatoulaye and her baby daughter by the Nakamberiver close to Wonko, Burkina Faso. Four months earliershe was forced to give birth on the river bank becausethere was no boat available to take her across.
Fatou was subjected to domestic violence because all her children were girls.
Fatou, a housewife and petty trader living not far from Bobo-Dioulasso, had a very difficultlife with her husband because he was unhappy with her for only giving birth to girls. Shehad seven pregnancies and gave birth to five girls. At the birth of one of her daughterssome years ago, Fatou asked the medical personnel and the women accompanying hernot to reveal the baby's sex until her husband had paid the bills. When he learned thatit was a girl, he left, very angry. Later on, her husband took a second wife who gave hima son. While under customary rules the first wife retains a prominent place, Fatou wasforced to play a secondary role in the family.
In 2007, at the age of 41, Fatou again became pregnant. After a sonogram revealed thatshe was expecting another girl, her life became even more difficult. A friend told AmnestyInternational in March 2009: "Her husband continuously yelled at her. Life was notbearable anymore and she decided to flee her home and found refuge at my home inOuagadougou. The journey took six hours by bus and she arrived exhausted and afraidin the evening." Fatou eventually died in childbirth at the university hospital inOuagadougou.
WOMEN'S STATUS IN BURKINA FASO
‘THE FIRST TO GET UP IN THE MORNING AND THE LAST TO GO TO SLEEP'
Amnesty International col ected many testimonies describing the hard daily lives ofwomen, especially in rural areas where they are generally expected to bear theirnormal workload while pregnant or just recovering from childbirth.
Sarata died in childbirth, having worked until the last day of her pregnancy.
Sarata lived in a rural area not far from Ouagadougou, and was married at the age of 17.
None of her first four children survived for more than six months. She became pregnantagain at the age of 26 in 2006 – her fifth pregnancy in nine years.
Her friend told Amnesty International: "She worked until the very last day of herpregnancy helping her husband with the farming, which normally begins around 7am.
But beforehand, she prepared the meal, at around 6am. When she got back from thefields around 2pm, she had her meal and then rested for a moment before returning towork in the field until 6pm. Outside of the rainy season, she used to sell pancakes at themarket. During her pregnancy, I asked her to rest, but she responded that she could not,because she would be teased for not having any children."
She worked until the very last day before delivering and had no time to go to the CSPS.
One night she had pains and a while later, around 4am, she gave birth in her home. Shewas taken by motorcycle to the CSPS and then to the university hospital in Ouagadougouwhere she was diagnosed with puerperal infection (an infection that occurs afterchildbirth, due to poor sanitary conditions), severe malaria and eclampsia. She died onarrival at the hospital, before receiving any treatment.
FEMALE GENITAL MUTILATION
The practice of female genital mutilation (FGM, or excision) has been prohibited bylaw in Burkina Faso since 1996 (under Articles 380 to 382 of the Penal Code) andwomen accused of practising FGM are from time to time prosecuted and sentencedto prison terms. However, due to the persistence of traditional practices and customs,it is stil practised clandestinely in insanitary conditions, and is a major cause of deathand disability.23

GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Fatimata cycles to get water at the end of the day.
Women, especially in rural areas, are expected tocontinue their normal work regardless of pregnancy andchildbirth.
Some studies indicate that the practice of FGM can lead to difficulties in labour andother complications of pregnancy. For example, the WHO study group on femalegenital mutilation and obstetric outcome found that: "deliveries to women who haveundergone FGM are significantly more likely to be complicated by caesarean section,postpartum haemorrhage, episiotomy, extended maternal hospital stay, resuscitation ofthe infant, and inpatient perinatal death, than deliveries to women who have not hadFGM."24
EARLY MARRIAGES AND PREGNANCIES
Early marriages have serious consequences for girls; they lessen the chance of girlsattending school while increasing the risk of early and life-threatening pregnancies.
Since 1990, marriage and family matters have been governed by the Individual andFamily Code. Article 238 sets the minimum age of marriage at 17 for girls and 20 forboys, which may be reduced to 15 for girls and 18 for boys.25 In its 2004 report, the
WOMEN'S STATUS IN BURKINA FASO
CEDAW Committee stressed its concerns "about the persistence of severaldiscriminatory provisions in the [Individual and Family] Code, particularly in relationto the minimum age of marriage."26
This provision only applies to civil marriages. In rural areas, many people marryaccording to traditional rules with no minimum age, and girls as young as 10 areoften married. An official study recently found that the age of marriage was most oftenbetween 10 and 19, although the majority of teenagers living as a household weremarried when they were between 14 and 19.27 In addition, young women in ruralareas are more likely to bear children, with 157 per thousand rural adolescentsbecoming mothers, compared with 64 per thousand in urban areas.28
Early pregnancies entail a number of risks. Young girls who bear children before theirpelvises are ful y developed often suffer complications, including obstructed labour.
Where these complications do not result in death, they may cause chronic injurysuch as fistula – perforations in the birth canal that permit leakage from the bladderor rectum into the vagina.29
POLYGAMY AND FORCED MARRIAGE
Polygamy is legal and widespread in Burkina Faso. Article 232 of the Individual andFamily Code provides that monogamy is the common law form of marriage andpermits polygamy only when the spouses agree to that option before the weddingceremony. But when women cannot in reality take any important decision within thecouple, it is the man who chooses whether a marriage will be monogamous orpolygamous.
Forced marriages are forbidden by law: Article 16 of the Individual and Family Codeenshrines the right of men and women to choose their spouse. However, asacknowledged by the government in 2004, "In reality forced marriages are commonowing to ignorance of the relevant rules by victims and the constraints of customs,religion and other factors."30
The custom of the levirate, under which a widow has to marry a relative (usual y thebrother) of her late husband, is prohibited by the Individual and Family Code andthe Penal Code. Despite this, it is stil practised in Burkina Faso, especial y in ruralareas.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
WOMEN'S LACK OF POWER
Although women have equal status under the law,31 in practice most are subordinateto the men in their lives and are unable to make key decisions, including the timingand spacing of their pregnancies. Women are embedded in a vicious circle with littleaccess to education or to information on sexual and reproductive rights, and aresubject to early marriages, female genital mutilation and polygamy as wel as beingexpected to work long hours while pregnant or after childbirth.
Women are wel aware of the dangers of pregnancy, as nearly everyone knows arelative or friend who died or suffered complications in pregnancy and childbirth.
Several women told Amnesty International that young girls in rural areas used to wisheach other "not to have the misfortune of being pregnant". However, their access toinformation on reproductive rights and services is extremely restricted.
Women's lack of power, linked to economic dependence and subordinate status,means that women who need their husband's permission and funds to obtain healthcare have to adopt bargaining strategies. In a qualitative study published in 2007,three researchers identified the techniques adopted by women in Burkina Faso:"Typical y, the process is gradual. First, they wil adopt strategies that respect thehusband's authority; only when these have been exhausted would they resort todefiance."32 These bargaining strategies include offering to make a contribution (if thewife has savings), turning to mediation through in-laws, and confrontation, where thewoman reminds her husband of his responsibilities towards her or threatens to returnto her parents. As a last resort, the woman can return to her family's home, but asthe authors of the study stressed: "Confrontation occurs from time to time. Returningto the paternal home is rare."33
In order to make pregnancy and childbirth safer, the government of Burkina Fasohas to move beyond formal equality before the law and make greater efforts to givewomen access to information and education in order to empower them to claim theirrights and the public services they are entitled to.
In the absence of government leadership, a growing number of women in BurkinaFaso have created NGOs in the last two decades to inform women of their rights,especial y their sexual and reproductive rights. These NGOs include professionalorganizations of nurses and midwives as wel as associations of women activists.
WOMEN'S STATUS IN BURKINA FASO
Examples of NGOs raising awareness of sexual and reproductive rights
The Women's Promotion Association (Association pour la promotion féminine), foundedin 1992 by Ini Damien, a schoolteacher, has more than 400 members working to improvewomen's quality of life. This NGO promotes knowledge of reproductive and health rights,addressing both men and women, using the medium of theatre. Ini Damien told AmnestyInternational in June 2009: "The government's messages of awareness have not gonethrough in a population which remains deeply illiterate."
Juliette Compaoré, who also created an NGO for the defence of women rights, had herselfbeen confronted by traditional rules which restrict women's freedom. "My uncle wantedto impose a husband on me but I refused because he was not the man of my choice. Thenproblems started because I was ‘the peasant who refuses the prince' as my uncle said.
It drove me to create a NGO for the promotion of women's rights because I realized thatthe Ministry of Health does not have the means to lead a communication policy amongthe population." Juliette Compaoré created in 1994 the organization ASMADE,34 whichhas campaigned to raise awareness on sexuality among young people and to promote theadoption of the Law on Reproductive Health. "We fight now so this law is made a realityso all women have their say on matters of reproductive health."
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
3/GOVERNMENT POLICIES
‘THE REDUCTION OF MATERNAL MORTALITY IS A PRIORITY'Ministry of Health of Burkina Faso, 2006 "Roadmap"35
The authorities have given special attention to combating maternal mortality. Theirpolicies, strategies and actions were developed and implemented in the context ofMillennium Development Goal 5 (MDG-5) adopted by the UN in 2000.36 Thisstipulates a reduction in maternal mortality of 75 per cent by 2015, which for BurkinaFaso would mean achieving a maternal mortality ratio of 142 deaths per 100,000 livebirths.37 However, in its 2003 report on progress towards the MDGs, the governmentstressed that "this international goal seems very ambitious for Burkina Faso which,considering the strategies it wishes to develop, aspires to reach a ratio of 209 deathsper 100,000 live births by 2015."38
INCREASING BUDGET ALLOCATION
For the past decade the authorities in Burkina Faso have devoted increased financialresources to the health sector. In 2001, the authorities committed themselves to"increase the portion of the health budget in the total budget by 10 per cent per yearuntil it reaches 12 per cent."39 The proportion of the budget al ocated to health grewfrom 6.3 per cent in 2001 to 8.42 per cent in 2008.40
Budget figures for 200641
7.8 per cent of the total budget
� Reproductive health budget42
5.99 per cent of the health budget,0.47 per cent of the total budget
� Maternal health and family
4.67 per cent of the reproductive
health budget, 0.02 per cent of thetotal budget
11.44 per cent of the reproductive healthbudget, 0.05 per cent of the total budget
GOVERNMENT POLICIES
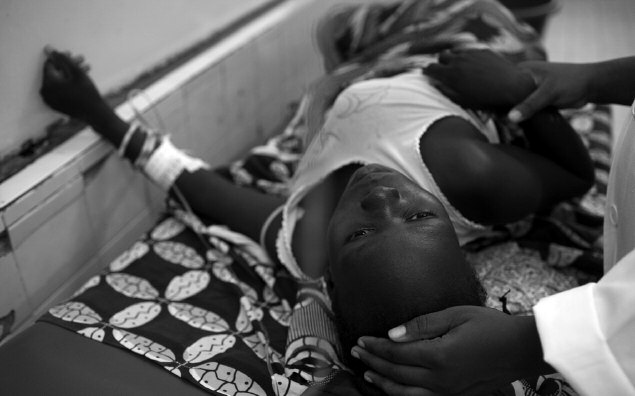
An 18-year-old woman in severe pain is calmed by amedical student while she waits for a caesarean.
During the operation, in which her daughter was safelydelivered, the birth cord was found to be tightlywound around the baby's neck. Yalgado Hospital,Ouagadougou, Burkina Faso.
However, the authorities have recognized that the percentage of the health budget"remains under the WHO standard (10 per cent)."43 Moreover, it remains far behindthe 15 per cent goal set by the African Heads of State at the AU Summit in Abuja in2001.44
The government's current health policy stems from the National Health Policy adoptedin September 200045 and its implementation plan, adopted in July 2001, the NationalHealth Development Plan (PNDS, Plan national de développement sanitaire 2001-2010). The aim of the Plan is to reduce morbidity and mortality through eight globalobjectives such as increasing the coverage of national health services, improving thequality, financial accessibility and use of health services, and improving themanagement of human resources in the health sector.46
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Official goals and results according to governmental statistics
The National Health Development Plan (PNDS) set up the following goals to reducematernal mortality. In 2008, some of them had been met, according to official statistics.
40 per cent reduction in maternal mortality.
The maternal mortality ratio went from 484 per 100 000 live births in2001 (DHS 2003) to 307 per 100,000 live births in 2008 (RGPH 2006),a 36.5 per cent reduction.
Increase in women undertaking prenatal visits from 65 to 90 per cent.
By 2008 75.25 per cent of pregnant women undertook at least oneprenatal visit.
An increase in assisted births from 34 to 60 per cent.
In 2008, the level of assisted deliveries was 65.19 per cent.
An increased prevalence of contraceptive use from 6 to 17 per cent.
Although showing an increase, figures differ on contraceptive prevalence(see Chapter 5).
It should be noted that these official statistics are incomplete, in particular because ofgaps in information on rural areas and the failure to record births and deaths that takeplace outside medical facilities.
In order to increase the coverage of national health services, the National HealthDevelopment Plan provides that in rural areas there should be one CSPS (Centre desanté et de promotion sociale, community health centre) per 10km radius, and inhighly populated areas, one per 10,000 inhabitants. The Plan also contains provisionsto improve the quality of health personnel, through the redeployment of personnel,the implementation of incentives, punishing misconduct, the development of trainingprogrammes and the creation of an ethics committee. Lastly, the Plan provides thatgeneric drugs should be made more available through better supervision of the supplyand distribution of medicines in al districts.47
In a landmark move to reduce the economic obstacles to women's access to healthcare, the government adopted in 2006 a subsidy policy for childbirth and emergency
GOVERNMENT POLICIES
obstetric care, including caesarean sections. This subsidy strategy – the Nationalstrategy of subsidy for deliveries and emergency obstetric and neonatal care48 – wasfostered and facilitated by the World Bank and is one of the priority actions of thePoverty Reduction Strategy Framework adopted by the government in 2000.49 Itsmain purpose is to limit the impact of payments for medical care on the incomes ofpoor households.
Under the subsidy strategy, women are entitles to have the costs of deliverysubsidized by 80 per cent, indigent women (women living in extreme poverty) shouldreceive free care in childbirth, and transport between different health facilitiesshould be free for al women in labour (see Chapter 7).
Within the framework of its health care policy, the government of Burkina Fasoprioritized the extension of geographical coverage by increasing the number of CSPSfrom 798 in 2000 to 1,352 in 2008.50 This reduced the average distance to a healthfacility from 9.4km in 2000 to 7.5km in 2008.51
However, there are stil enormous disparities between urban and rural areas (seeChapter 6).
The government of Burkina Faso is resolutely in favour of using exclusively genericmedicines. In 1992, a central drug procurement and distribution agency, CAMEG,52was created with the aim of generalizing the use of generic medicines and improvingthe supply of drugs in rural areas. The quality of these medicines is regularly checkedand their use plays a key role in the government's efforts to control health costs.
Under this policy, al public health facilities receive generic medicines distributed bythe CAMEG and cannot sel non-generic branded medicines.
ORGANIZATION OF THE HEALTH SYSTEM
The health care system in Burkina Faso is divided along administrative borders into13 regions and 63 health districts. Each district covers a population of 150,000 -200,000 people.
There are three levels of health care: primary, secondary and tertiary.
� Primary health care is provided by the Centre de santé et de promotion sociale(CSPS, Health and Social Promotion Centre) at the community level and by the Centremédical avec antenne chirurgicale (CMA, Medical Centre with Surgical Services -hereafter district hospital) at the district level. The CSPS provides maternal and childhealth care as wel as running prevention and promotion activities. The district hospital
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
The delivery room at Kiembara health centre, BurkinaFaso. More than a third of all births still take placewithout medical assistance.
is the first reference level for pregnant women with complications. In 2008, therewere 1,352 CSPS and 42 district hospitals.53
� Secondary health care is provided by nine Centres hospitaliers régionaux (CHR,hereafter regional hospitals) which are referral hospitals.
� Tertiary health care is provided by three Centres hospitaliers universitaires (CHU,hereafter university hospitals) – two of which have maternity units, one inOuagadougou and one in Bobo-Dioulasso, the country's second largest city.54
There are also some private clinics and treatment institutions, especial y in the cities.
The three-level health system was facilitated by a policy of decentralizationimplemented by the government since the early 1990s. National and regionalhospitals have progressively been given greater autonomy in terms of financial andpersonnel management. In 1994, hospitals and health centres were al owed to retainfunds collected from fees and the sale of drugs. Elected local Health ServiceManagement Committees,55 COGES, were set up. These committees are composedof members of the community, including women,56 with medical personnel as
GOVERNMENT POLICIES
advisers, and are responsible for the management of the retained funds. Twice a yearthese Committees have to account to the community and are audited by a DistrictManagement Team including an account supervisor and a chemist.
TRADITIONAL BIRTH ATTENDANTS AND AUXILIARYMIDWIVES
The government has developed in recent years a new policy towards traditional birthattendants ("matrons" or accoucheuses vil ageoises), who assist women giving birthwithin the community. In December 2007, the Ministry of Health stated that itintended to "refocus" their role from carrying out deliveries to preparing women forchildbirth by identifying the place of delivery, namely the nearest CSPS, and bymaking sure that reliable transport is available to take the woman to the health centrefor the birth or in case of complications.57
In order to improve the quality of care at the local level, the authorities also decidedto deploy auxiliary midwifes (accoucheuses auxiliaires) in every CSPS. Auxiliarymidwives require a basic elementary school-leaving qualification58 and receive twoyears' training at the national school of public health.59 The auxiliary midwifes carryout prenatal check-ups, in the course of which they identify and treat symptoms ofmaternal problems such as high blood pressure, anaemia and malaria, and they areresponsible for normal deliveries60 in the CSPS. They have to be capable ofrecognizing the signs of complications during childbirth, so that they can refer thewoman to a higher level health facility as quickly as possible.
In December 2007, the government also published a plan to set up village-levelmanagement teams for obstetric and neonatal emergencies in some pilot zones.
These teams of two or three community members would be responsible for raisingawareness of danger signs and enhancing preparations for childbirth by families andthe community. They would also work to improve the referral system by developingcommunications and transport to reduce delays in transfers.61
These efforts succeeded in increasing the number of medical y assisted deliveries –the official proportion of assisted deliveries rose from 37.7 per cent in 2005 to65.19 per cent in 2008, according to official figures.62 While this is positive, morethan a third of al deliveries stil take place without medical assistance, with a muchlower proportion of medical y assisted deliveries in rural areas.63
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
4/THE HUMAN RIGHTS FRAMEWORK
‘HEALTH IS A FUNDAMENTAL HUMAN RIGHT INDISPENSABLE FOR
THE EXERCISE OF OTHER HUMAN RIGHTS. EVERY HUMAN BEING IS
ENTITLED TO THE ENJOYMENT OF THE HIGHEST ATTAINABLE
STANDARD OF HEALTH CONDUCIVE TO LIVING A LIFE IN DIGNITY.'UN Committee on Economic, Social and Cultural Rights, General Comment 14, para 1
The obligation on states to progressively realize the right to the highest attainablestandard of health is enshrined in various international and regional instruments towhich Burkina Faso is a party. The treaties ratified by Burkina Faso that guaranteethe right to health include the International Covenant on Economic, Social and CulturalRights (ICESCR), the Convention on the Elimination of Al Forms of Discriminationagainst Women (CEDAW), the Convention on the Rights of the Child and the Protocolto the African Charter on Human and Peoples' Rights on the Rights of Women inAfrica (the Maputo Protocol).
The preamble to the Constitution of Burkina Faso refers to the Universal Declarationof Human Rights (UDHR) and reasserts the country's commitment to internationaltreaties and to the African Charter on Human and Peoples' Rights (ACHPR). Articles1 and 26 of the Constitution of Burkina Faso confer on every person the right to lifeand the right to health.
THE RIGHT TO HEALTH
The Committee on Economic, Social and Cultural Rights (CESCR) has stated that theright to health requires that health and health care facilities, goods and services beavailable, accessible, acceptable and of good quality.64 This means that:
� A sufficient quantity of health facilities, trained professionals and essentialmedicines must be available.
� Health facilities, goods, services and information on health must be physical yand economical y accessible (within easy reach and affordable) to everyone withoutdiscrimination.
THE HUMAN RIGHTS FRAMEWORK
� Health facilities, goods, services and information must be acceptable, that isrespect medical ethics, be culturally appropriate and sensitive to genderrequirements.
� Health facilities, goods, services and information must also be scientifical y andmedical y appropriate and of good quality. This requires, among other things, skil edmedical personnel, scientifically approved and unexpired drugs and hospitalequipment and adequate sanitation.
PREVENTABLE MATERNAL MORTALITY IS A VIOLATION OFTHE RIGHT TO LIFE
Preventable maternal mortality is also recognized as a violation of the right to life asenshrined in the International Covenant on Civil and Political Rights (ICCPR). TheHuman Rights Committee urges states to take positive measures to safeguardindividuals from arbitrary and preventable losses of life.65 This includes steps to protectwomen against the unnecessary loss of life related to pregnancy and childbirth66 byensuring that health services are accessible.67 In addition the CEDAW Committee hasissued a number of General Recommendations that further develop this right. In itsGeneral Recommendation on Health, it states that women's access to health careservices, "particularly in the areas of family planning, pregnancy, confinement andduring the post-natal period"68 is imperative. The Committee's recommendationssupport the claim that there is a governmental duty to ensure that al women haveaccess to maternal care, pre and postnatal care, emergency obstetric care, andfamily planning.
MATERNAL HEALTH IS A RIGHT
The right to maternal health is part of the right to health. The UDHR, the ICESCR, theCEDAW, the ACPHR and the Maputo Protocol specifical y obligate governments toprotect maternal health.69 Under these agreements, the state has an immediate dutyto ensure that the right to health is realized and enjoyed without discrimination of anykind by providing access to "a ful range of high quality and affordable health care,including sexual and reproductive services."70
The ICESCR contains the most comprehensive provisions regarding this right. In itsArticle 10(2), it states that "special protection should be accorded to mothers duringa reasonable period before and after childbirth."
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
In November 2008, the African Commission on Human and Peoples' Rights adopteda resolution to address maternal mortality in Africa.71 The resolution acknowledgedthat preventable maternal mortality in Africa is a violation of women's right to life,dignity and equality as enshrined in the ACHPR and the Maputo Protocol. It cal s onAfrican governments to address, individual y and col ectively, the issue of maternalmortality.
THE RIGHT TO NON-DISCRIMINATION
Most human rights treaties guarantee women the right to equality and non-discrimination. Pregnancy and childbearing impose "inequitable burdens" on women,particularly in relation to access to education and employment. This perpetuateswomen's inequality, which is further reinforced by discriminatory practices such asearly marriage and stereotyped views on women's role as procreators. The CEDAWstates that "the role of women in procreation should not be a basis fordiscrimination."72
Article 12 of the CEDAW requires states to "eliminate discrimination against womenin the field of health care in order to ensure, on a basis of equality of men and women,access to health care services."73 Women suffer from both direct and indirect formsof discrimination in attempting to obtain health care. Certain groups of women facenot only gender discrimination, but discrimination on such bases as economic status,geographic location and age. Under Article 14 of the CEDAW, governments mustmake special efforts to ensure that women in rural communities are notdisadvantaged, particularly regarding "access to adequate health care facilities,including information, counsel ing and services in family planning."74
In addition, the ACHPR declares that al individuals are "equal before the law" andrequires states to "ensure the elimination of every discrimination against women andalso ensure the protection of the rights of woman and the child as stipulated ininternational declarations and conventions."75 The Maputo Protocol also cal s uponstates to reform laws and practices that discriminate against women.
Furthermore all children are entitled to enjoy the highest attainable standard ofhealth,76 just as adults are,77 and the Convention on the Rights of the Child explicitlyguarantees children the right to be free from discrimination.78 Under the principle ofnon-discrimination, adolescents should enjoy the same rights to reproductive healthservices as adult women.
THE HUMAN RIGHTS FRAMEWORK
SEXUAL AND REPRODUCTIVE RIGHTS
Sexual rights are human rights and are recognized in international human rightsstandards.79 They include the right of al people, free of coercion, discrimination andviolence, to the highest attainable standard of sexual health, including access tosexual and reproductive health care services.
Everyone is entitled to:
� seek, receive and impart information related to sexuality
� education related to sexuality
� respect for bodily integrity
� choose their partner
� decide to be sexual y active or not
� consensual sexual relations
� consensual marriage
� decide whether or not, and when, to have children
� pursue a satisfying, safe and pleasurable sexual life
Reproductive rights enable al people to decide freely the number, spacing and timingof their children and to have the information and means to do so. They also guaranteeal people the right to attain the highest standard of sexual and reproductive healthfree of discrimination, coercion and violence. These rights relate to access toreproductive health services and information, safe pregnancy and childbirth,prevention and response to unwanted pregnancy, and freedom from forcedsterilization, contraception or abortion.
Sexual and reproductive rights are central to the realization of every individual'shuman rights. Respect for these rights is essential to human dignity and to theenjoyment of physical, emotional, mental and social well-being. Their fulfilmentenhances life and personal relationships and helps to achieve gender equality andempowerment. Al people must be al owed to enjoy their sexual and reproductiverights free of coercion, discrimination and violence.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
5/FAMILY PLANNING
‘IF UNMET NEEDS WERE SATISFIED, CONTRACEPTIVE PREVALENCE
COULD REACH 43 PER CENT OF WOMEN OF CHILDBEARING AGE;
I.E. THREE TIMES HIGHER THAN THE ACTUAL RATE.'Ministry of Health, January 200980
More than 5,000 women died in Burkina Faso between 1995 and 2000 as a resultof pregnancies that were unintended,81 according to a statistical analysis publishedin 2002.82 Such a large number of deaths is strongly correlated throughout the worldwith inadequate access to family planning information and services as wel as earlyand forced marriages. Early, mistimed and unwanted83 pregnancies contribute greatlyto the health risks for both the woman and the baby. Faced with an unwantedpregnancy, many women, especially unmarried girls, resort to unsafe and life-threatening abortions.
Ensuring access to voluntary, safe and effective family planning and contraceptivemethods is therefore a vital part of any strategy for reducing maternal mortality. TheCEDAW guarantees the right of women, on the basis of equality with men, to decidefreely and responsibly on the number and spacing of their children and to haveaccess to the information, education and means to enable them to exercise theserights.84 The CEDAW Committee has emphasized the obligation of states to "prioritisethe prevention of unwanted pregnancy through family planning and sex educationand reduce maternal mortality rates through safe motherhood services and prenatalassistance."85
The government of Burkina Faso has acknowledged the importance to every humanbeing of enjoying her or his sexual and reproductive rights. In December 2005, itadopted a Law on Reproductive Health86 that enshrines these rights. This law statesthat "The right to reproductive health is a fundamental right guaranteed to eachhuman being during her or his entire life, in al situations and in al places" (Article8) and that "couples and individuals decide freely and responsibly the number ofchildren they have as wel as the spacing of their births" (Article 9). Four years afterthe adoption of this law, the government passed two decrees on the creation of privatereproductive health structures and on the production and import of contraceptiveproducts.87
A 45-year-old mother of five in the recovery ward aftera caesarean to remove her twins who had died due tocomplications at seven months. Yalgado Hospital,Ouagadougou, Burkina Faso.
In practice, although modern contraception was introduced in Burkina Faso in the late1980s, its use remains very limited, especially in rural areas. The inadequacy ofsexual and reproductive health services in Burkina Faso was noted by the CEDAWCommittee in 2005, when it cal ed on the government "to improve the availability ofsexual and reproductive health services, including family planning… [and to] enhanceavailability of contraceptive services."88
In December 2005, the government adopted a Contraceptive Security Strategic Plan(2006-2015). Its main objectives include the state gaining independence from donorsin the purchase of contraceptives, guaranteeing that contraceptives are available toal women and that family planning services are of good quality.89 A broader plan foral products related to reproductive health, the Reproductive Health Products SecurityStrategic Plan (2009-2015), was adopted in June 2009 and assessed theachievements to date and the remaining gaps in this area (see Chapter 10). Itemphasized the use of female condoms as a way to improve reproductive health.90As a result, training programmes on this method of contraception have started insome regions, with dummies purchased in order to demonstrate their use.91
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
USE OF CONTRACEPTIVES REMAINS LOW
While there is great variability and uncertainty in the statistics on contraceptive use,al available figures indicate that the proportion of women who use contraception hasat least doubled in the last 15 years. The DHS 2003 found that the rate had risen from8 per cent in 1993 to 14 per cent in 2003. This survey stated that only 14 per centof women in a relationship (one in seven) were using some method of contraceptionat the time of the survey: 9 per cent were using a modern method, primarily injections(3 per cent) and the contraceptive pill (2 per cent) and 5 per cent were using atraditional method, primarily periods of abstinence (3 per cent).92
Figures published recently by the UN indicate that the contraceptive prevalence rateis 17 per cent for women aged between 15 and 49.93
This low rate means that the contraceptive needs of many women remain unmet. Inits report to the CEDAW Committee submitted in February 2004, the Burkina Fasogovernment estimated that 42.4 per cent of married women had an unmet need forcontraception.94
BARRIERS TO THE USE OF CONTRACEPTIVE SERVICES
An auxiliary midwife working at a rural CSPS told Amnesty International in March2009 that:
population. In rural areas, women of childbearing age often don't know themethods of modern contraception or they don't trust them as they are afraid
of becoming sterile or of being affected by other side effects. In fact, many womenin rural areas want a high number of children as this is beneficial in the traditionalsocial and economic organization but they want the pregnancies to be spaced; soinstead of modern contraception, they prefer post partum abstinence and usenotably a natural method called "le collier" [the necklace – a string of plastic beadsof different colours representing the fertile and infertile days of the menstrualcycle]. Cost can be another obstacle. Some women attend the initial consultationbut don't return after that because they have to pay for the products and they don'tdare ask their husband. Husbands are often an obstacle because some men believecontraception leads to infidelity. Fertility is one means of monitoring women'sfidelity."
This testimony highlights some of the overlapping barriers to women's access tocontraception in Burkina Faso. As wel as lack of information, often giving rise tomisplaced fears, there are cultural barriers, notably the opposition of husbands and
the social condemnation of extramarital sexuality. In focus groups organized byAmnesty International, both married and adolescent unmarried women describedwomen suspected of having sexual relations before marriage as "dévergondées"(loose or debauched). There are other structural barriers: the inadequate quality offamily planning services, the lack of availability and cost of contraceptive productsand, at least until recently, a lack of funding by the government and the donors whohad other priorities.
INADEQUATE INFORMATION ON SEXUAL AND REPRODUCTIVE RIGHTS
Official statistics indicate that knowledge of modern contraception has increased.
According to the DHS 2003, in 1993, 63 per cent of married women said they knewabout modern contraceptive methods, rising to 89.4 per cent in 2003, and 91.1 percent among men.95 However, this stated knowledge does not mean that women areable to use these methods, especial y in rural areas. This is confirmed by the DHS2003: "Contraceptive prevalence for al the methods is 3.4 times higher in urbanzones (34 per cent) than in rural areas (10 per cent) and more than 5 times higheras regards the modern methods (28 per cent against 5 per cent)."96 The DHS alsoshows that women with a higher level of education are more likely to usecontraception.97
However, information col ected by Amnesty International indicates that many womenstil suffer both from a lack of general information on sexual and reproductive rightsand on specific medical information related to contraception methods. A largenumber of women interviewed by Amnesty International, especial y in rural areas,had not heard of the Law on Reproductive Health or were unfamiliar with its mainprovisions, notably the right "to decide freely and responsibly the number of childrenthey have as well as the spacing of their births."98 Moreover, some people toldAmnesty International that they were finding it difficult to get information aboutcontraception from medical personnel or family planning services.
Although the right to information about family planning is enshrined in the 2005 Lawon Reproductive Health,99 the government has not launched the nationwide,comprehensive awareness raising campaign needed to make this a reality. TheContraceptive Security Strategic Plan for 2006-2015 cal ed for a Communication Planto raise awareness on family planning, especial y among men,100 which started in2007. A campaign was carried out to encourage people to use family planningservices and to ral y civil society actors on this issue, but it does not seem to havecovered the whole country.
The lack of information on sexual and reproductive rights and contraception isespecial y key for young people, many of whom told Amnesty International that theydid not have the information they needed about family planning. Several girls who
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
participated in a focus group discussion in Pissy (a neighbourhood of Ouagadougou)said that the classes offered in school were insufficient and overly abstract. Theinadequacy of information for young people was stressed by the CEDAW Committeewhich recommended to the government of Burkina Faso in 2005 "that sex educationbe widely promoted and targeted at girls and boys, with special attention to theprevention of early pregnancies and sexual y transmitted diseases."101 The UN SpecialRapporteur on the right to health has also emphasized that "women should haveequal access, in law and fact, to information on sexual and reproductive healthissues."102
In order to improve the education of the general public, notably young people, localNGOs such as the Association burkinabè pour le bien-être familial (ABBEF, BurkinabèAssociation for Family Welfare) carry out awareness-raising programmes incommunities.
ABBEF: raising awareness among young people
Within the framework of its campaign to promote sexual and reproductive health, ABBEFoffers advice on family planning, gynaecological consultations and confidentialconsultations in the 13 regions of the country.
This NGO has set up Centres d'écoute pour jeunes (Listening centres for young people).
In Koupela, 140 km east of Ouagadougou, for example, teenagers and young people arewelcomed to the listening centre and are given advice in confidence. In 2008, thenumber of people who benefited from this service increased by 27 per cent from 1,397to 1,783. Of the 1,007 adults, 826 were women and of the 776 young people, 680were girls.
QUALITY CONCERNS IN FAMILY PLANNING SERVICES
Women who want information and contraceptive products have to go to local healthfacilities. A male nurse working in a rural CSPS told Amnesty International in June2009:
methods of contraception and, if needed, we make some gynaecologicalexams to see what methods suit them better. At our community level, we can
prescribe them pills or condoms and we can carry out injections and implants. Butwe cannot place an intra-uterine device so we refer them to the nearby districthospital."
However, family planning services are often inadequate both in terms of quality ofinformation and confidentiality. Amnesty International gathered evidence from severallocal NGOs and women indicating that the personnel in charge of informing womenabout contraceptive methods often fail to give sufficient information about the differentmethods and do not tailor their advice to women's individual needs. In a focus groupin Ouagadougou in July 2009, several women said that the public family planningservices were often run by men who tried to deter them from using contraceptives.
They also complained about a lack of confidentiality.
In some cases, medical personnel refused to give information to adolescents becausethey were "too young". An auxiliary midwife working in a rural CSPS told AmnestyInternational in March 2009 that "sometimes medical personnel tel adolescents whocome for a consultation about contraception that it is not for girls their age and thatthey should go home."
During a focus group discussion in Pissy, several young female students said thatthey were reluctant to seek information about family planning in health centres asthey were "likely to meet their parents or neighbours". This is of particular concernfor the young and unmarried women, and for women who do not want their husbandsto know they are seeking contraception.
This lack of privacy is a strong deterrent against seeking contraceptive advice. Theissue of discretion is even more sensitive in rural areas where it is impossible for anadolescent girl to visit a health centre for advice without that fact being known.
Married women with children can seize the opportunity of child consultations to askquestions discreetly.
By failing to ensure that women are able to receive health care services in a mannerthat respects their confidentiality, the government inhibits women's access tocontraceptives.
CONTRACEPTIVE PRODUCTS NOT ALWAYS AVAILABLE
Since the launch of the Contraceptive Security Strategic Plan (2006-2015), thegovernment has made a concerted effort to improve the availability of contraceptivesby contributing a significant part of the budget to the purchase of contraceptiveproducts.103 It has also sought to provide health centres with better teaching andtechnical materials in order to reinforce the skil s of health providers.104
In the CSPSs visited by Amnesty International, contraceptive products wereapparently available and staff said that when there were shortfal s the products wereimmediately ordered and quite quickly provided. But Amnesty International also heardthat in some locations, notably in remote areas, contraceptives are sometimes not
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
available for long periods. Amnesty International learned, for example, that in Koupelaa shortage of male condoms during 2008 seriously undermined family planningcampaigns. These temporary shortages have serious consequences, increasing therisk of sexually transmitted infections, including HIV, as well as unwantedpregnancies. These supply shortages have been acknowledged in the ReproductiveHealth Products Security Strategic Plan, which points to failures in logistics andinformation management leading to "risks of disruption in the supply chain, expiration[of contraceptive products due to delays], damage in transit or overstocking ofcontraceptives." The Plan explains that "there is no national plan for the supplyof products."105
COSTS ARE AN OBSTACLE TO CONTRACEPTIVE USE
The cost of contraceptives is a barrier to women without independent sources ofincome. Although consultations at public health centres are free, contraceptives mustbe purchased at a subsidized price of 25 per cent of the cost. Male condoms cost10 CFA francs each (around US$0.02), female condoms cost 100 CFA francs (aroundUS$0.20), the pil costs 100 CFA francs per monthly pack, injectable contraceptives106cost 500 CFA francs (around US$1, four per year), a contraceptive implant107 costsabout 1,000 CFA francs (around US$2, renewable every three or five years) andan intra-uterine device costs 800 CFA francs (around US$1.60, renewable every10 years).
The information gathered by Amnesty International indicates that the cost of buyingcontraceptives dissuades many women from using them, especial y in rural areas,where women do not have money. A male nurse from a rural CSPS told AmnestyInternational:
"For the poorer populations, the cost of contraceptive products is a real
obstacle. Some women who chose the injections [that need a shot every threemonths] don't come back for the second shot as they couldn't collect the
money. Others choose the pills as it's the least expensive method but it's risky asthey can be lost, forgotten or found by the husband."
Cost is an often insuperable barrier for young girls who depend entirely on theirfamilies. One adolescent in a town 100km north of Ouagadougou said: "I often haveto manage to find the money to buy contraceptives and I have to hide them becausewe [women who use contraceptives] are considered loose."
RESISTANCE FROM HUSBANDS OR OTHER RELATIVES
In many cases documented by Amnesty International, husbands or other male familymembers were opposed to contraceptive use. During a focus group discussion withwomen in Pissy, a 26-year-old mother of four said that she hid her birth control pil sin her kitchen because she knew that her husband never went in there. The choiceof contraceptive product can be determined by the necessity to hide it. A male nursein a rural district said that "many women prefer to choose injectable contraceptiveproducts or contraceptive implant even if it's more expensive as with the pil s thereare daily constraints and it may be very difficult to hide them from their husband."108Amnesty International heard of cases where husbands denounced medical personnelfor providing contraceptive products and advice to their wives. During their visit to arural area in March 2009, Amnesty International's delegates were informed by anauxiliary midwife that the week before a man had come to the CSPS to admonishstaff for prescribing a contraceptive for his wife.
Opposition to contraception is often rooted in the traditional role assigned to womenand the value placed on children as a source of wealth. It is therefore very difficult fora married woman to choose when to have a child. The husband of a woman whodied in April 2008 two weeks after giving birth told Amnesty International:
refused because I wanted to have a baby while I was still young. I also desireda child because I told myself that if I was married, I would take good care of
my wife. I wanted to give my wife a place within my family: when a woman has achild, she can have this place. This is our tradition."
A woman living in Ouagadougou told Amnesty International in March 2009 that:
to use contraceptive methods but my husband refused and told me that if Idid this, I should return to my mother's home. I therefore had to obey him."
These two testimonies show how difficult it is for women to negotiate contraceptiveuse, which is essential to the realization of their sexual and reproductive rights.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
INADEQUATE FINANCING OF FAMILY PLANNING
For many years, family planning programmes in Burkina Faso have been sufferingfrom a lack of financial resources. In its Contraceptive Security Strategic Plan (2006-2015), the Ministry of Health stated: "the financial partners and the government whousual y provided the contraceptives considerably decreased and even interruptedtheir assistance in favour of other areas which they consider a priority such as malaria,tuberculosis and AIDS."109
However, both governmental officials and donors told Amnesty International that inthe past few years, family planning has again become a priority, with the state wil ingto become financial y independent from donors for the purchase of contraceptives.
For example, the government spent 359 mil ion CFA francs in 2006, 410 mil ion CFAfrancs in 2007 and 450 mil ion CFA francs in 2008 (around US$820,000, 940,000and 1 mil ion).110 However, the cost of contraceptive products is stil currently 70 percent financed by international partners (with UNFPA contributing 80 per cent of thetotal provided by donors) and 30 per cent by the national budget.111
CLANDESTINE AND UNSAFE ABORTIONS
The lack of information and gaps in access to contraceptive methods partial y explainthe high number of clandestine abortions in Burkina Faso. These abortions are carriedout outside public health centres, often in unhygienic conditions and by untrainedpractitioners.
Although exact statistics are impossible to determine, the number of clandestineabortions is high. UN statistics published in 2002 indicate "that five per cent of alwomen admitted to maternity wards in hospitals in Burkina Faso had seriouscomplications resulting from il egal y induced abortions. Of these, 70 per cent werebetween the ages of 16 and 24 and 80 per cent were students or unemployed."112
According to more recent official statistics for the year 2008, complications arisingfrom clandestine abortions represented 6.3 per cent of maternity cases treated at thedistrict level (1,214 out of 19,400 cases) and 11.6 per cent of the cases treated inregional and university hospitals (277 out of 2,381 cases).113 These figures only coverwomen who had access to treatment in health facilities for post-abortioncomplications.
The real figure of clandestine abortions leading to serious health problems is certainlymuch higher. Official statistics do not take into account the women who do not go tohealth facilities after an unsafe abortion. Moreover, women do not admit to clandestineabortions and it can be difficult to differentiate an induced abortion from aspontaneous miscarriage.
Augustine suffered serious complications after an unsafe abortion.
Augustine, aged 25, lived during her childhood in Abidjan, Côte d'Ivoire, and returnedto Burkina Faso with her family when she was 12. Living in the streets with no resources,she became pregnant and tried to obtain an abortion. Amnesty International met her inFebruary 2009 after she had three sessions with an "illegal abortionist", followed bythree dilations and curettages (D and Cs) at a hospital in Ouagadougou. Her life was inserious danger.
Augustine told Amnesty International: "I did not want to keep the baby. I went to see aman so that he would help me get rid of my pregnancy. He took an iron bar and tried toget rid of the baby. But it didn't work. I returned again and he started over again withthe iron bar on the inside. I returned a third time but after that it was too painful. I paidhim a total of 15,000 CFA francs (around US$34). I did not go back. I was losing a lotof blood. I had a lot of pain on my right side. Finally, I went to a hospital in Ouagadougou.
I was suctioned, but everything didn't come out. So I had to start over, and there was stilldebris inside after the second time. I also had two sonograms. Yesterday morning[February 2009], I again had a lot of pain on my right side. But I did not have any wayto get to the hospital, so I had to go get my brother so that he could take me there onhis motorcycle. The nurse told me to take ‘cytotec' (a product used to open the cervix ofthe uterus in order to permit the evacuation of debris)."
When Amnesty International met her, Augustine was still suffering from persistent painsin her lower abdomen.
ABORTION: THE LEGAL FRAMEWORK
The government modified its legislation on abortion in 1996 to reduce the number ofassociated maternal deaths.114
Under the 1996 amended Penal Code, abortion is classified as a crime, and a personwho carries out an abortion is liable to between one and five years' imprisonmentand a fine of 300,000 to 1,500,000 CFA francs (around US$685 to 3,430). However,abortion is al owed if the life of the pregnant women or of the unborn child is in dangerand in cases of rape and incest.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Article 387 of the Penal Code states: "Voluntary interruption of pregnancy is al owedat al times during pregnancy if two physicians attest that the continuance of thepregnancy endangers the health of the woman or that a strong possibility exists thatthe unborn child will be afflicted with a condition of exceptional seriousnessrecognized as incurable at the time of diagnosis. Moreover, in a case of rape or incestestablished by the State prosecutor, a woman is authorized to request a physician toperform an abortion during the first 10 weeks of pregnancy."
The provisions al owing women to terminate a pregnancy in these circumstances arecomplex and difficult to meet.
For therapeutic abortions, two doctors have to attest to the danger of continuing thepregnancy. This can be an insuperable obstacle for women living in rural areas, sinceCSPSs are not staffed by doctors, so women have to travel to a hospital, which canbe difficult and costly.
In cases of rape or incest, the requirement that the public prosecutor establishes thatthe crime has been committed appears to be a particularly intimidating and deterrentcondition in a context where women victims face serious risks of stigmatization.115
The government appears to have done very little to inform the general population ofthe legal provisions al owing abortion under certain circumstances and most of thewomen met by Amnesty International in rural areas were not aware of theseprovisions.
The Special Rapporteur on the right to health has emphasized that: "The right tohealth, including sexual and reproductive health, encompasses both freedoms, such asfreedom from discrimination, and entitlements. In the context of sexual and reproductivehealth, freedoms include a right to control one's health and body."116
The Special Rapporteur on the right to health has also stated that: "Women withunwanted pregnancies should be offered reliable information and compassionatecounselling, including information on where and when a pregnancy may beterminated legal y. Where abortions are legal, they must be safe: public health systemsshould train and equip health service providers and take other measures to ensurethat such abortions are not only safe but accessible. In al cases, women should haveaccess to quality services for the management of complications arising from abortion.
Punitive provisions against women who undergo abortions must be removed."117
During an Extraordinary Assembly in Nigeria in October 2009, Health Ministers ofthe Economic Community of West African States (ECOWAS) cal ed for the passage ofsafe abortion laws as part of efforts to reduce the high maternal mortality rate in thesub-region.118
AMNESTY INTERNATIONAL'S POSITION ON ABORTION
Amnesty International believes that where women's access to safe and legal abortionservices and information is restricted, their fundamental human rights may be atgrave risk. Amnesty International therefore cal s on states to prevent and end graveabuses of women's human rights in accordance with state obligations underinternational human rights standards and to:
� repeal al laws which permit the imprisonment or any other criminal sanction onwomen who seek or have an abortion, and all other laws which provide forimprisonment or other criminal penalties solely for those providing information aboutor carrying out abortions;
� provide access to medical services for complications arising from abortion to alwomen in need in any circumstance, regardless of the legal status of abortion;
� take al necessary measures to ensure that safe and legal abortion services areavailable, accessible, acceptable and of good quality for al women who require themin cases of pregnancy as a result of rape, sexual assault or incest and pregnancywhich poses a risk to the life or grave risk to the health of the woman.
Amnesty International does not take a position on any other aspects of abortion.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
6/HEALTH FACILITIES HARD TO
‘HEALTH FACILITIES, GOODS AND SERVICES MUST BE WITHIN
SAFE PHYSICAL REACH FOR ALL SECTIONS OF THE POPULATION'UN Committee on Economic, Social and Cultural Rights, General Comment 14, para 12(b)
Health care facilities are often far from people's homes, especial y in rural areas, andtransport is unreliable and expensive. Although the government has increased thenumber of CSPSs in recent years, enormous disparities continue to exist betweenurban and rural areas. In the Central Region, which includes the capitalOuagadougou, 98 per cent of the population live less than 10km from a health centre,while in the Sahel Region only 50 per cent live within 10km.119
An official map of health facilities for 2007 showed that the districts containing thethree largest cities (Ouagadougou, Bobo-Dioulasso and Ouahigouya) had far shorteraverage distances than remote areas in the east and the north.120 Moreover, by 2008,11 districts across Burkina Faso stil had no district or regional hospital.121 Two regionsaround the capital (Central South and Central Plateau) have no regional or universityhospital, but depend on the university hospital in Ouagadougou.
The combination of the inequitable distribution of health facilities, especially theCSPSs, the poor road conditions and the absence of a transport network means thatmany women face significant barriers if they seek access to health services and facilities.
DIFFICULT JOURNEYS
Amnesty International investigated a number of cases where pregnant women haddifficulties in reaching health facilities in time because of long distances, weatherconditions (notably during the rainy season122), geographical obstacles such as rivers,and the lack of reliable and affordable transport. The government's stated policy is torefocus the role of traditional birth attendants towards identifying the place of deliveryand ensuring reliable transport to take the woman to the health centre for the birthor in case of complications. However, so far no transport system has been put intoplace, and women's families have to organize their own transport reach the health
HEALTH FACILITIES HARD TO REACH
A woman and her seven-month-old son, pictured by thetree where she gave birth. Women in rural areas oftencannot reach a health facility in time.
facility. There is no ambulance system to help transport women to a CSPS, even inan emergency. The ambulance system, where it exists, only operates between theCSPS and other health facilities.
Few roads are paved beyond the cities and major arteries, and they are not wellmaintained. In rural areas, women rarely have access to any means of transport andhave to rely on husbands and relatives, or on the generosity and solidarity of vil agers.
In general, women usual y walk or are transported by bicycles, motorcycles or donkeycarts to the health centres. This can be dangerously slow, especial y during the rainyseason when roads are muddy.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Maternity ward, Ouahigouyaregional hospital, Burkina Faso.
Ramatoulaye had to give birth on her own on the bank of a river.
Ramatoulaye, a 25-year-old housewife, lives in a rural village in the district of Séguénéga.
She had her first child at the age of 12, giving birth at home assisted by a traditional birthattendant. She told Amnesty International that during her later pregnancies, she hadbeen encouraged to go to the CSPS in Ramsa, 12km from her village, for prenatal visitsand to give birth. To reach Ramsa she had to take a boat to cross a deep river.
She told Amnesty International that during her fourth pregnancy, in March 2009, "Istarted to have my first pains. My husband's brother drove me with his motorcycle, myhusband followed us on another motorcycle. Once arrived on the bank of the river, welooked for the boatman but he was not there because he also has another job. But withouthim, no other person can help you to cross the river because it's deep and it is impossibleto cross it by foot. Thus I gave birth alone on the banks of the river. It was very difficult.
After my delivery, the boatman came back and I was able to get on the boat to go fortreatment in the CSPS in Ramsa."
HEALTH FACILITIES HARD TO REACH
Safiatou died while trying to reach a health centre after delivering at home.
Safiatou, 26, married her cousin Hamidou when she was 14 years old. They lived in avillage about 100km south of Ouagadougou, where they farmed livestock. She alreadyhad four children when she became pregnant again in 2007.
According to the nurse who saw her some days before her delivery, in May 2008, Safiatouhad not attended prenatal visits. She only went to the CSPS (some 12km from her home)at the end of her pregnancy and she stayed there for 48 hours because she was very weakand was suffering from anaemia. The nurse said that he impressed upon her and herhusband the importance of taking iron (provided free of charge) and that Safiatou shoulddeliver her baby in the health centre.
Safiatou's husband told Amnesty International: "The day of her delivery, she was in goodhealth and worked all afternoon as usual without any problem. She prepared tô [a localdish made from maize flour] for her children and went to get the hay for the animals. Inthe evening, when her labour began, she left for her mother's home. Her mother cameto warn me that she was not well, that we had to take her to the clinic. I do not have amotorcycle, so I had to go and get one. That made us lose time." The husband addedthat he "did not know that she should have delivered at the clinic. When I came to fetchher at her mother's house, she had lost consciousness."
The husband borrowed a small motorcycle from his neighbour, but it did not have anyfuel and the closest gas station was 10km away. They had to first push the motorcyclefor 10 km… Safiatou ended up delivering at home, but there was placenta retention andserious haemorrhaging.
Her husband asked a friend to help him take Safiatou to the CSPS but she died on themotorcycle 4km away from the health centre. The friend told Amnesty International:"When I arrived, Safiatou was delirious; she could no longer stand on her feet. Herhusband was afraid of driving her on my motorcycle. So we put her on the motorcyclebetween us. It was 2am when we left. There are three small ravines before you reach theCSPS. Each time, we had to get off the motorcycle and then get back on, and withSafiatou, it was not easy… At some point, Safiatou wasn't moving anymore, weunderstood that she had died. We did not go to the CSPS. We decided to take an easierroad, to return to the village with the body."
Safiatou left five boys, aged 11, nine, seven and four, and the newborn baby. Since herdeath, the children spend their days with their maternal grandparents and sleep at theirpaternal family's home. Safiatou's father was devastated by the death of his daughter.
The Amnesty International delegates were told that since then he "no longer gets up, hedoes not sleep and he almost doesn't eat any more."
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
The geographical and other barriers encountered by pregnant women explain thelow number of assisted deliveries in rural areas. For example, in the area covered bya rural CSPS in the district of Tougan, official figures indicate that in 2007 the averagerate of assisted deliveries was 11.22 per cent for communities within 5km of thehealth centre but only 4.05 per cent for communities more than 10km away.123
Faced with these difficulties, many women resort to the services of traditional birthattendants even though officially they are no longer supposed to deliver babies.
A traditional birth attendant in a village some 30km west of Ouagadougou toldAmnesty International:
nobody, I have to do it. Last Tuesday [8 July 2008], a woman had pains, itwas bucketing down and because of the big rains, roads were impracticable
and as the family had only a cycle it was impossible to bring her to the healthcentre. I was called at midnight by the husband. I went with my scarf but I had notools. The woman was shouting. I asked to switch on a light, they brought me akerosene lamp, I examined her, her water had just broken and the amniotic liquidhad gone out. I asked them to put her on a tablecloth. I delivered her with myhands, without gloves. It went well, it was a girl."
Under the CEDAW, Burkina Faso is under an obligation to ensure access for ruralwomen to adequate health care facilities, including information, counselling andservices in family planning.124 Both the CESCR and the CEDAW Committee haveclarified that the realization of women's right to health requires the removal of albarriers interfering with access to health services.125 The CEDAW Committee hasstated that "barriers include… distance from health facilities and absence ofconvenient and affordable public transport."126
The CESCR has also emphasized that states are under a core obligation to ensure theequitable distribution of al health facilities, goods and services and also the right ofaccess to health facilities, goods and services on a non-discriminatory basis, especial yfor vulnerable or marginalized groups.127 The government is therefore under a dutyto prioritize those groups, who face the greatest barriers realizing their rights, whenal ocating resources.
HEALTH FACILITIES HARD TO REACH
Pregnant women also have to overcome another obstacle. Women in labour aregeneral y accompanied by members of the family or by friends. Being alone duringchildbirth is seen as socially unacceptable, and a woman's companions have anumber of tasks to perform, such as washing clothes and feeding her.128 However, ifthe pregnant women arrives "too early" at the health facility, she may be asked toreturn later, which may annoy her companions and make them reluctant toaccompany her again.
A housewife who sel s mil (a smal -seeded cereal) in a rural vil age told AmnestyInternational:
the morning when I started to feel pain. Friends working in the market agreedto accompany me in a cart to the CSPS, 7km from there. It took more than
two hours to reach the CSPS. But the [auxiliary] midwife said to me that it wasmuch too early. On returning to the village, my friends made me understand thatthey had wasted time to accompany me pointlessly. I continued to have pain but Idid not dare to ask them any more to come along. Finally, one evening, the painwas unbearable and I had to deliver at home with a traditional birth attendant."
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
7/COSTS AS A BARRIER TO
‘HEALTH FACILITIES, GOODS AND SERVICES MUST BE AFFORDABLE
FOR ALL'Committee on Economic, Social and Cultural Rights, General Comment 14, para 12(b)
"It cost too much for a poor man like me"
Albertine, a 25-year-old mother of two children, died in January 2007 at a regionalhospital 200km north of Ouagadougou.
Albertine's brother-in-law, who farms during the rainy seasons and also works in themines, told Amnesty International in July 2008: "Her husband was not in the village whenher labour pains started and I took her by motorcycle to the CSPS, 15km from our village.
I paid at least 5,000 CFA francs (around US$11.50) for medicines but the medicalpersonnel told me that they could not do anything, that she needed to be hospitalizedat the regional hospital. As I had given them all the money I had, I brought back Albertineto our village. But the next day, she was still having labour pains and after borrowing somemoney I took her to the hospital."
"I was told that Albertine needed a blood transfusion and I was given a prescriptioncosting around 20,000 CFA francs (around US$46). I don't know whether this moneywas to buy blood or medicines. After the transfusion, Albertine seemed to be doing better.
The next day she gave birth to a stillborn baby."
"On the third day, she was suddenly very cold. She was given a prescription and I paid15,000 CFA francs (around US$34) to buy her injections and medicine. On the fourthday, she had a relapse; I was given a new prescription for new medicines costing 12,000CFA francs (around US$27.50) but I didn't have any more money. So I had to go to thevillage and back. On the fifth day, I came back with the money and paid for the medicinesbut Albertine had died in the meantime. I did what I could to save my sister-in-law butit cost too much for a poor man like me."
COSTS AS A BARRIER TO HEALTH CARE
An 18-year-old woman in labour in a new clinic inGorgare. This is her first child and she is accompaniedby her aunts who wait outside. Health centre (CSPS) inGorgare, Burkina Faso.
In many parts of world – especial y, but not solely, in developing countries – cost hasbeen identified as a significant barrier to people's access to health care. The case ofAlbertine clearly shows how costs can deter or delay medical treatment, endangeringthe life of a pregnant woman.
People have paid directly for medical care in Burkina Faso since the 1980s. TheBamako Initiative,129 a policy adopted by African health ministers designed to raiserevenue for health care and increase efficiency in the use of health services by, amongother things, imposing and decentralizing control of user fees, stimulated thegovernment to put in place a uniform pricing system throughout the country in 1993.
At the same time, however, conscious of the fact that this system of direct paymentscreates an impassable barrier to people living in poverty, the government adoptedseveral policies to al ow waivers or subsidies in some cases.130 Prenatal visits weremade free for al women in 2003.131 The government also announced a policy towaive al payments from those unable to pay (so-cal ed "indigents") in accordancewith one of the principles of the Bamako Initiative aimed at "ensuring that the pooresthave access to primary health care".
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
THE 2006 SUBSIDY POLICY
The decision made in 2006 to subsidize emergency obstetric and neonatal care(EmONC) was taken in a context of general wil ingness to reduce financial barriers tohealth care. This policy was prepared with the support of the World Bank, whichplayed a key role.132 The subsidy policy is funded by the national budget with aplanned budget close to 30 bil ion CFA francs (around US$68.5 mil ion) for the periodfrom 2006 to 2015, of which 5 bil ion CFA francs (around US$11.5 mil ion) was tobe devoted to giving free care to pregnant women deemed indigent.133 The policybegan to be implemented in October 2006 for caesarean sections and in January2007 for other deliveries.
The main components of the subsidy policy
� 80 per cent of the cost of deliveries and caesarean sections is covered by
government subsidy, with women paying the remaining 20 per cent. The subsidizedpayments from patients are meant to cover parts of the costs of medical services,drugs and supplies needed for the delivery. Complications and postnatal careduring the first week after the delivery are also covered by this policy.
� Transport between a CSPS and a referral hospital is free for all pregnant women.
� The subsidy covers the entire health costs for indigent pregnant women.
Under this policy, deliveries are subsidized by 80 per cent.134 Patients have to pay 900CFA francs (around US$2) for normal deliveries, 3,600 CFA francs (around US$8) forcomplex deliveries and up to 11,000 CFA francs (around US$25) for caesareansections or for treatment of a complication during the delivery. This sum covers thecost of medical services and a kit containing the drugs and supplies (such as sterilegloves and syringes) needed for a normal delivery or for a caesarean section.135
The subsidy policy only comes into effect when the pregnant woman arrives at thehealth care centre. Transport costs between home and the care centre can be a realbarrier for women in poverty, but are not taken into consideration in this policy.
However wel elaborated on paper, this policy subsidy suffers from several severeshortcomings. In every case studied by Amnesty International since the policy wasimplemented, the families said that they had paid more than the amount outlined inthe policy. Many families said that they had to pay for gloves because the medical staffdid not have any more, as wel as other products or medicines. Moreover, almost alhad to buy bleach to clean the delivery room.
COSTS AS A BARRIER TO HEALTH CARE
Some midwives and doctors continue to prescribe branded medicines, rather thangeneric drugs as required by national policy. An expert told Amnesty International:
the deliveries relies upon the use of generics. However, some doctors continueto prescribe patented drugs that are available in a generic form which means
that the families have to go to private pharmacies outside the health facilities andspend much more."
Women's families are therefore forced either to pay for branded medicines or toforgo potential y life-saving treatment, although equivalent generic medicines areusual y available free of cost.
The main problems undermining the implementation of the subsidy policy are:
� absence of clear communications to women and health staff about the policyand, notably, lack of clarity on what is subsidized and what is exempted;
� in some districts, failure to implement an effective free referral service betweenhealth facilities due to factors such as shortages of ambulances and fuel;
� absence of criteria enabling indigent women to be identified.
In practice, the subsidy policy is also undermined by the fact that health care staffoften demand unofficial payments for treatment, supplies or transport.
LACK OF INFORMATION ON THE SUBSIDY POLICY
Many people136 told Amnesty International that they were not entirely sure whichtreatments or medical products were free, which were subsidized and which had tobe paid for in ful .
This has given rise to confusion and suspicion. A midwife told Amnesty International:
"Since the launch of the subsidy policy, there is stil an endless conflict between themedical staff and the patients because the masses think that everything is now freewhilst several treatments, including blood tests and scans, must stil be paid for."
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
"I don't know why I paid so much money, I was told health care is now free."
In March 2009, Amnesty International investigated the case of a woman who had nearlydied two days earlier in a district hospital near Bobo-Dioulasso.
The doctor who treated this woman told Amnesty International: "This woman sufferedfrom high blood pressure, pre-eclampsia, anaemia and malaria. When she arrived at thedistrict hospital, she was feeling dizzy. During her delivery, she was suffering from ahaemorrhage due to a cervical rupture. We can consider her to be a near-miss."137
Her husband, who sells textiles, told Amnesty International: "I paid a total of 22,500 CFAfrancs (around US$51.50). My wife followed the three prenatal visits and each time I wasasked to pay. I had to pay successively 2,000, 1,000 and 1,000 CFA francs (aroundUS$4.50 and US$2.25) for medicines but I didn't receive any receipt and I don't knowwhether I should have paid for them."
"I was then given two prescriptions for medicines I bought at the pharmacy, which costme 3,875 CFA francs and 1,750 CFA francs (around US$9 and US$4). When we reachedthe hospital, I was told I had to buy gloves and serum for which I paid 650 CFA francs(around US$1.50). I was then asked to pay for bleach in order to clean the deliveryroom. I then bought a kit for the delivery that cost 3,600 CFA francs (around US$8) andthen after the delivery I was given another prescription and I had to pay 2,250 CFA francs(around US$5). I've still got to pay the hospital bills which are likely to be expensivebecause my wife has been hospitalized for a whole week. I don't know why I paid somuch money, I was told health care is now free."
According to the subsidy policy, this man should only have had to pay 3,600 CFA francs(around US$8) for the delivery. The prenatal visits and some of the medicines givenduring those visits should have been free. The remaining costs linked directly to thedelivery, including gloves, medicines and hospitalization costs during the first week afterthe delivery, are normally covered under the subsidy policy. Amnesty International wasnot able to find out whether these payments stemmed from real stock shortages or not.
The widespread confusion over what the subsidy policy covers al ows extortion ofmoney by medical staff.
A recent study found that "only 2 per cent of the budget allocated for theimplementation plan was devoted to the communication of the policy to the generalpublic."138 That money was largely spent on radio programmes and local meetings.
Two years after the beginning of the policy, notices were put up in French in manyhealth facilities showing what is subsidized and the prices to be paid by patients.
However, the notices do not include several treatments which patients stil have to payfor, and in any event a large proportion of the population cannot read.
COSTS AS A BARRIER TO HEALTH CARE
NO FREE TRANSPORT BETWEEN HEALTH FACILITIES
One important aspect of the subsidy strategy is that transport between the primaryhealth care centre and the referral hospital is provided free of charge. However,Amnesty International has col ected information on a number of cases where familieshad to pay for this transfer. In some cases, ambulance drivers or medical personnelappear to have taken advantage of the urgency of the situation to demand money. Inothers, the family had to pay for fuel for the ambulance.
These costs, added to the price of drugs, can lead to delays in transferring women tohospital for emergency care.
Awa, aged 26, died in September 2007.
Awa, who married when she was 17, became pregnant for the fifth time and gave birthat a CSPS in September 2007. She then had severe pains in her stomach. Another wifeof Awa's husband told Amnesty International: "She was seen by a midwife's assistant,who prescribed her medicines, for which we paid the sum of 11,250 CFA francs (aroundUS$26). I don't know what medicines we had to buy."
A nurse told Amnesty International that "after delivering a stillborn baby, she wasswimming in her own blood. An uterine revision was done and she was kept underobservation. Her husband opposed this observation because he said that he didn't haveenough money to buy any medicines." She was taken home in the afternoon at around4pm.
Early the next morning, her family brought her back to the CSPS. She was given aprescription but the medicines were not available at the health centre store and thefamily had to pay 5,750 CFA francs (around US$13) to get them.
That afternoon, at around 2pm, the nurse said that they could not do anything more forAwa and that she had to be evacuated by ambulance to the university hospital inOuagadougou. As there was apparently no fuel for the ambulance, Awa's husband wasasked to pay for it. He said he could not afford this, and the nurse had to negotiate withhim for quite a long time until he agreed to pay 5,000 CFA francs (around US$11.50)for the fuel. They left the CSPS at around 4.30pm and arrived at the hospital inOuagadougou an hour later.
At the hospital, there were no free beds, so she had to lie down on a mat on the floor.
One became free at 7.30pm, but Awa died a few minutes later.
The hospital medical records note puerperal infection (an infection that occurs afterchildbirth), serious malaria and eclampsia.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
NO CRITERIA TO IDENTIFY WOMEN ENTITLED TO FREE CARE
According to the subsidy policy, about 17 per cent of the available funds – close to5 bil ion CFA francs (around US$11.5 mil ion between 2006 and 2015) – would beused to provide free care to indigent women. However, this part of the policy has yetto be implemented, largely because the government has established no criteria toidentify who qualifies as indigent.139
In interviews with Amnesty International, the authorities asserted that it was verydifficult to determine criteria of poverty and that it was necessary at al costs to avoidabuse of the system. Their fear was that some people would falsely claim to beindigent in order to take advantage of the system.
However, an experiment led by researchers with health workers and communityrepresentatives in the Ouargaye district demonstrates that identifying people whoshould qualify under such schemes is possible. In 124 vil ages, selection committeeswere put in place and they were able, without pre-established criteria, to select peoplethat the vil agers considered should benefit from free health care.140
The lack of political will in implementing this key aspect of the subsidy policy iscorroborated by the fact that very little, if any, information on this part of the subsidypolicy has been disseminated by the authorities. According to a study carried out in2008, "Although the state provided that there would be 5 billion CFA francs forindigent people until 2015 under the subsidy policy, the majority of people met in thefield as wel as some of those at a central level were absolutely not aware of thispossibility."141
In a country where according to official figures nearly half of the population lives belowthe national poverty line,142 the fact that the government has done nothing to identifyand address the emergency obstetric needs of the most marginalized women, whowould otherwise be unable to afford essential health care, undermines the entiresubsidy policy. It also contravenes Burkina Faso's obligation under internationalhuman rights law to ensure the affordability of health care and, when allocatingresources, to prioritize the most vulnerable and marginalized groups who face thegreatest barriers realizing their rights.
COSTS AS A BARRIER TO HEALTH CARE
UNOFFICIAL PAYMENTS
In the course of its research, Amnesty International col ected many testimonies fromthe families and friends of pregnant women who paid unofficial and il egal sums tomedical personnel while seeking medical care.
"If you are poor, you are ‘left'; if you can pay, you are treated."
Mariam was 23 when she died in a hospital in Ouagadougou in April 2008, 13 daysafter delivering a stillborn baby. Mariam lived with her husband, Ali, a motorcyclemechanic, in Ouagadougou. Their first child died at six or seven months. During Mariam'ssecond prenatal visit at a nearby CSPS, they learned that Mariam was expecting twins.
A few days later, they were told that Mariam needed blood tests which cost 3,200 CFAfrancs (around US$7). Ali told Amnesty International: "Actually, the personnel told usthat the ones who did the exams were not there and I understood that we had to pay. Ireally wanted the exams to be done. As soon as I paid, my wife was able to do the tests."
There were problems during the delivery. One baby was born (he survived), but the seconddidn't come out. Mariam was then transferred to a hospital where she spent three days.
One week later, Mariam became dizzy and experienced severe headaches. Ali took herback to the hospital. He told Amnesty International: "Mariam was moaning and shakinga lot and several medical personnel told me I had to pay for products, I don't know whichones. I paid several sums amounting to more than 30,000 CFA francs (aroundUS$68.50)."
The following day, Mariam was told that she could go home. Her husband said: "Wewere getting ready to leave, but Mariam said that she wanted to sleep: she slept from 7amto 7pm at the hospital. But once Mariam was awake, she was not well. She began toshake again and had to be taken back to the emergency ward." Her husband was againgiven a prescription and had to pay 4,500 CFA francs (around US$10) for a box of gloves.
"They opened them and gave me some. I was not given the other gloves. After waitingfor two hours, I went to ask why the treatments had still not begun. I was told that therewere sicker patients to treat first. I kept waiting and then asked why they were not takingcare of my wife. I was told: ‘You must first take care of your patient'. I then realized thatI had to pay so that they would take care of my wife: I handed over 5,000 CFA francs(around US$11.50) and then my wife was taken care of."
Ali was given another prescription but he could not find the product. "I asked a nursefor help. She offered to sell me the product that she herself had bought for her mother.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
She told me that the product cost 7,000 CFA francs (around US$16) from a pharmacyand that she would sell me it for 4,720 CFA francs (around US$11). I gave her 10,000CFA francs (around US$23) and she gave me back my change but it was too late, my wifedid not use this product, as she had already died."
In total, the delivery and the trips to the hospital cost Ali around 90,000 CFA francs(around US$206).
Mariam's eldest brother said, "my sister died due to a lack of means and adequatetreatment. The hospital, it is like a chamber of commerce. If you are poor, you are ‘left';if you can pay, you are treated."
It is clearly forbidden for medical staff to sel medicines, which can only be boughtfrom pharmacies, where receipts should be given, but often are not.
The information col ected by Amnesty International shows that two types of corruptionare widespread: people are asked to pay to have access to a medical facility ortreatment; and people are charged for medical supplies which should be coveredunder the subsidy policy and which have been misappropriated.
These corrupt unofficial payments take several forms, notably:
� ambulance drivers demanding large sums to transport a woman from a healthcentre to a hospital although this transfer is official y free under the subsidy policy;143
� staff sel ing medicines and supplies that should be covered under the subsidypolicy, citing shortages;
� doctors prescribing branded medicines instead of generic drugs;
� staff demanding money so that a patient wil be treated more quickly or diligently,or wil be given a hospital bed.
Each of these forms of payment was described to Amnesty International by severaldifferent witnesses. For example, the husband of a woman who died in August 2007of a haemorrhage in a city 200km north of Ouagadougou told Amnesty International:
hospital. At that time, our area was not covered by the cell phone network, soI went by bicycle to fetch an ambulance from the regional hospital. The
ambulance driver demanded that I pay him 12,000 CFA francs (around US$27.50)
COSTS AS A BARRIER TO HEALTH CARE
A woman sits with her daughter and newborn sonoutside the maternity ward in Kiembara, Burkina Faso.
before he would start the vehicle. I didn't have the money and had to ask a friendwhich delayed our departure."
Anxiety and uncertainty when complications arise during childbirth make familiesvulnerable to extortion. In addition, as a researcher who investigated the issue ofcorruption in Burkina Faso has stressed, "the asymmetry of information that putssick, illiterate patients face-to-face with more knowledgeable doctors leads to aninformational imbalance that encourages … corruption."144
Local NGOs and journalists have consistently monitored and exposed cases ofextortion by medical personnel. According to REN-LAC, the National Network to FightAgainst Corruption (Réseau National de Lutte Anti-Corruption), the health sector hasbeen for many years seen by the population as one of the sectors most tainted bycorruption. In its most recent annual report, published in December 2007, REN-LACfound that the health sector was perceived by the people it surveyed to be the fourthmost corrupt sector, after customs, taxes and the justice system.145
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
THE DEBATE AROUND TOTAL FEES EXEMPTION
The issue of providing obstetric care free of charge has been debated in BurkinaFaso for several years. Some experts, policy-makers and NGOs have argued for atotal fees exemption to ensure greater clarity throughout the system, to al ow the mostmarginalized people living in poverty, especial y women, to have access to healthcare and also to make it more difficult for health staff to demand unofficial payments.
Similar debates are also taking place in other countries in Africa and elsewhere.146
When elaborating the subsidy policy, in June 2006, the government examined threeoptions: a subsidy of 60 per cent, 80 per cent or 100 per cent of the cost. Thegovernment apparently excluded the full fees exemption option not so much onfinancial grounds, but because of the fear that providing a free service would tend tomake the population irresponsible in its use of services. An official documentpublished in June 2007 stated that: "several scenarios were envisioned includingone that configured free services. Nevertheless, the idea of subsidy was chosenbecause according to some findings, free services create less accountability from therecipient."147
Several government officials repeated to Amnesty International the view that freehealth care can be counter-productive because it does not give the public a sense ofthe value of the services provided.148
PILOT PROJECTS PROVIDING FREE CARE
The total fees exemption option is currently being studied in two pilot projects inBurkina Faso, led respectively by the Swiss NGO Terre des Hommes (TDH) and bythe German NGO HELP.
The TDH project covers two northern districts. Launched in October 2008, it providesfree care for pregnant women, breastfeeding women and children under the age offive. The project, initiated at the request of the European Union, is financed by theEuropean Commission Humanitarian Office (ECHO).
The project provides technical support to all 47 CSPSs and two hospitals in thedistricts of Tougan (Sahel region) and Séguénéga (Northern region). This supportcosts close to 25,000 euros per month.
Since the launch of this project, TDH has noted a sizeable growth in the numberof people visiting the CSPSs. According to TDH, the increase in Tougan has been235 per cent, with an 18.6 per cent increase in the number of deliveries in hospital.
The population's confidence in the health system has similarly risen.
COSTS AS A BARRIER TO HEALTH CARE
A representative from TDH told Amnesty International at Ouagadougou in March2009:
order to demonstrate that total exemption of payment for care for youngchildren and their mothers is possible, in the hope that this experiment will
be undertaken again on a larger scale."
TDH sought to increase community mobilization in order to encourage visits to healthcentres. They have made nurses available to the public, and have assigned apharmacist to Tougan to manage prescriptions and the reimbursement system linkedto the exemption of costs.
TDH have also attempted to resolve transportation problems. One solution (a "healthcare taxi" pulled by a donkey) has not been successful while another (maternitywaiting houses near CSPSs) has worked wel .
TDH staff believe that the project has been a success but fear for its future, as a TDHrepresentative explained:
and emergency) doctor, it is for the time being financed for 2009 and we hopethat this will be continued through 2010 but it is not designed to be followed
indefinitely. It is therefore necessary to take lessons from this experiment and seehow to perpetuate or even extend it. Otherwise, the enormous expectations that wehave created at the heart of the population run the risk of being cruellydisappointed."
The HELP project is running in two districts in Sahel region. After having successful yled a project providing free care for children under the age of five and pregnant andbreastfeeding women in Niger, HELP proposed to the Burkina Faso government asimilar project in one of the regions where health services are less wel used, theSahel region.149 This project was launched in September 2007 in the Dori and Sebbadistricts, with a total of 450,000 inhabitants.
A large information campaign was organized in the vil ages in order to explain theproject. Taking into consideration the lessons learned in Niger, the local healthmanagement committees (COGES) were involved from an early stage. The systemfor reimbursement after consultations provided without charge to patients wentthrough the committees as an integral part of the process. After 10 months ofexperience, it was established that each consultation for a child cost about 1,200
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
CFA francs (around US$2.50). For deliveries, HELP met the cost of 900 CFA francs(around US$2) established under the national subsidy policy.
According to an expert who studied the impact of this project:
system has recovered and mothers are bringing their ill children a lot earlierthan before the launch of this project."
The use of health services for children under the age of five more than doubled, whiledeliveries assisted by qualified staff increased by 50 per cent when comparing the 10months before the project started with the fol owing 10 months.
HELP, in col aboration with TDH and other NGOs, has organized a series of activitiesaimed at documenting the effects of the fees exemption in order to promote a decisionto exempt fees throughout the whole country.
Both TDH and HELP have reported that the projects appear to be reducing theincidence of preventable maternal mortality. While Amnesty International has notverified these results, these models should be investigated and discussed further bythe authorities, while reviewing the health policy.
REMOVING FINANCIAL BARRIERS TO MATERNAL HEALTH CARE
The government of Burkina Faso has made real efforts to reduce significantly thecost of maternal health care, but the remaining 20 per cent that has to be paid by thepopulation stil poses a barrier for many women needing essential and life-savingtreatment. First of all, many women still have to rely on their husbands or othermembers of their family to pay the subsidized price for heath care. Secondly, thispolicy is not wel understood by the public, leading to confusion and to unofficialpayments demanded by medical staff. Thirdly, the most marginalized indigent womendo not in practice receive free care as there are no criteria for identifying the womenentitled to a total exemption from costs.
A total subsidy for sexual and reproductive health care would therefore greatlycontribute to the government's stated goal of ensuring that al pregnant women haveaccess to medical y assisted deliveries. As il ustrated by the TDH and HELP projectsin Burkina Faso, and other projects in Africa, removing costs increases the demandfor health services. It also makes the health policy clearer for the population andmakes it more difficult for medical personnel to demand unofficial payments.
COSTS AS A BARRIER TO HEALTH CARE
While in the recent past user fees for health care have been promoted as a means ofcost recovery and improving efficiency in service provision, the reality has shown thatthey are often a significant barrier to access to health services. They often haveparticularly negative effects on people living in poverty, especial y the poorest andmost vulnerable, and a have particularly detrimental effect on women living inpoverty.150
The WHO has also highlighted the negative effects of payments for health care, statingin its World Health Report 2005 that: "Catastrophic payments for health care – whichpush about 100 mil ion people in the world into poverty every year – occur whereverhealth services require out-of-pocket payments, there are no mechanisms for financialrisk-pooling, and households have a limited capacity to pay."151
Even when there are exemptions and waivers to protect those who cannot afford topay, these have often been found to be unreliable, ineffective, costly and difficult toadminister and also open to misuse – with people often not aware that exemptionseven exist and that they are entitled to them if they cannot afford to pay for necessaryhealth care.152
While fees are stil in place in many countries, in recent years a lot of attention hasbeen paid by NGOs, UN agencies and governments to the negative effects of chargingfees for essential health services on people living in poverty and the need to providefree health care services where necessary to ensure access.
A report published in June 2009, called The Global Campaign for the HealthMil ennium Development Goals 2009 – Leading by Example – Protecting the mostvulnerable during the economic crisis, which was endorsed by a number of countries,UN agencies and institutions, stated that: "Evidence is now mounting for the efficacyof a package of free quality services at the point of care to overcome the inequity thatfee-for service inevitably breeds. This is one effective, evidence-based and equitableway to expand access to services to a greater proportion of the population."153
Thus there is now an emerging policy consensus that removing fees that present afinancial barrier to health services is a key element in achieving universal access toessential health care, with a number of developing countries removing fees and anumber of donors committing to support countries to do so with technical and financialassistance. September 2009 saw a donor agreement to support six countries to increaseaccess to free health care: Burundi, Ghana, Liberia, Malawi, Nepal and Sierra Leone.154There is also a growing consensus on the vital need to strengthen countries' healthcare systems in order to prevent avoidable deaths and il ness. The removal of userfees therefore needs to be accompanied by additional measures to increase theavailability of quality services, which requires an increase in the number of adequatelytrained and remunerated health professionals and adequate medical facilities and
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
supplies, in order to respond effectively to increased demand and ensure quality ofcare.155
In Burkina Faso, while the provision of free obstetric care presents evidentadvantages, many believe that such a policy can only succeed if the management offunds and medical supplies is greatly improved. As a doctor from Burkina Faso toldAmnesty International in March 2009:
can be the solution, but the problem is knowing how to secure the presenceof medical material in the public sector, in other words, how to prevent this
material from disappearing and then being sold privately."
A policy for the total exemption of costs for obstetric services, if adopted, shouldtherefore be accompanied by other measures to ensure that it can be implementedeffectively and increase access to quality care. To this end, any policy on removingfinancial barriers to health care needs to be communicated in a timely and effectiveway to both health facilities and service users, and must be implemented in tandemwith the necessary measures to strengthen and improve health care centres, such asincreasing the number and ensuring the equitable distribution of adequately trainedhealth care staff, improving staff's working conditions, ensuring the provision ofnecessary medical supplies and equipment, having an effective referral system andenhancing monitoring and accountability systems in the health care system.
THE RIGHT TO HEALTH AND FINANCIAL BARRIERS
One of the crucial components of the right to health is economic accessibility oraffordability. The CESCR has emphasized that under Article 12 of the InternationalCovenant on Economic, Social and Cultural Rights: "health facilities, goods andservices must be affordable for all. Payment for health care services, as well asservices related to the underlying determinants of health, has to be based on theprinciple of equity, ensuring that these services whether privately or publicly provided,are affordable for al , including social y disadvantaged groups. Equity demands thatpoorer households should not be disproportionately burdened with health expensesas compared to richer households."156
The government is also under a duty to prioritize the most vulnerable andmarginalized groups, who face the greatest barriers realizing their rights, whenal ocating resources.
COSTS AS A BARRIER TO HEALTH CARE
Burkina Faso, as a state party to CEDAW, is under an obligation to take al appropriatemeasures "to eliminate discrimination against women in the field of health care inorder to ensure, on a basis of equality of men and women, access to health careservices" and "to ensure to women appropriate services in connection withpregnancy, confinement and the post-natal period, granting free services wherenecessary, as wel as adequate nutrition during pregnancy and lactation" (Article 12).
The CEDAW Committee has interpreted Article 12 of CEDAW to include a requirementon states to eliminate barriers to access to health services such as high fees and totake measures to ensure women timely and affordable access to health services.157The Committee has emphasized that it is the duty of states to ensure women's rightto safe motherhood and emergency obstetric services and that they should al ocateto these services the maximum extent of available resources.158
The Special Rapporteur on the right to health has also stated that the right to healthentitles women to reproductive health care services, goods and facilities that areaccessible physical y and economical y: "Physical access to, and the cost of, healthservices often influence women's decisions about whether or not to seek care. Inmany countries, reducing maternal mortality wil depend on making relevant servicesmore accessible, including through expansion of relevant services into underservedareas. It wil also often depend on ensuring relevant interventions are affordable."159
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
8/SHORTAGES OF STAFF AND
‘FUNCTIONING PUBLIC HEALTH AND HEALTH CARE FACILITIES,
GOODS AND SERVICES, AS WELL AS PROGRAMMES, HAVE
TO BE AVAILABLE IN SUFFICIENT QUANTITY WITHIN THE STATE
PARTY. THEY WILL INCLUDE, HOWEVER, THE UNDERLYING
DETERMINANTS OF HEALTH, SUCH AS SAFE AND POTABLE
DRINKING WATER AND ADEQUATE SANITATION FACILITIES,
HOSPITALS, CLINICS AND OTHER HEALTH-RELATED BUILDINGS,
TRAINED MEDICAL AND PROFESSIONAL PERSONNEL RECEIVING
DOMESTICALLY COMPETITIVE SALARIES, AND ESSENTIAL DRUGS.
‘… AS WELL AS BEING CULTURALLY ACCEPTABLE, HEALTH
FACILITIES, GOODS AND SERVICES MUST ALSO BE SCIENTIFICALLY
AND MEDICALLY APPROPRIATE AND OF GOOD QUALITY. THIS
REQUIRES, INTER ALIA, SKILLED MEDICAL PERSONNEL,
SCIENTIFICALLY APPROVED AND UNEXPIRED DRUGS AND
HOSPITAL EQUIPMENT, SAFE AND POTABLE WATER, AND ADEQUATE
SANITATION.'UN Committee on Economic, Social and Cultural Rights, General Comment 14, para 12(a) and (d)
Despite significant efforts by the government to improve health facilities and increasethe skil s of medical personnel, the quality of emergency obstetric treatment remainslargely inadequate and many women do not have access to a skil ed attendant atbirth. Both factors contribute to the high number of maternal deaths in Burkina Faso.
The health care system suffers from several recurrent problems which have a seriousimpact on maternal mortality:
� inadequate health infrastructure
� shortages and interruptions of supplies of drugs and medical equipment
SHORTAGES OF STAFF AND SUPPLIES
A midwife checks a 17-year-old girl who is in the firststages of labour. This is her first child. Lankoué,Burkina Faso.
� recurring blood shortages
� lack of trained medical personnel
� lack of skil ed birth attendants
INADEQUATE HEALTH INFRASTRUCTURE
In the 2001 PNDS, the authorities acknowledged that "health facilities and medicalsupplies have been given until now very little attention in terms of maintenance" andthat they should "define a maintenance strategy for infrastructures and supplies."160During Amnesty International's four research missions in Burkina Faso, the delegatesvisited a number of health facilities, nearly all of which were suffering frominfrastructural problems.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
This 23-year-old woman was referred to a regionalhospital for a caesarean three days before thisphoto was taken. When she failed to recover fromthe operation she was sent to Yalgado hospital inOuagadougou, where she was diagnosed with anaemia,hypertension and kidney problems. She wasunconscious for most of her stay at Yalgado and wasdisoriented when awake. She died eight days after thisphoto was taken on 1 July 2009.
DILAPIDATION AND INSANITARY CONDITIONS IN HEALTH PREMISES
Most of the health facilities visited by Amnesty International had significantinfrastructural problems. Some CSPSs visited were very run down, with brokenwindows and holes in their sheet metal roofs. They suffer flooding when it rains, dueto the age of the buildings or a lack of upkeep and maintenance.
Such problems can be found to different degrees at al levels of the health system,from the CSPS to the national university hospitals. During a visit to one of the universityhospitals in June 2009, Amnesty International observed that the access roads on thehospital's grounds are not asphalted, and the external corridors leading to thematernity ward are flooded when there is heavy rain.
SHORTAGES OF STAFF AND SUPPLIES
Health facilities are desperately short of space and Amnesty International saw womenin a university hospital who were about to give birth or had just given birth sleepingon the floor in the corridors.
ELECTRICITY SUPPLY
There are recurring and serious problems with the electricity supply for healthfacilities, especial y in rural areas where health centres rely on solar power. In severalrural health centres, medical personnel told Amnesty International that the solarpanels were damaged and had not been replaced.
An auxiliary midwife working in a rural CSPS said that the solar power batteries onlylast four hours a day, and that she regularly had to perform deliveries "with a torchheld between her neck and her shoulder".
Electricity supply is also a problem in several district hospitals in Ouagadougou.
During a research mission in March 2009, Amnesty International delegates learnedthat a few days earlier the medical personnel of a district hospital in Ouagadougou hadto help a woman give birth by candlelight because there was no electricity.161 Thishospital, which has particularly serious infrastructure problems, can barely carry outsurgical operations. During a meeting with Amnesty International a few days later,the Minister of Health, Seydou Bouda, acknowledged the problem and said that thisdistrict hospital "was undergoing considerable renovation".
WORKING CONDITIONS
Working conditions for staff in surgical units and delivery rooms are extremely difficultbecause of the lack of basic hygiene and adequate ventilation. Medical personnelcomplained to Amnesty International about the insanitary conditions, including filthyrooms and toilets that were blocked for weeks at a time.
Amnesty International delegates saw in June 2009 a flooded corridor leading to thesurgical unit in one of the university hospitals and they saw cockroaches crawling onthe wal s of the maternity ward's staff room.
In the country's biggest health facilities, which carry out a large number of caesareansections, the lack of air conditioning is a major problem. An obstetrician told AmnestyInternational: "Without air conditioning it is very difficult to operate at such hightemperatures since we cannot open the window because of germs."
During meetings with government officials and members of Parliament, AmnestyInternational raised its concerns regarding the state of the health facilities that it had
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
visited and echoed the frustrations of medical personnel. Al the government officialsin charge admitted that they were aware of the situation and a senior member ofParliament said that he had seen some CSPSs "in an unimaginable state ofdilapidation with holes in the roof", and explained this was due to budgetaryconstraints.
Infrastructure and supply issues in 10 community health centres
In July 2009 Amnesty International visited 10 CSPSs on the outskirts of Ouagadougouand spoke with medical staff.
• Each CSPS has at least one delivery table and four beds on average. Although most arein good condition, they are not covered with sheets and it is up to those accompanyingthe patients to bring cloths.
• Although all of the facilities have electrical equipment, electricity works in only one ofthe CSPSs. Even this CSPS does not have electricity all the time because of frequentpower cuts.
• Among the CSPSs without access to an electrical grid, eight have solar panels and onehas no electricity source at all. Medical staff told Amnesty International that solar energywas not reliable and only produced electricity for short periods. Furthermore, the wiringis faulty and does not extend to all the rooms in the health centre. Staff use torches andlamps for deliveries and those accompanying patients are sometimes asked to supply thisequipment.
• All the CSPSs are supplied with water by wells which belong either to the health centreor to the village. Where hot water is needed, the people accompanying the patient areasked to heat it.
• One CSPS uses a dry heat sterilizer, while the other nine sterilize their instruments withsteam from a pressure cooker or by using High-Level Disinfection (HLD) which is the normin health centres without electricity.
• Six CSPSs indicated that they regularly suffered shortages of medical products (nopharmaceutical outlet, no iron for pregnant women, worn out blood pressure meters, noweighing scales), as well as shortages of cleaning products (bleach, liquid soap, alcohol,gloves and protective material). Restocking takes a very long time.
SHORTAGES OF STAFF AND SUPPLIES
SHORTAGES OF DRUGS AND MEDICAL EQUIPMENT
In many of the health facilities visited by Amnesty International, some essentialsupplies were damaged or missing. In addition, many medical staff complained ofinterruptions to supplies and delays in restocking drugs and equipment.
SHORTAGES OF EQUIPMENT AND DISREPAIR
At al levels of the maternal health care system, there are shortages of beds anddelivery tables. In several CSPSs visited by Amnesty International, the delivery tableswere rusty or damaged. A nurse working in a rural CSPS told Amnesty Internationalthat "the delivery table is so uncomfortable and dirty that women prefer to deliver onthe ground."
Many women interviewed by Amnesty International said that tables were not cleanedbetween deliveries and that the pregnant woman's companions (sisters, mother,friends) were asked to wipe down the beds and wrap the newborn babies with theirown cloths or soiled linens. At least two women living in a rural area nearOuagadougou remembered being placed on a soiled delivery table upon whichanother woman had just given birth. These unhygienic conditions are placingpregnant women and their newborn at risk of infection.
The lack of delivery tables can be seen right at the top of the health system. In theuniversity hospital in Bobo-Dioulasso, medical personnel told Amnesty Internationalin March 2009 that there were only two functioning delivery tables and a doctor said,"If both tables are occupied, the woman who waits to be delivered has to be lucky."
SHORTAGES AND POOR QUALITY OF MEDICAL SUPPLIES
In many CSPSs visited by Amnesty International, medical staff complained thatsupplies were of poor quality, especially instruments to measure blood pressurewhich often lasted no longer than three months. Many stressed that they lackedessential medical supplies such as gloves and syringes, sometimes for months at atime. These two items are essential in preventing the transmission of disease. Severalnurses told Amnesty International that they had only one pair of scissors or a smalnumber of clamps that they had to sterilize after each use, causing delays.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
SHORTAGES OF DRUGS
Amnesty International visited pharmacies in some CSPSs and district hospitals wherestaff said that there were frequent shortages of drugs such as iron, used to treatanaemia, and anti-malarials.
A midwife working in Ouagadougou said in March 2009:
generic medicines to prevent haemorrhages are missing. There are not anysterile gloves. The midwives have to bring their gloves with them in their
handbags. There are often supply breakdowns. We have delivery kits without anysterile gloves, no bleach, no alcohol… We keep on making demands for the stocksto be replenished, but there are no responses to the grievances that are made andthe personnel cannot do anything more."
Stock shortages could result from a shortage at the central level or from poor stockmanagement in the health facility itself. As a Burkina Faso health system expert putit, "sometimes people wait until the last vial has been used before they make anorder". She went on to say:
care or bad usage. For example, concerning rusted delivery packs it's often acase of poor knowledge of disinfection solutions before the sterilization takes
place (over-concentrated solution, too long soaking time, poor rinsing, etc. whichdamages the equipment). All aspects of sterilization are neglected and are rarelysubject to quality control. Furthermore, in some health facilities, doctors and thosein charge of managing the treatment centre only give medication or medicalmaterial sparingly because they know that if material was given all at once there'sa chance it could be broken or disappear into thin air to be resold to patientsillegally or recycled for a fee in private clinics."
SHORTAGES OF STAFF AND SUPPLIES
RECURRING BLOOD SHORTAGES
Haemorrhage is a primary cause of maternal mortality in countries worldwide. Urgentaccess to compatible and safe blood is essential.
The government of Burkina Faso has made real efforts to improve the quality andquantity of available blood. A national policy on blood transfusion162 was adopted toensure that blood for transfusion is col ected and kept according to WHO standards.163Two national blood transfusion centres (NCBTs) were created in Ouagadougou andin Bobo-Dioulasso in 2005 and two more were created in 2008 in Fada and inKoudougou. The government also increased the budget for the NCBTs fivefold, fromsome 200 mil ion CFA francs in 2005 to 927 mil ion CFA francs in 2009 (from aroundUS$457,000 to US$2.1 mil ion).164
These four national blood transfusion centres are responsible for supplying regionaland district hospitals with blood. However, they are unable to provide a nationalservice as they cannot supply blood to three health regions (North, Sahel and South-West). Even in the regions covered by the blood transfusion centres, the supply is notalways regular. For example, Amnesty International was told by medical staff that theblood transfusion centre in Bobo-Dioulasso can only provide blood "from time totime" to the regional hospital in Banfora, the one in Kodougou can only supply blood"from time to time" to the regional hospital in Dédougou and the blood transfusioncentre in Fada can "rarely" supply the regional hospital in Tenkodogo.165
Shortage of blood is particularly critical during the rainy season because of theincidence of paludal anaemia (anaemia as a consequence of malaria) and becauseit coincides with vacations for schools and universities (students are the largest groupof blood donors). During this period, the blood transfusion centre in Ouagadougouonly manages to obtain 60 units of blood a day, less than half of the needed150 units a day.
The fact that the four blood transfusion centres cannot supply al the regional hospitalsand district hospitals is very serious, as these health facilities often do not have therefrigerators and equipment to collect and preserve blood safely. According to aspecialist on blood transfusion in Burkina Faso, the hospitals do what they can tomanage without the national supply: "The blood is tested; however they maketransfusions with what is at hand, without being able to respect the WHO internationalstandards that stress that the entire blood must not be given. It must be split intovarious components (red blood cel s, plasma, and plaques) and only the componentneeded should be transfused."
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Some health facilities cannot have blood banks because of lack of electricity. Forexample, a district hospital some 100km west of Ouagadougou visited by AmnestyInternational in July 2008 had no blood bank as it had not had regular electricitysupplies since May 2007. A doctor working there said:
blood. There is a problem of compatibility and even if we can find compatibleblood, it may not be in sufficient quantity for a particular patient."
Amnesty International has documented many cases where the relatives of a pregnantwoman have been asked to give their own blood.
Maïmouna died in August 2007 of haemorrhage and lack of blood.
Maïmouna lived in a village 5km from the nearest CSPS in a district 200km fromOuagadougou. During her pregnancy, she regularly visited the CSPS. After giving birthat the CSPS, Maïmouna started bleeding and was told that she needed a bloodtransfusion and had therefore to be transferred to the regional hospital, 30km away.
Maïmouna's husband told Amnesty International in March 2009: "When we reached theregional hospital, the doctor told us that my wife needed a transfusion but they had noblood; I offered to give her my blood but it was incompatible. I went to get my parents,who live in this city, but their blood was also incompatible. The medical personnel offeredto help me, but their blood was also incompatible. Despite other searches during the nightof Saturday till Sunday, we did not find anything. Around 7pm, my wife died withoutreceiving any blood transfusion."
SHORTAGES OF STAFF AND SUPPLIES
LACK OF TRAINED MEDICAL PERSONNEL
Although there has been an increase in medical personnel in the last five years, thereare stil not nearly enough qualified medical staff in Burkina Faso. The number ofregistered midwives grew from 504 in 2004 to 697 in 2008166 – one midwife for about21,000 inhabitants, wel short of the standards set by the WHO of one midwife for5,000 inhabitants. The number of physicians also increased from 359 in 2004 to473 in 2008 (including around 70 gynaecologists), a ratio of one physician for about31,000167 inhabitants whereas the WHO standard cal s for one physician per 10,000inhabitants.
This lack of trained medical personnel is exacerbated by the fact that health careproviders are not evenly distributed throughout the country. For example, in 2007, theCentral Region with a population of 1,560,049 had 44 doctors and 199 midwives atthe district level, while in the Northern Region, with a population of 1,156,207, therewere only 10 doctors and 16 midwives.168 These staffing levels meant that in 2007 inthe Central Region there was one midwife for every 3,000 women of child-bearing age,while there was only one for every "20,000 and more" women in the NorthernRegion.169
One of the primary reasons for the uneven distribution in qualified personnel is thedifficult conditions for health staff in rural areas, where they work alone, withoutessential materials and new technologies. General y speaking, qualified personnelare reluctant to go to rural areas and this is particularly true for female midwives.
Most are unwil ing to work outside cities because they are usual y married to a manwho works in a city and the women want to remain with their family. To address this,the government created a new body of male midwives, cal ed "maïeuticiens d'Etat",but they are deployed at the district level, leaving only auxiliary midwives at thecommunity level.
The UN Special Rapporteur on the right to health has stated that the right to healthentitles women to reproductive health care services, goods and facilities that areavailable in adequate numbers: "…this gives rise to an obligation on States to ensurean adequate number of health professionals. Improving human resource strategies,including increasing the number of health professionals and improving terms andconditions, is a vital prerequisite for reducing maternal mortality in many countries."170
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
LACK OF SKILLED BIRTH ATTENDANTS
Skil ed care at delivery for al women has been identified as one of the three maincomponents of any strategy to reduce maternal mortality, together with contraceptiveservices to prevent unwanted pregnancy, and emergency obstetric care for al whoneed it.
Skilled attendance at birth: a definition171
A skilled attendant is an accredited health professional – such as a midwife, doctor ornurse – who has been educated and trained to proficiency in the skills needed to managenormal (uncomplicated) pregnancies, childbirth and the immediate postnatal period,and in the identification, management and referral of complications in women andnewborns.
Skilled care refers to the care provided to a woman and her newborn during pregnancy,childbirth and immediately after birth by an accredited and competent health careprovider who has at her/his disposal the necessary equipment and the support of afunctioning health system, including transport and referral facilities for emergencyobstetric care.
In order to guarantee skilled care at birth, it is essential that the training level ofmedical staff, notably midwives and auxiliary midwives, is of sufficient quality and issubject to constant revision and improvement.172
However, the training of these key medical personnel suffers from long-runningproblems. A Burkina Faso health system expert told Amnesty International:
schools, underpaid professors, few teaching materials, lack of logistical orfinancial means enabling instructors to follow their students where they do
their professional training."
Auxiliary midwives at the CSPS level constitute the first level of care for nearly alpregnant women, especial y in rural areas where midwives are not available. In theabsence of the head nurse (infirmier major), it fal s upon them to take the decisionto refer the pregnant woman in case of a complication.
The level of training of auxiliary midwives is subject to debate in Burkina Faso. Someexperts say that they can deal with simple deliveries and are able to refer pregnant
SHORTAGES OF STAFF AND SUPPLIES
women with complications to the referral centres. Others, including severalgynaecologists working in the university hospitals in Ouagadougou and in Bobo-Dioulasso, feel that many auxiliary midwives are not competent to recognize signs ofdanger. A researcher from the Bobo-Dioulasso MURAZ centre told AmnestyInternational delegates:
care, a midwife is the benchmark health professional. In Burkina Faso, 80 to90 per cent of the health facilities only have auxiliary midwives to carry out
the deliveries. This category of health professional is not recognized on aninternational scale by the WHO as being able to guarantee qualified assistanceduring delivery. We should carry out a complete evaluation of competencies of thistype of medical personnel and increase the required level of training. This is muchmore worrying as a mistake when making a diagnosis in a CSPS can delay the on-time transfer to an appropriate health care facility."
In addition, it seems that partographs173 – one of the essential protocols in terms ofquality of care – are not always used. For example, Amnesty International was ableto see the medical record of a near-miss in March 2009 where the partograph wasblank. A nurse in a rural area told Amnesty International, "despite the fact that theuse of partographs is taught during our training, some health workers fail to use it. Thisis worrying as the partograph can be a critical tool to decide when to refer a womanto a higher level health centre." An expert on the Burkina Faso health system toldAmnesty International that "some midwives fil the partograph after the delivery whenit's useless, in order to insert it in the medical record and avoid any reproach".
Some Ministry of Health officials that Amnesty International met in March 2009recognized that the training of auxiliary midwives was insufficient, and stated that inorder to make up for these shortcomings, the government had just created a newintermediate category of qualified midwives (accoucheuses brevetées). The entryrequirement for the two-year training is several years' experience in the role of auxiliarymidwife, plus the Brevet d'étude du premier cycle, an entry-level diploma.174 One ofthe officials told Amnesty International that the first cohort of qualified midwives(around 50 people) was due to qualify in mid-2009 and that they would be appointedto district hospitals. The level of treatment in CSPSs, where the large majorityof women give birth, wil not therefore benefit directly or immediately from this newtraining programme.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
9/SUB-STANDARD CARE
‘IN CHILDBEARING, WOMEN NEED A CONTINUUM OF CARE TO
ENSURE THE BEST POSSIBLE HEALTH OUTCOME FOR THEM AND
THEIR NEWBORNS… THE SUCCESSFUL PROVISION OF THE
CONTINUUM OF CARE REQUIRES A FUNCTIONING HEALTH CARE
SYSTEM WITH THE NECESSARY INFRASTRUCTURE IN PLACE,
INCLUDING TRANSPORT BETWEEN THE PRIMARY LEVEL OF HEALTH
CARE AND REFERRAL CLINICS AND HOSPITALS. IT ALSO NEEDS
EFFECTIVE, EFFICIENT AND PROACTIVE COLLABORATION
BETWEEN ALL THOSE INVOLVED IN THE PROVISION OF CARE
TO PREGNANT WOMEN AND NEWBORNS.'WHO, International Confederation of Midwives and the International Federation of Gynaecologyand Obstetrics175
Besides shortages of staff and supplies, two key issues undermine the quality of carereceived by pregnant women in Burkina Faso: serious failures in the referral systemand difficulties in the relationship between patients and medical personnel.
SERIOUS FAILURES IN THE REFERRAL SYSTEM
The referral system is the basis of a functioning health system, al owing complicationsto be treated at a higher level of care. This system has been adopted in Burkina Faso,where CSPSs can only carry out normal deliveries and have to refer to a higher tier(district, regional and university hospitals) any pregnant women suffering fromcomplications.
This referral network is undermined by several deficiencies, in particular:
� delays in making the decision to refer a patient
� lack of emergency capacity in district and regional hospitals
SUB-STANDARD CARE
A woman in labour with her first child lies in thecorridor in the maternity ward. With space for only sixbirths at a time, women have to wait to enter the labourward until the birth is imminent. Yalgado hospital,Ouagadougou, Burkina Faso.
� blood shortages
� lack of ambulances for transferring pregnant women
� no communication between health facilities
Because of those problems, many women are referred to the two university hospitalsin Ouagadougou and Bobo-Dioulasso, which leads to delays that can have fatalconsequences. Some doctors working in the two university hospitals told AmnestyInternational that many women have been referred too late. An obstetrician from theYalgado hospital in Ouagadougou stated: "Some women arrive in a hopeless stateand sometimes they are already dead when they arrive."176
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
DELAYS IN REFERRAL DECISIONS
Delays in making the decision to refer a patient can stem from staff in the CSPS notrecognizing the urgency of the woman's situation or from difficulties in finding suitabletransport.
Sometimes the member of staff able to take the referral decision is absent. Thehusband of a woman who died in August 2007 told Amnesty International:
12km from our home. We spent Friday night at the health centre and the nextday, Saturday, around 11.30am, my wife gave birth to a boy. The baby was
delivered by an auxiliary midwife. Just after the delivery, my wife began to shakeand wasn't well. We had to wait until the arrival of the head nurse to take thedecision to transfer her. He came back six hours later and as soon as he saw her,he said that she should be immediately transferred to the regional hospital."
This woman final y arrived at the regional hospital at 7pm, where the doctor said thatshe needed a blood transfusion. As there was no blood bank in this hospital and nocompatible blood among members of the family, she should have been transferredimmediately to the university hospital of Yalgado but it was too late and she died a fewminutes later.
LACK OF EMERGENCY CAPACITY IN DISTRICT AND REGIONAL HOSPITALS
Some district and regional hospitals refer patients to university hospitals because theysimply do not have the capacity to operate on pregnant women with complications.
Sometimes the surgeon is absent, or the operating room is not functioning becausethe generator is broken or there is a problem of sterilization. So, in Ouagadougou,out of four urban district hospitals, only one, (the Sector 30 district hospital, CMA),operates day and night. The emergencies which arise in the other district hospitalsare partial y managed by the Sector 30 district hospital and mostly by the Yalgadouniversity hospital which, because of this, is severely overcrowded.177
BLOOD SHORTAGES IN DISTRICT AND REGIONAL HOSPITALS
Problems arise in the referrals system because the university hospitals inOuagadougou and Bobo-Dioulasso receive many women who cannot be treatedin district or even regional hospitals because of a lack of compatible blood(see Chapter 8). A doctor working at a regional hospital told Amnesty International:
SUB-STANDARD CARE
blood. If we cannot find compatible blood, we transfer the patient toOuagadougou, which causes delays that can be life-threatening."
LACK OF AMBULANCES FOR TRANSFERRING PREGNANT WOMEN
The lack of ambulances is another real problem, causing potential y dangerous delaysin referrals (see Chapter 6). Al the district hospitals visited by Amnesty Internationalhad one or two ambulances, but in some of them, one of the ambulances did notfunction, posing real problems when there were two emergencies at the same time.
Assetou, aged 25, died in January 2008 while trying to reach a health facility.
Assetou was married at 21 when her grandparents organized her marriage to Alassane,born in 1964 and the father of four children born to a first wife. Assetou never went toschool. The family lives in a village with a CSPS, about 16km from the regional hospital.
During her pregnancy, Assetou attended prenatal visits at the CSPS. In January 2008,Assetou had pains and went to the health centre but was told to come back later. Thenext day, she again had contractions, and she was accompanied back there by womenfrom the village. Assetou delivered at around 3am but the baby did not survive. At 9amshe went back home with her husband. She went to rest, but two days later, she stoppedeating. A woman neighbour who cared for her told Amnesty International, "Assetou saidthat she felt as if there were cinder in her stomach." The following day, this neighbouraccompanied Assetou to the CSPS where she was given a prescription that her husbandpaid for.
After having spent the night at the CSPS, a nurse said that she had to be evacuated tothe regional hospital but the ambulance was broken ("elle était gatée") and staff told thefamily that "they had to figure out how to get there." Alassane's youngest brother tookAssetou on his small motorcycle. Alassane told Amnesty International: "She was holdingonto him and as a precaution, we tied a piece of cloth around her and the motorcyclist.
I drove another motorcycle."
The brother said: "At a certain point, I noted a certain imbalance, I felt the release ofher hands, and I was no longer carrying the weight of her body. I stopped and thenI realized that she had rendered her soul. There was blood on my motorcycle."
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
NO COMMUNICATIONS BETWEEN HEALTH FACILITIES
Another problem raised by several doctors is the lack of any system of communicationbetween health facilities at different levels. An obstetrician from the university hospitalin Yalgado said:
task easier as we could prepare ourselves to cater for them. We shouldintroduce a system of communication to help us to maintain telephone links
between the different health facilities."
The aunts of a young woman in labour wait patientlyoutside the delivery room at a new community healthcentre (CSPS) in Gorgare, Burkina Faso.
SUB-STANDARD CARE
PATIENTS AND MEDICAL PERSONNEL:
RELATIONSHIP DIFFICULTIESDuring its four research missions, Amnesty International observed the professionalismand commitment of medical personnel both in towns and rural areas. However, thedelegates also col ected a number of accounts il ustrating worrying negative attitudestowards pregnant women and their families. This can be partly explained by the lackof motivation and work overload among many medical personnel.
LOW MORALE AMONG HEALTH STAFF
Al the medical staff who met Amnesty International underlined that low public sectorsalaries were detrimental to the quality of treatment and led to the partial or totaldeparture of competent and trained people to the private sector. A medical professorfrom Bobo-Dioulasso told Amnesty International that the starting salary for a nurse is50,000 CFA francs per month (around US$114). "To make ends meet, they stay inthe public sector in the morning then do private work in the afternoon." Agynaecologist told Amnesty International that by spending two afternoons in theprivate sector, doctors could double their wages.
The need to offer competitive salaries to medical staff so that they can stay within thepublic health service has been stressed by some international bodies. The CESCR hasstated: "Functioning public health and health care facilities, goods and services, aswel as programmes, have to be available in sufficient quantity… These facilities,goods and services should include hospitals, clinics and other health-relatedbuildings, trained medical and professional personnel receiving domesticallycompetitive salaries, and essential drugs."178
A midwife met by Amnesty International in July 2008 in a town 100km north ofOuagadougou highlighted another factor which explains why experienced midwivesare leaving the profession: "The basic wage for midwives varies between 75,000 and80,000 CFA francs (around US$171 to 183). To live comfortably, you have tospecialize. However there is no specialization in obstetrics. Therefore lots ofexperienced male and female midwives take exams to specialize in surgery,anaesthesia, ENT [ear, nose and throat] or in paediatrics. Because of this we're losingthe most experienced and competent people and we constantly have to train newrecruits."
This is about to change as a new programme has just been set up to al ow midwivesto progress in their careers.179
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
NEGATIVE ATTITUDES TOWARDS PATIENTS AND THEIR FAMILIES
Many of the families that Amnesty International spoke to criticized the attitudes ofnurses, midwives and auxiliary midwives who treated them rudely and evensometimes violently. When a woman dies in childbirth, medical staff rarely reveal thecause of death and in certain cases treat the family of the woman brusquely,especial y families living in poverty and with a low level of education.
In almost al the maternal mortality cases that Amnesty International investigated, themedical staff did not tel the family the cause of death. Members of families living inpoverty often do not dare question medical staff, but many bereaved husbandsregretted not knowing how their wives died. A farmer told Amnesty International:
visits. They never told us that there was a problem during the pregnancy. Shewas taking medication, but I don't know what. I went with her to the health
centre for the birth. I was told to wait. Then a nurse came and told me it wasn'tgoing well. He asked me if my wife had an illness. I told him that she was healthy,since she had been coming to this health centre and there hadn't been anyproblems. He came back some time later and told me simply that my wife had died.
I don't know why she died. Nobody told me. I didn't dare ask why but I'd really liketo know."
There are also cases where the personnel treat a bereaved family disrespectful y.
A mechanic, whose wife was treated in a health facility in Ouagadougou before shedied in April 2008, told Amnesty International:
asked me to buy an empty carton. I returned to the maternity ward with it. Afew minutes later, the male nurse came back out with the carton, in it there
was the stillborn baby. He told me to bury the child, and then to come back."
NEGLIGENCE AND VIOLENCE DURING LABOUR
Amnesty International col ected a number of testimonies from mothers who said thatthey had been victims of carelessness, neglect and even violence in health facilities.
Women reported being insulted and being pinched on the thighs, slapped or beateninto compliance during labour. They also said they were left alone for hours. Otherwomen described rough, painful, and degrading treatment during physicalexaminations and delivery, as wel as verbal abuse from medical staff if they expressedpain or fear.
SUB-STANDARD CARE
Aïcha was verbally abused and slapped during labour.
Aïcha sells jewellery in the market. The mother of a two-year-old son, she told AmnestyInternational how she was treated during her first delivery in May 2005. She eventuallyhad a caesarean section and delivered a stillborn baby:
"It was my first delivery. I arrived at the district hospital at 5pm with my mother-in-law,and I was told that I would deliver at 9pm. On the second day, the baby had still notarrived. We were told to go do a sonogram at the hospital so my husband took me backto the hospital. On the delivery table, the midwife asked me to yell but I said that Icouldn't do it because I was too tired. Then all of the maternity personnel left, they toldme that they had to go to a baptism. I felt abandoned. There were no more medicalpersonnel that afternoon. So we had to wait for the night shift to come, at midnight.
Suddenly, I saw the umbilical cord come out and I thought that it was my internal organs.
So I thought that I was going to die. A midwife arrived and said ‘You shouldn't cry',‘When you were doing the thing with your husband, you were happy' and sheslapped me."
A number of women told Amnesty International that midwives, especial y auxiliarymidwives, were very impatient and occasional y insulted them when they were in painand asking for help. During a focus group discussion in Ouagadougou in March 2009,a woman told Amnesty International that when she gave birth at a CSPS in the capital,she was told aggressively by a midwife: "I am a woman, I know what it is to give birth,open up, spread your legs, it is not painful."
Women reported that midwives and auxiliary midwives did not pay attention to themand were doing other things such as knitting while they were suffering on the deliverytable.
Several doctors said that they were aware of such practices. One of them witnessedverbal abuse from several midwives. "I saw one midwife say to a woman in labour:‘You're hopeless, you're unbearable, you're dirty, go and wash yourself before youcome.' If the woman in labour is accompanied, she is protected." A male nurseadmitted to Amnesty International in July 2008 that he "occasional y had to slap orpinch pregnant women because they don't want to push and this can cause the deathof the baby."
It is difficult to assess how common such cases are. Staff are working in stressfulconditions and may be provoked by the family. A midwife working in Ouagadougoutold Amnesty International:
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
in our work; they press for their relative or friend to be treated first while thecase of other women is more urgent and they often want to attend the delivery
which causes a lot of disruption. I was once slapped by a woman because her friendwas not immediately treated whereas other women needed more urgent care andthere weren't enough personnel to take care of so many pregnant women at thesame time."
Whatever the provocation, however, acts of verbal or physical violence by medicalstaff cannot be justified or condoned.
When Amnesty International raised these cases with the authorities and medicalpersonnel, the response was that these were isolated cases, although there was somerecognition that they could occur because of the pressures on staff. AmnestyInternational remains concerned by the lack of control over staff behaviour and thefact that such practices are not subject to disciplinary sanctions, which can onlyperpetuate them.
SUB-STANDARD CARE
Pilot project to improve quality of care: Sector 30 in Ouagadougou
A pilot project – Amélioration de la qualité et de l'accès aux soins obstétricaux d'urgence(AQUASOU, Improvement of the quality and access to emergency obstetric care) – waslaunched in 2003 in the district hospital in Sector 30 in Ouagadougou, with support fromthe French Ministry of Foreign Affairs. One of the objectives of the AQUASOU project wasto improve the quality of obstetric care: technical quality and also interpersonal quality,since the analysis of the situation brought up frustrations and lack of understanding fromboth users and providers. Users complained of a poor reception and sometimes badtreatment and health staff complained about women arriving too late and of a lack ofrespect for visiting hours from friends and family.
Several initiatives have started to improve the carer-patient relationship:
� Home visits for women who have had a caesarean section so that midwives can
see the women's living conditions and ensure they have the information they need;
� Users-providers meetings to improve interpersonal relationships;
� Reinforcement of midwife training, with the aim of "developing health professionals
so they pay greater attention to people's personal experiences in order to providemore patient-centered care."180
When the project ended in 2006, several key objectives seemed to have been achieved,notably in terms of improving relations between users and health staff. Questionnairescompleted at the end of this project showed that the majority of women were very satisfiedwith their care. Many said that: "We were quickly taken care of", "They respect us".
There was also better information for those accompanying the patient and betterorganization of visits.181
Those in charge of Sector 30 highlighted, however, that these successes had financialimplications. As one of the Sector 30 district hospital doctors pointed out to AmnestyInternational in March 2009, "We are victims of our own success. Some pregnant womenwho aren't originally from our Sector come to give birth here. As we perform a lot ofdeliveries and caesarean sections, the material quickly gets spoilt and we have to ensurethat there is a rapid renewal of equipment. The French government aid ended in 2006and that of the Italian government in 2007. Without external or state support we couldsoon be declared insolvent."
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Accountability is a key factor in any functioning health system. The government hasto account for the implementation of its health policies. Patients are also entitled tohold accountable medical personnel who might be responsible for abuses ormisconduct, such as unlawful demands for unofficial payments, and must haveaccess to avenues of redress. However, in Burkina Faso, accountability is rare, bothat government and individual level.
LACK OF MONITORING OF POLICY IMPLEMENTATION
Despite the many strategic plans and policies adopted by the government of BurkinaFaso to tackle maternal mortality, and health more general y, some key aspects ofthese policies stil need to be implemented.
During the 10-year period of the PNDS (2001-2010), the government published aseries of evaluation reports indicating the progress made and the gaps to be fil ed. InMarch 2004, the authorities acknowledged and identified very clearly the fol owingproblems in health care for pregnant women:
� limited accessibility and availability of maternal and neonatal care,
� low quality of care,
� insufficient co-ordination and col aboration within and outside the sector,
� and inadequate commitment of stakeholders at al levels.182
These problems were again highlighted two years later in a plan adopted bythe Ministry of Health in 2006, the Plan d'accélération de la réduction de la mortalitématernelle et néonatale au Burkina Faso (Plan to accelerate the reduction inmaternal and neonatal mortality in Burkina Faso), also called the "roadmap"(feuil e de route).183
Many of these obstacles stil need to be addressed.
The death of a woman in childbirth deprives her familyof their daughter, sister, wife and mother. This is thehome of Sawadogo Mousa in Wonko, whose wife died inchildbirth.
An evaluation of the PNDS (2001-2010) was underway at the time of writing thisreport. The terms of reference for this evaluation were adopted in June 2009,international and local consultants were hired and the evaluation report was due tobe ready by the end of 2009. In a meeting with officials from the Ministry of Healthin November 2009, Amnesty International was told that a workshop was planned forJanuary 2010 to consult representatives of civil society, partners and the privatesector.
FAMILY PLANNING: THE UNMET NEED FOR CONTRACEPTION
Despite efforts to make contraceptives available to al women since the launch of theContraceptive Security Strategic Plan (2006-2015), contraceptive use remains lowand too many women have unmet needs for contraception. The Reproductive HealthProducts Security Strategic Plan (2009-2015) acknowledges the existence ofweaknesses in the supply and storage of contraceptive products. In this document,the authorities stressed that: "Logistical management shows insufficiencies in termsof availability of reliable and timely information in order to estimate needs at al levels.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Hence risks of stock shortages, expiration, damage or over storage. The informationgathering system is. not functional for family planning."184
SHORTAGES AND MISAPPROPRIATION OF DRUGS AND MEDICAL SUPPLIES
Stock management of drugs and medical supplies is a very serious problem in manycountries, including Burkina Faso. As a doctor from Burkina Faso told AmnestyInternational in March 2009: "Al policies aiming at the exemption of costs must beaccompanied by a mechanism of stock control and sanctions for people stealing ormisappropriating money or medical goods belonging to the public service." Suchmechanisms do not exist or do not function effectively in Burkina Faso.
The issue of stock shortages was acknowledged in the PNDS, which states that inorder to make medicines more available, the Ministry of Health would "oversee thesupply and distribution of essential generic medicines in al health districts to avoidstock shortages."185 In practice, throughout the health system, this does not appearto be the reality.
For example, information col ected by Amnesty International shows that the kits fordeliveries, which are prepared by a person in charge of stock management, are oftenunavailable or incomplete and no real system of stock management seems to be inplace. This al ows misappropriation of medical materials, and can lead to al egedshortages of supplies, which means that patients' families have to pay for "missingproducts".
The government must take more determined and robust action to improve the supplyand control of necessary drugs and medical supplies to ensure that they are availableand cannot be misappropriated.
ACCOUNTABILITY OF MEDICAL PERSONNEL
In many health facilities, the performance, attendance records and attitudes ofmedical staff are rarely subject to checks and controls from doctors or managers. Althe information gathered by Amnesty International shows that medical personnelresponsible for abuses and misconduct against patients are rarely, if ever, held toaccount.
CHARTER OF PATIENTS' RIGHTS
Amnesty International's research has found that the relationship between medicalstaff and patients and their families may be strained. Relatives are often not told thecause of death or of serious complications related to childbirth. A patients' Charter wasadopted by the Ministry of Health in 2007 and stressed that, "Any health services'user is entitled to be wel received and to benefit from quality care".186 However, thisCharter is not displayed in hospitals and other health facilities and is very little knownby patients or medical personnel. There is a regional charter concerning the dutiesand behaviour of midwives,187 but no such text exists at the national level.
All the testimonies collected by Amnesty International indicate that patients areunaware of their rights, including the right to information and the right to be treatedproperly and with respect by medical staff.
LACK OF SANCTIONS
The PNDS stressed the necessity to "enforce sanctions for misconduct"188 committedby medical personnel. Although there is a disciplinary procedure provided by theprofessional doctors' organization,189 Amnesty International did not find evidence thatmedical personnel accused of corruption or inappropriate treatment of patients,including physical and verbal abuse, were effectively punished.
Amnesty International met several doctors who acknowledged that such abuses werecommitted and that nothing had been done to penalize the person responsible. Adoctor working near Bobo-Dioulasso told Amnesty International in March 2009:
pregnant women: ‘Give me some money, I am going to give it to the doctor tomotivate him.' When I heard about it, I was furious, I summoned the male
nurse. He apologized but there was no penalty."
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Another doctor cited the case of a hospital porter who put a patient in the corridor ofa hospital in Ouagadougou and told the pregnant woman's family: "if you don't pay2,500 CFA francs (around US$5.50), I'll leave her here." The doctor added:"Everybody knows cases like this but no one wants to denounce them as this mightcreate problems within the health facility."
Officials working at the Health Ministry acknowledged that there were some "blacksheep" (brebis galeuses) among the medical staff but stressed that these wereisolated cases and that once these cases were known, "everything went back tonormal." They also told Amnesty International in November 2009 that if patients feelthat their rights are not being respected or they have paid unjustified amounts ofmoney, they can ask for redress through different services, either at the medical orthe administrative level. However they acknowledged that "there are in fact very fewcomplaints due to cultural barriers."190
INVESTIGATING MATERNAL DEATHS AND NEAR-MISSES
At the national level, every maternal death should be investigated by a team sent bythe Ministry of Health, but an official of the Ministry of Health wrote to AmnestyInternational in November 2009 that audits of maternal deaths are being organizedat the referral level and that guidelines were sent to health facilities in 2008.191However, this practice is not implemented in every district hospital and no inquiriesinto maternal deaths are carried out at the community level. In addition, it is unclearhow these investigations are to be carried out and what fol ow-up they entail.
At the level of the health facility, several medical centres organize a monthly audit,either on one case of maternal death (Yalgado university hospital) or on a case ofsevere maternal complication or a stil born baby (district hospital Sector 30). A file ischosen at random and al the medical staff concerned (gynaecologists, midwives andnurses) analyse the case. The aim is to learn lessons from past mistakes and to makerecommendations while avoiding stigmatization: "No name, no blame, no shame."
These audits are important because they can be used to determine the factors leadingto maternal deaths, and establish policy priorities for change. Audits are not meantto assign blame for past maternal deaths, but rather to facilitate prevention of futuredeaths and learn how to manage severe complications without delays.192
Audits: Learning lessons from past mistakes
In March 2009, the head of the maternity department in Yalgado invited the AmnestyInternational delegation to take part in one of its monthly maternal death audits. Formore than three hours, the case of a woman who died a month earlier was examined. Thedelegates were impressed by how serious and transparent the debates were, as well asby the quality of the report of the discussions which was transcribed on a computer andshown on an overhead projector.
During this audit, all possible failures were scrutinized and discussed, including delaysin referral, transport difficulties, and failings in medical care, such as delays,misdiagnosis, lack of blood or insufficient attention. The whole group maderecommendations which had to be implemented by one or more of the members of staffwithin a given time.
Maternal death audits are not always easy to carry out. Without a minimum level ofequipment and human resources, audits cannot improve the quality of care. Medicalstaff must share the desire to change practice and be prepared to reveal mistakes infront of a peer group. Confidentiality cannot be guaranteed in teams which knoweach other wel ; members of staff recognize the case even if the patient's name is notrevealed. Unless recommendations are implemented, they are of no use and caneven demotivate staff.193
ABSENCE OF EFFECTIVE REMEDIES
The CESCR has stated that anyone who is a victim of a violation of the right to healthshould have access to effective judicial or other appropriate remedies at both nationaland international levels. "Al victims of such violations should be entitled to adequatereparation, which may take the form of restitution, compensation, satisfaction orguarantees of non-repetition." It has also stated that "National ombudsmen, humanrights commissions, consumer forums, patients' rights associations or similarinstitutions should address violations of the right to health."194
In Burkina Faso, women and their families who are victims of violations of the rightto health have extremely limited access to avenues to make complaints and seekeffective remedies, either through the courts or by other means.
The right to health is one of the social rights enshrined in Article 18 of the Constitutionof Burkina Faso. However, virtual y the only way in which victims of violations of theirright to health can lodge complaints is to use the normal and very intimidatingadministrative and justice systems. They cannot bring complaints before the National
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Human Rights Commission (NHRC) of Burkina Faso as this body does not have thepower to receive and address individual complaints. Moreover the NHRC lacksindependence from the state authorities, a failure that was stressed in the conclusionof the Universal Periodic Review of Burkina Faso in January 2009 that asked thegovernment of Burkina Faso to "ensure that the statute of the national human rightscommission is in conformity with the Paris Principle, to ensure that it is ful y operational… [and] ensure its independence, particularly in adjusting its competences andfunding."195
There is, formal y, a complaints procedure which involves an official known as theMediator of the Republic, but this procedure is little known, particularly in rural areas,and Amnesty International is unaware of any cases related to maternal mortality takenthrough this procedure.
LACK OF POLITICAL WILL TO COMBAT CORRUPTION
Corruption by medical personnel, notably unofficial payments, has been identified asa major element undermining the whole health care system and in particular thesubsidy policy. It is therefore very worrying that, despite some pledges and the creationof anti-corruption bodies, the government of Burkina Faso seems to be doing very littleto tackle this major issue.
The government of Burkina Faso has made statements and undertaken legal duties atthe national, regional196 and international level in order to combat corruption. Under thePenal Code, corruption and influence-peddling in the public sector are criminalized,with penalties including imprisonment with fines and the removal of civic rights.197
The government has created several bodies in charge of monitoring and fightingcorruption and fraud, and in November 2007 the authorities set up the SuperiorAuthority of State Control (ASCE, Autorité supérieure de contrôle de l'État), whose aimis to rationalize and enhance efforts to combat corruption.198 The ASCE has the mandateto release annual reports from audited entities and has the authority to receivecomplaints from the public and investigate and prosecute ethics breaches in the publicsector, including by state civil service employees, local and public authorities, state-owned companies, and al national organizations invested with public service.199
However, the independence of this new entity is severely undermined by the fact thatit comprises only government officials and that it is run by a civil servant named by thegovernment and working under the authority of the Prime Minister. A prominentmember of civil society told Amnesty International:
a civil servant will immediately be transmitted to this person who might resortto retaliation. To be efficient, such a body should comprise members of civil
society, of the private sector, of the press as well as state officials and should benefitfrom state structures such as judges and police officials to carry out investigationsand judicial proceedings."
Members of civil society are also worried by the fact that the new ASCE discarded althe corruption cases identified by previous anti-corruption bodies that needed to bereferred to the justice system.
The general climate of impunity has been repeatedly denounced by REN-LAC, theNational Network to Fight Against Corruption (Réseau National de Lutte Anti-Corruption). In its 2006 report, REN-LAC stated that: "the ongoing absence of politicalinitiative and the reign of impunity make it so that corruption and the corrupt are gainingground, they are taunting the populations and dangerously compromising developmentand the democratic process."200
The UN Convention against Corruption, which Burkina Faso ratified in October 2006,expresses concern that corruption jeopardizes the rule of law and its Article 34 requiresfrom each state party to "take measures, in accordance with the fundamental principlesof its domestic law, to address consequences of corruption."201
The government has an obligation to address the problem of unofficial and unlawfulcharges by medical personnel and others charging for services, transport, drugs andsupplies, and to ensure that the limited resources Burkina Faso does have are properlyal ocated and reach their intended targets. Its failure to take adequate steps to addressthis problem contributes to serious violations of the right to health, including thepersistence of preventable maternal deaths.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
11/ROLE OF DONORS
For the last decade, under Burkina Faso's Poverty Reduction Strategy Framework,bilateral and multilateral donors have played a key role in supporting the country'shealth care policies and delivery.
SOURCES OF DEVELOPMENT ASSISTANCE
Donor support to Burkina Faso for the financing of the national health policy comes fromseveral sources:
� Funding from General Budget Support provided in support of the Poverty ReductionStrategy Framework.
� Funding through the Support program for the development of the health sector2008-2012 (PADS, Programme d'Appui au Développement Sanitaire), also called"pooled funding" or "basket funding".
� Direct support for specific projects or partners.
GENERAL BUDGET SUPPORT
General Budget Support provides development assistance which is not earmarked forspecific projects or items of expenditure, and which is disbursed through the recipientgovernment's own financial system, and in line with the recipient government's owndevelopment and poverty reduction strategies. Burkina Faso has received, andcontinues to receive, General Budget Support from a variety of bilateral and multilateraldonors, primarily Denmark, France, Germany, the Netherlands, Sweden, Switzerland,the European Union, the World Bank and the African Development Bank.202 In termsof the volume of assistance, the World Bank and the EU are the main donors, fol owedby the Netherlands.
Contributions made through General Budget Support are provided directly to thenational Treasury Account and mixed with the country's own revenues. They are thuspart of the budgetary al ocations to Ministries in accordance with the budgetary priorities
decided by the Burkina Faso government in its Poverty Reduction Strategy Framework,with donors and the government agreeing on minimum al ocations to priority sectors,including the health sector.
POOLED DONOR FUNDING FOR THE HEALTH SYSTEM
According to the latest available official figures, in 2006 donor funding contributed37.69 per cent of health spending on reproductive health, which comprises maternalhealth and family planning.203
The PADS is a pooled funding mechanism for support to the national healthdevelopment plan. The PADS is defined as "a joint initiative of the Ministry of Health andcertain partners in the development of the health sector, for a better coordination anda rational management of the resources mobilized for the implementation of thePNDS."204 In September 2009, the donors supporting this pooled funding mechanismwere the Netherlands (who are acting as lead donor in co-ordinating this fundingmechanism), Sweden, France, the World Bank,205 UNFPA, UNICEF, the Global Al iancefor Vaccines and Immunisation (GAVI) and the Global Fund to Fight AIDS, Tuberculosisand Malaria. This "basket funding" is managed by the Ministry of Health.
DIRECT SUPPORT FOR PROJECTS OR SPECIFIC PARTNERS
Donors also provide direct support for certain projects. For example, the AfricanDevelopment Bank (AfDB) is supporting loans at concessionary rates for thedevelopment of health infrastructure – hospital buildings, health centres, equipmentand also training of health care workers. The AfDB is also supporting the national healthaction plan in the eastern and northern regions of the country by building two regionalhospitals.
UN agencies also finance specific projects. UNICEF provides technical support for safemotherhood and child care interventions and intervenes through the Bil & MelindaGates Foundation for Maternal, Neonatal and Child Health Programme in two regions.
UNFPA supports access to family planning and provides technical assistance for sexualand reproductive health. A spokesperson for UNFPA told Amnesty International in June2009 that UNFPA contributed to spending linked to family planning to a sum ofUS$200,000 and financed the subsidy of contraceptive products by up to 80 per cent.
The WHO offers technical assistance in many areas including maternal health andHIV/AIDS.
Other donors also finance certain specific projects which have a direct link to reducingmaternal mortality. For example, the German agency GTZ focuses particularly on familyplanning, which it considers crucial in helping to tackle maternal mortality. In a meeting
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
with Amnesty International in July 2008, GTZ officials said that their action, which isconcentrated on the south-west and eastern regions, supports a programme on sexualhealth and human rights that focuses on family planning, sexual health andHIV/AIDS.206
AN APPROACH BASED ON GENDER EQUALITY
Some donors are also supporting the development and implementation of a genderpolicy to promote gender equality. This represents a priority for many internationaldonors such as Germany, Canada, Denmark, the Netherlands, Sweden andSwitzerland. Since 2002, about 20 donors have supported a gender consultationframework aimed at promoting gender equality in Burkina Faso by focusing on themessuch as the health and reproductive rights of women, gender and HIV/AIDS and thefight against domestic violence.
FACTORS REDUCING THE EFFECTIVENESS OF
INTERNATIONAL AID
In interviews with donor representatives and representatives of the government ofBurkina Faso, Amnesty International heard that the effectiveness of developmentassistance is hampered by insufficient co-ordination between donors and inadequateevaluation of the impact of development assistance for the health sector.
PROBLEMS OF CO-ORDINATION
There are more than 80 different funding sources for health sector activities in BurkinaFaso and there is a clear risk that some of these projects either duplicate each other orleave entire geographical areas unaddressed. Amnesty International was told ofinadequate co-ordination among donors in relation to support for the Burkina Fasohealth sector.
During a meeting with Amnesty International in March 2009, the Minister of Financeof Burkina Faso said that "it would be good to rationalize and to improve co-ordinationof the donors' interventions, because each donor wants to have their project and certainintervention zones are privileged in relation to others."
A representative of one of the main donors confirmed the existence of this problemand told Amnesty International in July 2009:
of action [agreements aimed at improving the delivery and effectiveness ofaid],207 on the ground this is still a dead letter. Too much energy is lost in high
transaction activities instead of using the very limited human capacity forconcerted actions aiming at the poor."
INADEQUATE OUTCOME EVALUATION
The government of Burkina Faso and donors have set up a series of mechanisms tomonitor and control the funds provided by donors. Since 2005 there has been anannual financial audit of funds provided to the PADS.
However, as an expert on the health system in Burkina Faso told AmnestyInternational:
evaluation' that could reveal the real impact of the work done on the ground.
The government does regular ‘output evaluation' of the activities financed by
donors and sends them reports so that aid continues to be provided. But there isno real and general assessment of the situation on the ground that could highlightthe needs and gaps."
Amnesty International learned that this issue was to be addressed by the introductionof a Health Sector Review System, a process that wil culminate in the first annualreview planned for March 2010. The outcome of this review wil feed into the annualreview of the Poverty Reduction Strategy Framework in April 2010.
Some NGOs have also underlined some of the gaps in the implementation of thePNDS. For example, the GAVI Alliance has noted "insufficient health programmonitoring and evaluation" and "insufficient planning and monitoring at theperipheral level."208
In this regard, some donors told Amnesty International that the evaluation ofthe implementation of the PNDS (2001-2010), due to take place in 2010, could bethe opportunity for a real assessment of the use of resources allocated to theimplementation of the PNDS.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
12/CONCLUSION AND
Over the past decade, the government of Burkina Faso has devoted significantresources to reducing the level of maternal mortality. With the help of internationaldonors and within a careful y planned framework, the authorities have focused oncommunity-level health care with the stated goal of increasing the number ofmedical y assisted deliveries.
According to official figures, progress has been made, notably in terms of reducingthe maternal mortality ratio and increasing the proportion of women who undergoprenatal consultations and have skil ed assistance in childbirth.
However, many pregnant women stil cannot obtain the health care they need in time.
They face many hurdles: women's subordinate status in society; geographical andfinancial barriers; poor conditions in many health facilities; shortages of staff and ofsupplies; negatives attitudes from some staff; and demands for unofficial paymentsby medical personnel. For the most marginalized women living in poverty, especial ythose in rural areas, pregnancy al too often ends in tragedy.
Family planning is a key component of any strategy for reducing maternal mortality.
The authorities of Burkina Faso have to improve the provision of information on sexualand reproductive health, and to ensure that sexual and reproductive health servicesare more accessible and available. Many women, especially adolescents, find itdifficult to have access to family planning services.
The subsidy policy, in place since 2006, represents a step towards dismantling thefinancial barriers that prevent pregnant women obtaining the health care they need.
However, significant problems remain. Women living in the most extreme povertycontinue to be confronted by financial barriers which take a heavy tol on their lives andon the lives of their children. The subsidy policy is not clear: few people know exactlywhat it covers and what treatments stil have to be paid for. That confusion al ows asituation where medical staff can demand unofficial payments for medicines andservices that should be free or subsidized. Amnesty International believes therefore thatmaking obstetric services, including emergency obstetric services, free of charge wouldhave a positive impact on access for al pregnant women, especial y the poorest.
CONCLUSION AND RECOMMENDATIONS
Final y, the authorities have to improve the quality of care by addressing shortages ofstaff and supplies, by improving the training of medical personnel and by putting inplace a real system of accountability able to tackle internal failures of the healthsystem such as stock shortages and misconduct by medical personnel.
Donors have a responsibility to sustain the efforts of the authorities of Burkina Fasoin their efforts to reduce maternal mortality. International aid has to be co-ordinatedso that the government and international and local NGOs can lead their projects in acoherent way. It should be predictable and stable, so that expectations are not raisedamong the public that cannot be met due to a sudden reduction in funds.
If the government, the donors and al the other actors, including NGOs, can act in acoordinated and accountable way, the progresses already achieved in the fight againstmaternal mortality wil be entrenched and many more preventable deaths of pregnantwomen wil be avoided.
Amnesty International urges the Burkina Faso authorities, and in particular theMinistry of Health, to ensure that the state meets its national and internationalobligations to respect, protect and promote the right to health, guaranteeing theequitable distribution of health facilities, goods and services, protecting the right ofaccess and eliminating economic and physical barriers. Amnesty International alsourges the Burkina Faso authorities to guarantee access to information on sexual andreproductive rights. The organization cal s on donors to cooperate closely with thegovernment in a long-term approach, ensuring access for al women to adequatereproductive health services, including emergency obstetric care.
1. ADDRESS DISCRIMINATION AGAINST WOMEN AND HARMFUL PRACTICES
The government has an obligation to take all appropriate measures to enddiscrimination against women in al its forms, including the elimination of customarypractices which are harmful to women, or which are based on stereotyped roles formen and women and reinforce the subordination of women. The government should:
� Review its national legislation to ensure that early marriages are forbidden and thatany discrimination between men and women regarding the age of marriage isremoved.
� Ensure that harmful customary practices such as FGM – prohibited by law – andearly and forced marriages are eliminated.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
2. EXPAND AND IMPROVE FAMILY PLANNING SERVICES
Ensuring access to family planning and contraceptive methods is a vital part of anystrategy for reducing maternal mortality. The government therefore should:
� Ensure that the 2005 Law on Reproductive Health is made a reality so that alwomen know their reproductive health rights.
� Undertake information and education campaigns aimed at both women and mento provide accurate, evidence-based, and comprehensive information aboutcontraceptives and to correct commonly held misconceptions. Such efforts shouldinclude sexual education aimed specifically at adolescents and publicity for theprovisions of the 2005 Law on Reproductive Health.
� Invest in an expansion of family planning services and information for al women,taking steps to ensure confidential access to such services and information for alwomen, including adolescents.
� Take al necessary measures to ensure that safe and legal abortion services areavailable, accessible, acceptable and of good quality for al women who require themin the circumstances as set out in national legislation.
� Repeal the provision of the Penal Code permitting the imprisonment of anyonewho carries out an abortion.
3. REMOVE FINANCIAL BARRIERS TO ACCESS TO MATERNAL HEALTH CARE
Despite the adoption of the subsidy policy, costs related to health care continue to actas a barrier to women's access to reproductive health services, including emergencyobstetric care. The authorities should therefore:
� Implement immediately and in ful the subsidy policy in al health facilities andcreate robust monitoring and accountability systems. Set up a centralized revenuecol ection system and a mandatory system of providing receipts for any paymentscol ected for services, supplies, transport and drugs.
� Consider introducing a total exemption from fees charged for services, drugs andsupplies for reproductive health services, including emergency obstetric care.
� Communicate the policy clearly and in an accessible manner in al parts of thecountry to create awareness of the exemptions under the policy. Consider setting upinformation points within health facilities to inform people of their entitlements underthe policy.
CONCLUSION AND RECOMMENDATIONS
� As a matter of priority, implement the subsidy policy for women who are entitledto a total exemption from costs related to health care by identifying and publicizingthe criteria to qualify for total exemption of costs. Create a transparent, participatoryand accessible system for women to claim the exemption.
� Publicize the policy on generic medicines and set up a monitoring system toensure that patients are not asked to pay for essential drugs.
4. IMPROVE THE AVAILABILITY AND ACCESSIBILITY OF REPRODUCTIVE
Most health centres, especial y in rural areas, cannot deal with complications linkedwith pregnancy and do not have functioning ambulances at their disposal to transferwomen to referral centres. The lack of proper communications between the primaryheath centres, the regional and university hospitals renders the referral system largelydysfunctional. Furthermore, there are wide disparities in the distribution of healthfacilities between different areas of the country. The authorities should therefore:
� Ensure the equitable distribution of health facilities, goods and servicesthroughout the country. When choosing locations for new health facilities and bloodbanks, prioritize the most marginalized sections of the population, who face thegreatest barriers in accessing health facilities.
� Increase the recruitment of qualified staff and create incentives to encouragequalified staff to work in rural areas and ensure that they receive adequate trainingand support. Ensure that these incentives promote an equitable distribution of skil edmedical personnel throughout the country.
� Set up a system for traditional birth attendants, women and their families to haveaccess to reliable forms of transport to health facilities, particularly in emergencies.
� Establish and strengthen links between health facilities by providing bettercommunications and transport equipment.
� Ensure that hospitals are ful y equipped to offer emergency obstetric care andthat they have proper ventilation, adequate supplies of electricity or alternative sourcesof power, drugs, blood and other materials necessary for providing care appropriateto their role within the health infrastructure.
� Ensure that the supplies and equipment necessary to maintain hygienicconditions are available and that hygienic standards are strictly enforced.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
5. ENHANCE MONITORING AND EVALUATION AND ENSURE
It is the responsibility of the government to address corruption and mismanagementwithin the health care system by establishing functioning, accountable institutionsand systems. Civil society needs to play an active role in monitoring and evaluatingthe health care system.
� The Ministry of Health should monitor practices in health centres to ensure thatinformal and inappropriate fees are not levied.
� The Ministry of Health should strengthen norms and procedures aimed atensuring that health care facilities are welcoming and respectful to all groups ofwomen and young adolescents.
� The implementation of the PNDS should be monitored by mechanisms whichprovide for the involvement and participation of women who use reproductive andmaternal health services, other community members and civil society in planning,monitoring and evaluation processes.
� Monitoring, evaluation and accountability mechanisms should be strengthened,including through systems to combat corruption and mismanagement inprocurement, storage and distribution of drugs and supplies. Any complaintmechanisms should be readily accessible to people and wel publicized.
� Concerted efforts must be made at the district, regional and national levels toaccurately assess the number of women dying and the reason for their death inboth communities and in health facilities. The Ministry of Health should take thisinformation into account in devising policies and strategies to reduce maternal death.
Relevant health care staff should be trained in data col ection and there should be asystem to ensure that data are accurately and routinely gathered.
� The government should ensure that medical personnel are trained to behave ina correct manner with patients and that any misconduct is penalized.
� The government should provide effective remedies to al victims, including accessto justice and the right to reparations, including restitution, rehabilitation,compensation, satisfaction and guarantees of non-repetition.
� The government should sign and ratify the Optional Protocol to the InternationalCovenant on Economic, Social and Cultural Rights, al owing the right of individualpetition.
� The government should encourage the National Human Rights Commission andother monitoring bodies to address violations of the right to health as part of their
CONCLUSION AND RECOMMENDATIONS
work and ensure that systems to submit information about violations are accessibleand wel publicized.
� The government should work closely with donors and international agencies tostrengthen its systems so that they are accountable, transparent and viable. Keypriorities include civil service reform, building the leadership and managementcapacity of the Ministry of Health at the central and district levels, assistance in puttingeffective drug procurement systems in place and, in the longer term, improved healthinformation systems.
� The government should work with al stakeholders including civil society, nationaland international NGOs and traditional leaders to carry out a countrywide mediacampaign to raise awareness of the importance of family planning, prevention ofcomplications, the need for institutional deliveries, timely interventions, and the rightto health.
6. IN LINE WITH INTERNATIONAL DEVELOPMENT COMMITMENTS, DONORS
� Support the government of Burkina Faso, with adequate long-term andpredictable technical and financial assistance, in its efforts to ensure the removal offinancial barriers to maternal health care and the availability and accessibility ofreproductive health services, including emergency obstetric care, for all womenthroughout the country.
� Continue to support the government of Burkina Faso to ensure the availabilityand accessibility of sexual and reproductive health care for al , including adolescents.
� Work with the government of Burkina Faso to ensure an outcomes-basedevaluation of the PNDS which identifies and addresses the continuing barriers facedby women and girls in access to sexual and reproductive health care, includingemergency obstetric care.
� Support efforts to improve the training, recruitment, retention and workingconditions of health staff, particularly in rural areas.
� Provide international co-operation and assistance to the government of BurkinaFaso to help fulfil the right to the highest attainable standard of health in the country,through strengthening the health system and ensuring the prioritization of access toessential health care for the most marginalized and vulnerable.
� Ensure that technical assistance is directed, among other priorities, to improvingdata col ection in the health system, including through maternal death audits, in orderto inform sexual and reproductive health planning, policy and practice.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
6 The figure of 484 per 100,000 live birthswas used as the reference by the authoritiesduring meetings with Amnesty Internationalin 2008 and 2009. However, in an officialdocument published in June 2009, thefigure of 307.3 was given, but it is basedon the 2006 RGPH, which uses a differentmethod than the DHS. See Ministry of
1 "Une femme enceinte a un pied dans la
Health, Annuaire statistique Santé 2008,
tombe et un pied sur la terre".
June 2009, p3.
2 A document published in 2007 by the
7 Ministry of Health, Tableau de bord Santé
Burkina Faso Ministry of Health states that
(Health reporting schedule) 2008, June
"approximately 2,783 women die every year
through wanting to give birth, that is 232maternal deaths a month or 58 maternal
8 Traditional birth attendants are medical y
deaths a week or another 8 maternal deaths
untrained women who assist pregnant
a day." See Ministry of Health, Projet
women giving birth in the community.
d'expérimentation de l'utilisation de
9 Mooré is the language of the Mossi people,
prestataires communautaires dans la lutte
the largest ethnic group in Burkina Faso.
contre la mortalité maternel e et néonataleau Burkina Faso, November 2007, p1.
10 For the research that identified the three
According to the 2006 General Population
delays, see notably Sereen Thaddeus and
and Housing Census (RGPH, Recensement
Deborah Maine, "Too far to walk: Maternal
général de la population et de l'habitat) the
mortality in context", Social Science &
population of Burkina Faso was 14,017,262,
Medicine, April 1994, Volume 38(8),
and women formed 51.7 per cent of the
11 Burkina Faso is ranked 177 out of
3 The WHO defines maternal mortality as
182 countries in the UNDP 2009 Human
the "death of a woman while pregnant or
Development Report, available at
within 42 days of termination of pregnancy,
irrespective of the duration and site of
heets/cty_ds_BFA.html (last accessed 5
the pregnancy, from any cause related to
November 2009).
or aggravated by the pregnancy or its
12 See UNDP 2009 Human Development
management but not from accidental
or incidental causes." See the WHOInternational statistical classification of
13 Human Rights Council, National Report:
diseases and related health problems,
Burkina Faso, 21 August 2008, para 95,
10th Revision, Volume 2, 2nd edition, 2004,
A/HRC/WG.6/3/BFA/1, available at
p98, available at http://www.who.int/
pdf (last accessed 5 November 2009).
kinaFaso_E.pdf (last accessed 5 November2009).
4 The maternal mortality ratio calculates thenumber of women who die as a result of
14 The Demographic and Health Survey
pregnancy and childbirth per 100,000 live
for the year 2003 indicates that only 0.8
births. See the International Planned
per cent of deliveries were carried out in
Parenthood Federation website, available at
the private sector. See DHS 2003, p123.
15 The Ministry of Economy and Development
m?g=M (last accessed 5 November 2009).
in partnership with the National Institute of
5 Ministry of Health, Annuaire statistique
Statistics and Demography publishes every
Santé (Health statistical yearbook) 2005,
five years a DHS. This document, which is
June 2006, p8. These figures are based on
supported by USAID, UNICEF, UNFPA and
Demographic and Health Surveys
the World Bank, is considered the most
(hereafter DHS).
reliable source of statistics. The most recent
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
DHS dates from 2003. Amnesty International
African countries", The Lancet, 3 June
was told that the results of a survey conducted
2006, Volume 367(9525), pp1835-1841.
in 2008 should be published "soon."
25 This article states that the marriage age
16 The Ministry of Health annual y
can be reduced for a "serious reason"
publishes an Annuaire statistique Santé
(pour motif grave) by a civil court.
(Health statistical yearbook) as wel as aTableau de bord Santé (Health reporting
26 CEDAW Committee, Concluding
schedule), the most recent of which,
Comments: Burkina Faso, 22 July 2005,
covering 2008, were published in June
2009. In addition a Carte sanitaire
27 Joel e Palmieri, "Burkina: intensifier la
(Health Map) was published in 2007.
lutte contre les mariages précoces", 5 March
17 UN figures are mostly based on national
2009, available at http://genre.francophonie.
statistics but use different methods of
org/spip.php?article519 (last accessed 5
evaluation, including weighting.
November 2009).
18 Customary law consists of traditional and
28 DHS 2003, p48.
unwritten rules that regulate issues such as
29 For a link between early pregnancies and
marriage, inheritance, divorce, and property.
the risk of fistula, see for example UNFPA,
19 CEDAW Committee, Combined fourth
Needs Assessment Report: Findings from
and fifth periodic reports of States parties:
Nine African Countries, 2003, available at
Burkina Faso, 9 February 2004, p29,
CEDAW/C/BFA/4-5, available at
(last accessed 5 November 2009).
30 CEDAW Committee, Combined fourth
(last accessed 5 November 2009).
and fifth periodic reports of States parties:
20 CEDAW Committee, Concluding
Burkina Faso, 9 February 2004, p44.
Comments: Burkina Faso, 22 July 2005,
31 Article 1 of the Constitution of Burkina
para 27, CEDAW/C/BFA/CO/4-5, available at
Faso prohibits discrimination on several
grounds including ethnicity, geographic
location and gender.
pdf (last accessed 5 November 2009).
32 Béatrice Nikièma, Slim Haddad,
21 National Institute of Statistics and
Louise Potvin, "Women bargaining to seek
Demography, Annuaire statistique
health care: norms, domestic practices,
(Statistical yearbook) 2008, April 2009, p57.
and implications in rural Burkina Faso",
22 DHS 2003, p48.
World Development, April 2008, Volume36(4), p615.
23 The DHS 2003 states that "the practiceof excision is very widespread in Burkina
33 Béatrice Nikièma, Slim Haddad,
Faso as 77 per cent of the women report
Louise Potvin, "Women bargaining to seek
having undergone this practice." This study
health care: norms, domestic practices,
also indicates that 65 per cent of girls aged
and implications in rural Burkina Faso",
between 15 and 19 had been excised and
World Development, April 2008, Volume
that the proportion of women who have
36(4), p615.
undergone this form of female genital
34 Association Songui Manégré / Aide au
mutilation is very similar in rural and urban
Développement Endogène (Songui Manégré
areas (77 and 75 per cent respectively).
Association / Aid to Endogenous
See DHS 2003, pp204-205.
24 WHO study group on female genital
35 Ministry of Health, Plan d'accélération
mutilation and obstetric outcome, "Female
de la réduction de la mortalité maternel e
genital mutilation and obstetric outcome:
et néonatale au Burkina Faso (Feuil e de
WHO col aborative prospective study in six
route), October 2006, p9, available at
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
statistique Santé 2008, June 2009, p4.
For al the other figures in the table, see
(last accessed 5 November 2009).
Ministry of Health, Comptes nationaux dela santé de la reproduction Burkina Faso
36 The eight Mil ennium Development Goals
2005-2006 (National Accounts of
(MDGs) – which range from halving extreme
Reproductive Health), June 2008, pp25-26.
poverty to halting the spread of HIV andproviding universal primary education, al by
42 The budget for reproductive health
the target date of 2015 – form a blueprint
includes health care (deliveries, prenatal
agreed to by al the world's countries and al
visits, counsel ing, infertility treatment,
the world's leading development institutions.
medical analysis.), drugs, salaries andtraining of health personnel, equipment,
37 This number corresponds to a 75 per cent
construction of health centres and medical
reduction from the 1993 maternal mortality
research. See Ministry of Health, Comptes
ratio of 566 deaths per 100 000 live births.
nationaux de la santé de la reproduction
In 2004, the government of Burkina Faso
Burkina Faso 2005-2006, June 2008,
recognized that "if the efforts are continued,
the rate of decline compared to 1998 couldhit the 50 per cent mark in 2015 (283
43 Ministry of Health, Tableau de bord Santé
deaths per 100,000 live births) and draw
2008, June 2009, p54.
closer to the mil ennium development goalset for Burkina Faso, which is 142 deaths
44 During a summit in Abuja (Nigeria) in
per 100,000 live births." See Burkina Faso:
April 2001, African Heads of State pledged
Poverty Reduction Strategy Paper,
"to set a target of al ocating at least 15 per
July 2004, p39, available at
cent of [their] annual budget to the
improvement of the health sector." See the
Abuja Declaration on HIV/AIDS, tuberculosis
(last accessed 5 November 2009).
and other related infectious diseases, para26, available at
38 See Burkina Faso and UNDP, Rapport
pays: Suivi des objectifs du mil énaire pour le
ion.pdf (last accessed 5 November 2009).
développement, December 2003, p21,available at
45 Ministry of Health, Politique sanitaire
nationale, available at
accessed 5 November 2009). The UNDP
considers that the national goal of 209
pdf (last accessed 5 November 2009).
deaths per 100,000 live births wil probably
46 Ministry of Health, Plan national de
be met, but that the maternal mortality ratio
développement sanitaire (2001-2010), p5.
wil stay above the goal of 142 deaths set bythe international community. See UNDP
47 Ministry of Health, Plan national de
website, available at
développement sanitaire (2001-2010),
pp30, 37-38 and 48-49.
accessed 5 November 2009).
48 Ministry of Health, Plan de mise en œuvre
39 Ministry of Health, Plan national de
de la stratégie nationale de subventions des
développement sanitaire (2001-2010), p19,
accouchements et des soins obstétricaux et
néonatals d'urgence au Burkina Faso, April
49 In the late 1990s, the World Bank and
2001_2010.pdf (last accessed 5 November
the International Monetary Fund fostered the
adoption of Poverty Reduction Strategies by
40 Ministry of Health, Annuaire statistique
many countries in the South. The elaboration
Santé 2008, June 2009, p4.
of these strategies was clearly spelt out as a"precondition" for "access to debt relief and
41 For the figure concerning the health
concessional financing from both institutions."
budget, see Ministry of Health, Annuaire
See World Bank website, available at
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
birth attendant's role), December 2007, pp2
,,contentMDK:22283891 pagePK:210058 piPK:210062 theSitePK:384201,00.html
58 Certificat d'études primaires élémentaires
(last accessed 5 November 2009).
50 Ministry of Health, Tableau de bord Santé
59 For details of this training, see School
2005, November 2006, p27, and Annuaire
of Public Health, Programme de formation
statistique Santé 2008, June 2009, pVII.
des agents de première ligne (Training
Prioritizing primary health care in this way
programme for front-line agents),
was in line with the 1978 Alma-Ata
February 1999.
Declaration which underlined for the first
60 Cal ed "eutociques".
time the importance of primary health careon an international level and was accepted
61 Ministry of Health, Guide pour la mise
by the member states of the WHO as vital
en place et le fonctionnement de cel ules
to achieve the objective of "health for
de gestion des urgences obstétricales et
néonatales au niveau vil age (Guide for theimplementation and the functioning of
51 Ministry of Health, Annuaire statistique
management units of obstetric and neonatal
Santé 2005, June 2006, p8 and Annuaire
emergencies at the vil age level),
statistique Santé 2008, June 2009, p28.
December 2007, p8.
52 Centrale d'Achats des Médicaments
62 Ministry of Health, Tableau de bord Santé
Essentiels Génériques et des Consommables
2007, June 2008, p50, and Annuaire
Médicaux (CAMEG, Purchasing centre for
statistique Santé 2008, June 2009, p2.
essential generic drugs and medical goods).
63 For example, in 2007, 68.33 per cent
53 For al the figures regarding the number of
of al deliveries in the Central Region were
health centres in Burkina Faso, see Ministry
medical y assisted, while only 25.64 per
of Health, Annuaire statistique Santé 2008,
cent were medical y assisted in the northern
June 2009, pp24-25.
Sahel Region. See Ministry of Health,
54 The CHU Yalgado in Ouagadougou and
Annuaire statistique Santé 2007, June 2008,
the CHU of Bobo-Dioulasso.
55 Comités de Gestion des Services de santé
64 CESCR, General Comment 14, para 12,
56 In the 1995 Decree governing the
(last accessed 5 November 2009).
functioning of the COGES, there are noprovisions for the active participation of
65 Human Rights Committee, General
women. During a mission in November
Comment 6, para 5. General Comments of
2009, Amnesty International learned that a
the Human Rights Committee are available
new text on the COGES is being elaborated
and experts have proposed that it provides
that each committee should have at least
(last accessed 5 November 2009).
one woman member. In written
66 Human Rights Committee, General
correspondence of the same month, an
Comment 28, para 10.
official of the Ministry of Health stated that itis difficult to evaluate women's participation
67 Human Rights Committee, Concluding
as it varies from one COGES to another, but
Observations: Mali, 16 April 2003, para 14,
on average there are two women out of six
CCPR/CO/77/MLI, available at
elected members.
57 Ministry of Health, Guide d'orientation
(last accessed 5 November 2009).
pour la mise en œuvre du nouveau rôle desaccoucheuses vil ageoises (Orientation guide
68 CEDAW Committee, General
for the implementation of the new traditional
Recommendation 24, para 2. CEDAW
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Committee's recommendations are available
and abortions.
83 An unwanted pregnancy is a pregnancy
(last accessed 5 November 2009).
that the pregnant woman or girl decides, ofher own free wil , is undesired.
69 Article 25 of the UDHR provides that"motherhood and childhood are entitled to
84 CEDAW, Article 16(1)(e).
special care and assistance." See also
85 CEDAW Committee, General
ICESCR, Article 12, which defines the right
Recommendation 24, para 31(c).
to health, and CEDAW, Article 12(2).
86 Loi n° 049-2005/AN portant santé de la
70 CESCR, General Comment 14, para 21.
reproduction (Law on Reproductive Health),
71 African Commission on Human and
available at http://www.legiburkina.bf/jo/
Peoples' Rights, Resolution 135 on maternal
mortality in Africa, 24 November 2008,
(last accessed 5 November 2009).
available at http://www.achpr.org/english/
87 See Décret n° 2009-676/PRES/PM/MS
portant conditions de création et d'ouverture
(last accessed 5 November 2009).
d'une structure privée de santé de la
72 CEDAW, Preamble.
reproduction (Decree on the creation andopening of a private reproductive health
73 CEDAW, Article 12(1).
structure) and Décret n° 2009-720/PRES/PM/MS/MEF portant sur les conditions de
74 CEDAW, Article 14(2)(b).
fabrication et d'importation
75 ACHPR, Article 18(3).
des produits contraceptifs au Burkina Faso(Decree on the production and import of
76 CRC, Article 24(1).
contraceptive products in Burkina Faso),
77 ICESCR, Article 12.
October 2009.
78 CRC, Article 2.
88 CEDAW Committee, ConcludingComments: Burkina Faso, 22 July 2005,
79 See WHO, "Gender and Human Rights:
Sexual Health", available athttp://www.who.int/reproductivehealth/topics/
89 Ministry of Health, Plan stratégique de
sécurisation des produits contraceptifs
(last accessed 5 November 2009).
(2006-2015), p16.
80 Ministry of Health, Plan stratégique de
90 Ministry of Health, Plan stratégique de
sécurisation des produits de la santé de la
sécurisation des produits de la santé de la
reproduction 2009-2015 (Reproductive
reproduction (2009-2015), p17.
Health Products Security Strategic Plan),
91 Information provided to Amnesty
January 2009, p28.
International by an official of the Ministry
81 An unintended pregnancy is a pregnancy
that is identified by the mother as either
92 DHS 2003, p69.
unwanted or mistimed (occurring earlierthan wanted) at the time of conception.
93 See Contraceptive prevalence rate byUN Data, based on the UNICEF's State of
82 See Nils Daulaire et al., Promises to Keep:
the World's Children 2009, available at
The Tol of Unintended Pregnancies on
Women's Lives in the Developing World,
D%3A34 (last accessed 5 November 2009).
Global Health Council, 2002, p42, availableat http://www.globalhealth.org/assets/
94 CEDAW Committee, Combined fourth
and fifth periodic reports of States parties:
(last accessed 5 November 2009).
Burkina Faso, 9 February 2004, p38.
In this study, the expression "unintended
95 DHS 2003, pp64 and 65.
pregnancies" comprises unintended births
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
96 DHS 2003, p73.
106 Injectable contraceptives areadministered by a deep intramuscular
97 The DHS 2003 states that while only
injection into the muscle of the arm or
11 per cent of women with no formal
buttock. They maintain a sufficient level of
education use contraception (6 per cent
hormone to ensure contraception for one to
modern methods and 5 per cent traditional
three months, depending on the type.
methods), among women with primary schooleducation, these proportions are 19 per cent
107 A contraceptive implant is a smal tube
(13 per cent modern methods and 5 per
placed below the skin under local
cent traditional methods) and for the most
anaesthetic. Each implant lasts three or five
educated woman 52 per cent (43 per cent
modern methods and 9 per cent traditionalmethods). See DHS 2003, p74.
108 According to official figures, the mostwidespread modern methods used in
98 Loi n° 049-2005/AN portant santé de la
Burkina Faso are injectable contraceptives
reproduction (Article 9).
(56.86 per cent), the pil (28.25 per cent),implants (7.27 per cent) and condoms (5.74
99 Article 11 of the Law on Reproductive
per cent). See Ministry of Health, Annuaire
Health stresses that, "al individuals,
statistique Santé 2008, June 2009, p52.
including adolescents and children, andal couples have the right to information,
109 Ministry of Health, Plan stratégique de
to education, concerning the advantages,
sécurisation des produits contraceptifs
the risks, and the efficiency of al methods
(2006-2015), p14.
of birth regulation."
110 Ministry of Health, Plan stratégique de
100 Ministry of Health, Plan stratégique de
sécurisation des produits de la santé de la
sécurisation des produits contraceptifs
reproduction (2009-2015), p29.
(2006-2015), p18.
111 Discussions with an official from UNFPA,
101 CEDAW Committee, Concluding
Comments: Burkina Faso, 22 July 2005,para 36.
112 United Nations Population Division,Department of Economic and Social Affairs,
102 Commission on Human Rights, Report
Abortion Policies: A Global Review, 2002,
of the Special Rapporteur on the right of
p76, available at
everyone to the enjoyment of the highest
attainable standard of physical and mental
s/abortion/profiles.htm (last accessed 5
health, 16 February 2004, para 28,
November 2009).
113 Ministry of Health, Tableau de bord
Santé 2008, June 2009, p23.
/$FILE/G0410933.pdf (last accessed 5
114 According to a 2002 UN document,
November 2009).
"[the government's] primary motivation
103 Ministry of Health, Plan stratégique de
was a concern for maternal health."
sécurisation des produits de la santé de la
See United Nations Population Division,
reproduction (2009-2015), p29.
Department of Economic and Social Affairs,Abortion Policies: A Global Review, 2002,
104 In al , 850 health providers in 13 regions
and 54 private professionals in familyplanning were trained. See Ministry of
115 The limitations of this law were stressed
Health, Plan stratégique de sécurisation des
by international NGOs in a submission to the
produits de la santé de la reproduction
Human Rights Council before the 2008
Universal Periodic Review of Burkina Faso.
They stated that the legal prohibition of non-
105 Ministry of Health, Plan stratégique de
therapeutic abortions "increases the rate of
sécurisation des produits de la santé de la
il egal abortion. In fact economic difficulties,
reproduction (2009-2015), p36.
in early pregnancy and especial y parents'
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
hostility in the face of pregnancy before
CEDAW Committee, General
marriage, plus the fact that sexuality is so
Recommendation 24, para 31(b).
often seen as taboo, are al factors thatencourage il egal abortion." See Human
126 CEDAW Committee, General
Rights Council Working Group on the
Recommendation 24, para 21.
Universal Periodic Review, 15 September
127 CESCR, General Comment 14, para 43.
2008, para 32, A/HRC/WG.6/3/BFA/3,available at
128 A study of the quality of care carried
out in a district hospital in Ouagadougou
underlines the importance of being
f (last accessed 5 November 2009).
accompanied. "The women who comealone, without someone to accompany them,
116 Commission on Human Rights, Report
have been qualified as ‘delinquents' or as
of the Special Rapporteur on the right of
‘social y disadvantaged persons' … To be
everyone to the enjoyment of the highest
alone a priori credibly means that one has no
attainable standard of physical and mental
money (it is the accompanying person who
health, 16 February 2004, paras 24-25.
pays the material and the prescriptions, and
117 Commission on Human Rights, Report
thus a solution has to be found for the
of the Special Rapporteur on the right of
deprived woman); it also means that there is
everyone to the enjoyment of the highest
a certain number of tasks normal y devolved
attainable standard of physical and mental
to the accompanying person which have to
health, 16 February 2004, para 30.
be ‘handled': wash the soiled linen, deal withthe placenta, feed the pregnant woman,
118 See International Planned Parenthood
etc." See Charlemagne Ouédraogo, David
Federation's website, "West African health
Bazié, Marc-Eric Gruénais, Fatoumata
ministers cal for passage of abortion laws",
Ouattara, Dominique Pobel, Cyril Wissocq,
Dominique Dubourg, Vincent De Brouwere,
Fabienne Richard, Programme d'amélioration
de la qualité et de l'accès aux soins
accessed 5 November 2009).
obstétricaux d'urgence dans les pays endéveloppement, Analyse situationnel e
119 Ministry of Health, Annuaire statistique
Secteur 30 Ouagadougou, p66.
Santé 2007, June 2008, pp19-20.
129 The Bamako Initiative was adopted in
120 In some of these remote regions,
1987 by Health Ministers of the WHO
populations are very dispersed and live in
African Region. According to an expert of the
desert areas.
issue of equity and user-fees in West Africa:
121 The health districts without a district or
"the [Bamako] initiative differs from the
regional hospital are: Mangodara (Cascades
national policy of user fees, whose main
region); Bittou, Garango and Pouytenga
objective is to generate income, in that its
(Centre East region); Réo and Sapouy
introduction should improve the quality of
(Centre West region); Manni and Gayéri
service and ensure equity in access to care.
(Eastern region); Kvigué and Léna (Hauts
A stock of essential generic drugs is provided
Bassins region); Gourcy (Northern region).
by donors to the dispensary management
See Ministry of Health, Annuaire statistique
committee (composed of representatives
Santé 2008, June 2009, pp24-25.
of the population). The drugs must thenbe sold to users at a profit. This profit, in
122 The rainy season in Burkina Faso starts
addition to payments by users for
in June and ends in October.
consultations (direct payment = user fees),
123 This figure was given to Amnesty
serves to buy back the initial stock of drugs,
International by the nurse in charge of this
and to improve access to care and quality of
service (staff incentives, building repairs,etc)." See Valéry Ridde, "Fees-for-services,
124 CEDAW, Article 14(2)(b).
cost recovery, and equity in a district of
Burkina Faso operating the Bamako
CESCR, General Comment 14, para 21;
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
Initiative", Bul etin of the World Health
caesarean sections, but an expert told
Organization, 2003, Volume 81(7), p532.
Amnesty International in August 2009 that"in reality, the contents of these kits vary
130 The government has withdrawn fees
significantly from one region to another
for people suffering from tuberculosis or
which causes real problems."
leprosy (1984), or HIV/AIDS (1991) as welas preventive care for vulnerable groups
136 Amnesty International was given this
(consultations for pregnant and
information by patients and members of
breastfeeding women) and for patients with
their families from both urban and rural
meningitis (2002) and for victims of severe
areas. This information emerged in individual
malaria (2005).
interviews, and also in focus groupdiscussions.
131 A circular from the Secretary Generalof Health in February 2002 asked health
137 A near-miss in this context refers to a
centres to make certain preventive
woman who came close to maternal death,
treatments free of charge, including
but did not die.
medicines against anaemia (iron) andmalaria (chloroquine). In March 2003,
138 Valéry Ridde, Abel Bicaba, Revue
prenatal visits were made free for al
des politiques d'exemption/subvention du
pregnant women.
paiement au Burkina Faso. La stratégiede subvention des soins obstétricaux et
132 In 2004, World Bank representatives
néonataux d'urgence, 16 January 2009,
participated with the government when
the terms of reference of this policy wereelaborated. Later, they took part in sessions
139 There is a system for acquiring a
in which the strategy was devised.
"certificate of indigence" from the Ministry of
To Amnesty International's knowledge,
Social Action, but people have to ask for it at
the decision to set the rate of subsidy at 80
district offices, which means that most of the
per cent was taken by the government of
rural population do not have access to them.
Burkina Faso; the World Bank played no
According to an expert on the health system
role in the discussions and decision.
in Burkina Faso, "these certificates are beinggiven in dribs and drabs by officials of the
133 This budget was calculated taking into
Ministry of Social Action who are only
account the estimated number and cost of
present in towns and who use criteria which
medical interventions. See Ministry of
are not uniform throughout the country."
Health, Stratégie nationale de subventiondes accouchements et des soins
140 Vil age selection committees made lists
obstétricaux et néonataux d'urgence au
of people considered to be indigent, using
Burkina Faso, 2006. For a detailed analysis
their knowledge of the population combined
of the origin and application of this subsidy
sometimes with field visits to households.
strategy, see the study financed by UNICEF
The list was validated by the chief of the
and co-ordinated by the Institute of Tropical
vil age, the mayor, and final y by the COGES
Medicine at Antwerp, Valéry Ridde, Abel
which had the final word. The COGES only
Bicaba, Revue des politiques
validated 47.53 per cent of those selected.
d'exemption/subvention du paiement au
Half those identified as indigent were
Burkina Faso. La stratégie de subvention des
women. See Valery Ridde, Maurice Yaogo,
soins obstétricaux et néonataux d'urgence,
Yamba Kafando, Omarou Sanfo, Norbert
16 January 2009.
Coulibaly, Abdouaye Nitiema, Abel Bicaba,"A community-based targeting approach to
134 The subsidy is only 60 per cent when
exempt the worst-off from user fees in
pregnant women go directly to referral
Burkina Faso", J. Epidemiol Community
centres instead of going first to the CSPS.
Health, 19 August 2009.
This is intended to deter bottlenecks at thereferral levels.
141 Valéry Ridde, Abel Bicaba, Revue despolitiques d'exemption/subvention du
135 There is an official list of what should be
paiement au Burkina Faso. La stratégie de
included in kits for normal deliveries and for
subvention des soins obstétricaux et
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
néonataux d'urgence, 16 January 2009,
advantage over the rest of the population".
For a discussion about user fees indeveloping countries, see David de Ferranti,
142 The DHS 2003 states that 46.4 per cent
Paying for health services in developing
of the population lives below the poverty line.
countries: a cal for realism, World Health
143 Several women at a focus group in
Forum, 1985, Volume 6.
Ouagadougou in March 2009 also told
149 In 2006 in Niger, the German NGO
Amnesty International that taxi drivers
HELP, financed by ECHO, tested the total
demand higher fares than normal when
exemption of payment for children under the
pregnant women need to reach a health
age of five and pregnant and breastfeeding
facility fast. One woman said: "some taxi
women in two districts. The Niger
drivers have no pity for us, when they see
government then decided to make it a
that we are about to deliver, they take
national policy, and it was extended to cover
advantage of the situation and ask for higher
the whole territory in 2007. See Valery Ridde,
Aissa Diarra, A process evaluation of user
144 Boubacar Kaboré, Etude des
fees abolition for pregnant women and
déterminants de la corruption passive, 2005,
children under five years in two districts in
Niger (West Africa), BioMed Central Health
Services Research, 3 June 2009, available at
passive-chr-ddg.html (last accessed 5
November 2009).
accessed 5 November 2009).
145 REN-LAC, État de la corruption au
150 For example, a study in Nigeria revealed
Burkina Faso (State of corruption in Burkina
that "the number of deliveries at a main
Faso), 2006 Report, December 2007, p29.
regional hospital plummeted by 46 per centfol owing the introduction of user fees."
146 Certain African countries such as
See Centre for Reproductive Rights and
Uganda and South Africa have adopted
Federation of Women's Lawyers, Failure to
policies to end user fees. See Valery Ridde,
Deliver: Violations of Women's Human Rights
Florence Morestin, Une recension des écrits
in Kenyan Health Facilities, 2007, p51,
scientifiques sur l'abolition des frais aux
usagers dans les services de santé en
Afrique, January 2009, available at
%20to%20deliver.pdf. See also Overseas
Development Institute, Alternative Social
Health Protection in West and Central Africa:
accessed 5 November 2009).
Achieving Equitable Access to Health Care
147 Ministry of Health, Rapport de synthèse
and Reducing Child and Maternal Mortality;
de la rencontre du Comité national de suivi
Save the Children, An Unnecessary Evil?
des programmes et stratégies de réduction
User Fees for Health Care in Low-income
de la mortalité maternel e et néonatale
Countries, 2005, available at
(Report of the meeting with the National
Committee fol owing up the programmes and
An_Unnecessary_Evil.pdf; and Save the
strategies to reduce maternal and neonatal
Children, Freeing up Health Care: A Guide
death), 1 June 2007, p3.
To Removing User Fees, 2008, available athttp://www.savethechildren.org.uk/en/docs/F
148 It seems that the refusal to provide free
reeing_up_Healthcare.pdf (last accessed 5
contraceptive products derives from this
November 2009).
same idea. A representative of UNFPA toldAmnesty International in June 2009 that "the
151 WHO, World Health Report 2005, p140,
cost of contraceptive products creates a
available at http://www.who.int/whr/2005/
barrier for the poorest women, but the
government has made the choice not to offer
(last accessed 5 November 2009).
free contraception in order not to give them
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
152 Save the Children, Paying With Their
159 UN General Assembly, Report of the
Lives: The Cost of Il ness for Children in
Special Rapporteur on the highest attainable
Africa, 2006, available at
standard of physical and mental health,
13 September 2006, para 17(b), A/61/338,
paying_with_their_lives.pdf (last accessed
available at http://www.atmindex.org/
5 November 2009). See also Centre for
download/10 (last accessed 5 November
Reproductive Rights and Federation of
Women's Lawyers, Failure to Deliver:Violations of Women's Human Rights in
160 Ministry of Health, Plan national de
Kenyan Health Facilities, 2007, p54.
développement sanitaire (2001-2010), p32.
153 Global Campaign for the Health
161 An obstetrician working in Ouagadougou
Mil ennium Development Goals 2009,
told Amnesty International in June 2009 that
Leading by Example – Protecting the most
one of the district hospitals "does not have
vulnerable during the economic crisis, p53,
an electricity generator as a back-up in the
available at http://www.ausaid.gov.au/
eventuality of a power cut during operations
in the surgical unit".
(last accessed 5 November 2009).
162 Décret n° 2000-449/PRES/PM/MS du
154 See International Health Partnership,
6 octobre 2000 portant création du Centre
"Leaders commit new finance to tackle
National de Transfusion Sanguine (Decree
women's and children's health in the
on the creation of the National Blood
developing world", available at
Transfusion Centre). Its missions include
"the supply to al health facilities in the
/en/taskforce (last accessed 5 November
country of blood products for which it
guarantees the sampling, treatment …conditioning and distribution" as wel as
155 According to the WHO, "By and large,
"the guarantee of transfusion safety."
the introduction of user fees is not a viableanswer to the underfunding of the health
163 WHO, Aide-Mémoire for National
sector: it institutionalizes exclusion of the
Blood Programmes, 2002, available at
poor and does not accelerate progress
towards universal access and financial
coverage. Nevertheless, abolishing user fees
accessed 5 November 2009).
where they already exist is not a panacea:
164 Meeting with an official in charge of the
it needs to be accompanied, from the very
system of blood transfusion on a national
day they are brought to an end, by structural
level in June 2009.
changes and a refinancing of the healthservices… Without other necessary
165 Meeting with an official in charge of the
structural reforms – increased 24-hour
system of blood transfusion on a national
availability of services, improved resourcing
level in June 2009.
and referral, enhanced technical capacity,
166 Ministry of Health, Tableau de bord
and changed attitudes to patients – gains
Santé 2008, June 2009, p50.
made by removing financial barriers alonemay not be adequate." See WHO, World
167 Ministry of Health, Tableau de bord
Health Report 2005, p139. See also Save
Santé 2008, June 2009, p6.
the Children, Freeing up Health Care:
168 Ministry of Health, Annuaire statistique
A Guide To Removing User Fees, 2008.
Santé 2007, June 2008, pp27-29.
156 CESCR, General Comment 14, para
169 Ministry of Health, Carte sanitaire 2007,
157 CEDAW Committee, General
170 UN General Assembly, Report of the
Recommendation 24, para 21.
Special Rapporteur on the highest attainable
158 CEDAW Committee, General
standard of physical and mental health,
Recommendation 24, para 27.
13 September 2006, para 17(a).
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
171 WHO, International Confederation of
176 Amnesty International learned that quite
Midwives (ICM) and the International
often pregnant women who die during their
Federation of Gynaecology and Obstetrics
transfer are not counted as maternal deaths
(FIGO), Making pregnancy safer: the critical
as both the medical team who referred the
role of the skil ed attendant, 2004, p1,
woman and the one that received the body
refuse to be held accountable for the death.
The statistics on maternal mortality are
9241591692.pdf (last accessed 5 November
therefore significantly lower than the reality.
177 For example, an obstetrician in
172 In Burkina Faso, midwives have a higher
Ouagadougou told Amnesty International in
level of entry requirement than auxiliary
June 2009 that since one of the district
midwives. Trainee midwives need a school
hospitals in the capital did not have an
leaving diploma plus a final year certificate.
electricity generator which could guarantee a
Auxiliary midwives need a basic school
continued power supply, "the people in
leaving qualification. Midwives' training takes
charge of the maternity ward do not want to
three years, while auxiliary midwives' training
take needless risks with their patients. They
only takes two years, and midwives study
prefer simply to transfer them to other
more theory and more courses on normal
facilities." Fol owing the September 2009
deliveries and complications. For example,
floods, several services of the Yalgado
midwives have 30 hours' training on
university hospital have been transferred to
emergency obstetric care, while auxiliary
other facilities in Ouagadougou, making the
midwives only have 15. For details, see
situation even more critical.
Charlemagne Ouédraogo, David Bazié,Marc-Eric Gruénais, Fatoumata Ouattara,
178 CESCR, General Comment 14, para 12.
Dominique Pobel, Cyril Wissocq, Dominique
179 This Programme has set up a new
Dubourg, Vincent De Brouwere, Fabienne
category of midwives cal ed Attaché(e)s
Richard, Programme d'amélioration de la
Soins Santé en Obstétrique et Gynécologie
qualité et de l'accès aux soins obstétricaux
(ASSOG, Obstetric and Gynecological Health
d'urgence dans les pays en développement,
care attachés). The first recruitment exam
Analyse situationnel e Secteur 30
took place in 2009 and the training
programme lasts two years.
173 A partograph is a tool used to monitor al
180 Fatoumata Ouattara, Amélioration de la
stages of labour of a pregnant woman. It is
Qualité et l'Accès aux Soins Obstétricaux
essential to the woman's and infant's wel -
d'Urgence dans les pays en développement
being and al ows a timely response in case of
(AQUASOU), available at
a complication. WHO standards require that
al deliveries are monitored with a
accessed 5 November 2009).
partograph. See WHO, The Partograph,1988, available at
181 See Programme d'amélioration de la
qualité et de l'accès aux soins obstétricaux
1988/WHO_MCH_88.4.pdf (last accessed
d'urgence dans les pays en développement,
5 November 2009).
Composante 2 – Burkina Faso, Rapport finald'activités, 1er janvier 2003 au 31 mars
174 For detailed information about the
2006, p48, available at
curriculum of this training see the document
published by the School of Public
Health, Programme de formation des
%202006-09-05.pdf (last accessed
accoucheuses brevetées, July 2008.
5 November 2009).
175 WHO, International Confederation
182 Ministry of Health, Plan stratégique pour
of Midwives (ICM) and the International
une maternité à moindre risque 2004-2008
Federation of Gynaecology and Obstetrics
(Motherhood at Lesser Risk Strategy), March
(FIGO), Making pregnancy safer: the critical
2004, p13, available at
role of the skil ed attendant, 2004, pp1-2.
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
/dsf/plan-strategie-mmr.pdf (last accessed 5
193 See Fabienne Richard, H. Filali, Vincent
November 2009).
De Brouwere, "Les erreurs en médecine :Pourquoi et comment en parler?", Revue
183 This document highlighted the low
d'Epidémiologie et de Santé Publique, June
availability of maternal and neonatal care,
2005, Volume 53(3), pp315-335.
women's lack of access to maternal andneonatal care, the low level of community
194 CESCR, General Comment 14, para 59.
investment into maternal and prenatalhealth care and the lack of stakeholders'
195 Human Rights Council, Report of the
engagement at al levels. See Ministry of
Working Group on the Universal Periodic
Health, Plan d'accélération de la réduction
Review: Burkina Faso, 7 January 2009, para
de la mortalité maternel e et néonatale au
98, A/HRC/10/80, available at
Burkina Faso (Feuil e de route), October
ts/Session3/BF/A_HRC_10_80_BurkinaFaso_E.pdf (last accessed 5 November 2009).
184 Ministry of Health, Plan stratégique desécurisation des produits de la santé de la
196 At the regional level, Burkina Faso
reproduction (2009-2015), p36.
ratified the African Union Convention onPreventing and Combating Corruption in
185 Ministry of Health, Plan national de
November 2005. Article 12 of this
développement sanitaire (2001-2010), p38.
instrument requires state parties to "createan enabling environment that wil enable civil
186 Arrêté n° 2007-240/MS/CAB Portant
society and the media to hold governments
Charte de l'Utilisateur des Services de Santé
to the highest levels of transparency and
(Decree on the Charter of Heath Services'
accountability in the management of public
User), Article 5.
affairs." See the AU Convention on
187 At the regional level, the Federation of
Preventing and Combating Corruption,
Associations of midwives from Centre and
adopted in Maputo, 11 July 2003, available
West Africa (FASFACO, Fédération des
Associations de Sages-Femmes de l'Afrique
du Centre et de l'Ouest) adopted in 2005
the African Charter of the midwife.
%20Corruption.pdf (last accessed 5November 2009).
188 Ministry of Health, Plan national dedéveloppement sanitaire (2001-2010), p49.
197 Article 156 of the Penal Code definesactive corruption as the action by "any agent
189 Ordre des Médecins, Order of Doctors.
or employee of the Administration… who
190 Amnesty International learned that in
accepts offers or promises, who receives
one case, in 2008, administrative sanctions
donations or presents, to do an act of his or
were taken against medical personnel
her functions or profession, even legal, but
involved in the sales of medicines and
not subjected to salary."
vaccinations in a referral hospital and that
198 This new organ merged three bodies
judicial proceedings are under way.
whose mandate was to fight against
191 Ministry of Health, Guide pour les
corruption and fraud, the High Commission
audits de décès maternels, néonatals et
for the Coordination of Anti-Corruption
des échappées bel es (Guide for audits on
Activities (HACLC, Haute Autorité de
maternal and neonatal deaths and near-
Coordination de la Lutte Contre la Corruption),
misses), November 2008.
the State Inspector General, and the NationalCommission for the Fight Against Fraud.
192 WHO, Beyond the Numbers: Reviewingmaternal deaths and complications to make
199 See ASCE, Rapport général annuel
pregnancy safer, 2004, pp45-46, available at
d'activités 2008 de l'Autorité supérieure de
contrôle de l'État, p6, available at
9241591838.pdf (last accessed 5 November
ASCE_Rapport_2008.pdf (last accessed 5November 2009).
GIVING LIFE, RISKING DEATH – MATERNAL MORTALITY IN BURKINA FASO
200 REN-LAC, Etat de la corruption au
207 The Paris Declaration on Aid
Burkina Faso, 2006 Report, December
Effectiveness aims to improve the way that
aid is delivered and make it more effectiveat al eviating poverty. It set out a series of
201 UN Convention against Corruption,
targets to be met by both donors and
adopted by the General Assembly by
partner, by 2010, focused on five key
resolution 58/4 of 31 October 2003,
principles for improving aid delivery: country
available at http://www.unodc.org/
ownership, alignment to partner country
systems, harmonization and co-ordination of
donor efforts, managing for results and
(last accessed 5 November 2009).
mutual accountability for aid commitments.
202 See General Framework for the
Progress on the implementation of the Paris
Organization of Budget Support linked to the
Declaration was reviewed at the third High
Strategic Framework for the Fight Against
Level Forum on Aid Effectiveness in Accra,
Poverty (CGAB-CSLP), 2005.
Ghana, in September 2008. The AccraAgenda for Action, which was endorsed by
203 Ministry of Health, Comptes nationaux
ministers of developing and donor countries
de la santé de la reproduction Burkina Faso
and heads of multilateral and bilateral
2005-2006, June 2008, p19. This document
development institutions, affirmed a set of
indicates that for the year 2006, out of a total
further commitments to take action to
budget of 12 mil ion CFA francs (around
accelerate progress on improving aid
US$27,200), the three financial sources for
reproductive health were respectively 37.69per cent from international donors, 30.81
208 GAVI Al iance, Health System
per cent from the state and 28.9 per cent
Strengthening, May 2009, available at
from households.
204 Ministry of Health, Programme d'Appui
accessed 5 November 2009).
au Développement Sanitaire (PADS)2008-2012, p10.
205 The World Bank's contribution to thePADS takes the form of a Health SectorSupport and Multisectoral HIV/AIDS projectthat focuses mainly on the fight againstHIV/AIDS and malaria. This project is partlyproviding unearmarked funding throughPADS, partly earmarked funding for nutritionactivities in six regions as wel as supplies ofbed nets and drugs for malaria. Accordingto an official of the World Bank, this funding"wil give Burkina the necessary flexibility todetermine its priorities based on localdisease burden while ensuring that keyinterventions – including for malaria,maternal and child health, nutrition, andHIV/AIDS prevention and treatment – receivethe necessary financing." See World Bankpress release, 27 April 2006, available athttp://web.worldbank.org/WBSITE/EXTERNAL/NEWS/0,,contentMDK:20904900 pagePK:64257043 piPK:437376 theSitePK:4607,00.html (last accessed 5 November 2009).
206 Meeting with a GTZ official inOuagadougou, July 2008.
WHETHER IN A HIGH-PROFILE CONFLICT
OR A FORGOTTEN CORNER OF THE GLOBE,
AMNESTY INTERNATIONAL CAMPAIGNS
FOR JUSTICE AND FREEDOM FOR ALL AND
SEEKS TO GALVANIZE PUBLIC SUPPORT TO
BUILD A BETTER WORLD
Activists around the world have shown that it is possible to resist thedangerous forces that are undermining human rights. Be part of thismovement. Combat those who peddle fear and hate.
� Join Amnesty International and become part of a worldwide movementcampaigning for an end to human rights violations. Help us make a difference.
� Make a donation to support Amnesty International's work.
Together we can make our voices heard.
I am interested in receiving further information on becoming a memberof Amnesty International
I wish to make a donation to Amnesty International (donations wil betaken in UK£, US$ or €)
Please return this form to the Amnesty International office in your country.
For Amnesty International offices worldwide: www.amnesty.org/en/worldwide-sites
If there is not an Amnesty International office in your country,please return this form to: Amnesty International,International Secretariat, Peter Benenson House,1 Easton Street, London WC1X 0DW, United Kingdom
GIVING LIFE, RISKING DEATH
MATERNAL MORTALITY IN BURKINA FASO
More than 2,000 women die in Burkina Faso every year fromcomplications of pregnancy and childbirth. Most of these deaths
could be prevented.
Some women die because they cannot reach a health facility capable
of treating them, or because they arrive too late. Many lose their livesbecause their relatives cannot pay the fees demanded by medicalpersonnel. Others die because of shortages – of blood, drugs,
equipment or qualified medical staff. Maternal mortality takes itsmajor toll on the poorest and the least educated women and those
who live in rural areas, home to 80 per cent of the population.
The authorities in Burkina Faso have devoted effort and resources
to reducing maternal mortality, with the help of the donor community.
However, many pregnant women still cannot obtain the health care
they need in time, and pregnancy all too often ends in tragedy.
Amnesty International calls for better information and services for
family planning, for the government to remove financial barriers to
maternal health care and for improvements in access to care. To do
less is to violate the right to health of the women of Burkina Faso.
ISBN 978-0-86210-457-3
MATERNAL MORTALITY
170 x 244 mm
170 x 244 mm
Source: http://amnistia.pt/files/Relatoriosvarios/Mortalidade_Materna_no_Burkina_Faso.pdf
Practice Parameters for the Evaluationand Management of Constipation Charles A. Ternent, M.D., Amir L. Bastawrous, M.D., Nancy A. Morin, M.D.,C. Neal Ellis, M.D., Neil H. Hyman, M.D., W. Donald Buie, M.D., and The StandardsPractice Task Force of The American Society of Colon and Rectal Surgeons T he American Society of Colon and Rectal methods of care or exclusive of methods of care
Untitled Document Issue 5 15 November Table of Contents Explanation of the Barometer Welcome to the fifth edition of the Roadmap to Equality. This edition The Roadmap to Equality: Regional: Media launch of the 16 Days campaign comes at a very exciting time with Southern Africa Gender and Development Protocol Baro- Malawi signing and Zimbabwe








