Microsoft word - nsaid paper 2014.docx


Questioning the use of NSAIDs Given Inflammation is a Perfectly Healthy
Response Following Acute Musculoskeletal Injuries
Written by: Dr. Bahram Jam, PT
Advanced Physical Therapy Education Institute (APTEI), Thornhill, ON, Canada
July 14, 2014 Article published on "Clinical Library"
Nonsteroidal
anti-inflammatory
The use of prescription NSAIDs is reported
(NSAIDs) are often prescribed in the
to be the 15th most common cause of death in
treatment of musculoskeletal injuries and are
the United States and it is conservatively
calculated that in the last 3 decades 300,000
people in the United States have died from
medications worldwide. It
GI complications due to NSAIDs (Wolf et al
is estimated that more
than 30 million people
take NSAIDs daily for a variety of conditions
Before I begin my likely controversial
ranging from headaches to low back pain
discussion on the use of NSAIDs, it is
(LBP) (McGettigan & Henry 2013).
appropriate to clearly state that I am certainly
not making a blanket statement that all
Ibuprofen is the most commonly used
NSAIDs are inappropriate for all medical
NSAID in North America while diclofenac is
conditions. In fact, there are studies
the most popular throughout the world
supporting their benefit with respect to pain
(McGettigan & Henry 2013). Interestingly a
and functional improvements in various
2013 review recommended that due to its
conditions such as rheumatoid arthritis,
high cardiovascular toxicity, diclofenac be
osteoarthritis, ankylosing spondylitis, gout,
and tension headaches. These and
(McGettigan & Henry 2013). In fact it is well
many other conditions where
documented that all forms of NSAIDs are
NSAIDs may be appropriate to
use have one thing in common;
gastrointestinal (GI), renal, hepatic, and
cardiovascular effects (Hunt et al 2007).
inflammatory response to an acute soft tissue
injury following a specific trauma.
In 1998 The American Journal of Medicine
stated the following:
Admittedly, there are several high quality
studies supporting the use of various
"Conservative calculations estimate that
NSAIDs on patients post soft-tissue injuries
approximately
(although conflicting). There are systematic
hospitalized annually for NSAID-related GI
reviews supporting the use of NSAIDs for
complications and at least 16,500 NSAID-
back pain (Chung et al 2013, Griffin et al
related deaths occur each year among
2002) and many other soft tissue injuries
arthritis patients alone in the USA, 4,000
(Jones & Lamdin 2013). Then again the
deaths in Great Britain and 1,650 deaths in
Cochrane database concludes that there is
Germany. The figures of all NSAID users
insufficient and conflicting evidence to
would be overwhelming, yet the scope of this
support the use of NSAIDs in treating lateral
problem is generally under-appreciated."
elbow pain (Pattanittum et al 2013).
(Singh et al 1998)



Despite the evidence, my goal is to have
NSAIDs is in any way associated with the
clinicians continue to question and scrutinize
risk of recurrence.
the use of NSAIDs on soft-tissue injuries.
Sure you may think that "this Bahram Jam
The million dollar question remains, could
guy is being hypocritical; in one breath he
post-acute
promotes evidence-based practice and in
musculoskeletal injuries actually increase
another breath he is questioning clear
the risk of recurrence
medical evidence".
inadequate
I will reply with, sure there are studies
supporting the use of NSAIDs on soft-tissue
injuries and that is precisely why health care
remains unknown as the
providers support their use, however the
studies look at the short-term symptomatic
involving rats and rabbits,
recovery; what they fail to do is look at the
give conflicting results. However, in this
long-term effects and recurrence rates
biased paper I shall summarize a number of
with and without NSAIDs. At the expense of
studies concluding that NSAIDs significantly
faster recovery, what effects do NSAIDs
reduce the quality and strength of bones and
have on the actual quality of the bone,
soft-tissues during healing.
tendon, ligament or muscle repair?
Based on 65 clinical trials,
(Warden et al 2006) 60
rats received a controlled
clearly supports the use of
incision of their knee
NSAIDs for patients with
medial collateral ligament (MCL) simulating
non-specific LBP (Roelfs et
an acute grade II MCL sprain. After 2 weeks
al 2008), hence nearly every patient with
they demonstrated that compared to the
acute LBP almost instantaneously consumes
control group, the rats who received NSAIDs
either over the counter or prescription
(celecoxib) 5 days a week had significantly
NSAIDs in order to hasten their recovery.
delayed healing where the MCL could
absorb 33% less energy before tearing.
Following an acute episode of LBP, the
recurrence rate within 1-year is up to 72%
In a second study (Ferry et al 2007) 200 rats
(Klenerman et al 1995), and there has yet to
received a controlled incision on their
be study investigating if the use of NSAIDs
patellar tendons at the inferior pole of the
is in any way associated with the risk of
randomized into 7 groups where they
received one of the following analgesics for 2
weeks: ibuprofen, acetaminophen, naproxen,
supported the use of
piroxicam, celecoxib, valdecoxib, or control.
post acute ankle sprain
At 2 weeks, all the animals were sacrificed,
(Slatyer et al 1997) yet
ankle sprain recurrence within 1-year is up to
33% (Hupperets et al 2009). Again, there has
demonstrated that the tendon strength in the
yet to be study investigating if the use of
control group (no meds) was significantly

stronger and had greater maximum load
biomechanical strength of their repaired
compared with the celecoxib, valdecoxib,
rotator cuff tendon when compared to the
and piroxicam groups.
placebo group (Chechik et al 2014).
Here is a summary quote from the paper,
Enough rat studies, let's take a look at this
study (Cohen et al 2006) where 180 rabbits
"Anti-inflammatory
with
the
received rotator cuff
exception of ibuprofen, had a detrimental
effect on healing strength at the bone-
tendon junction" and "Acetaminophen had
no effect on healing strength." (Ferry et al
placebo or one of two
NSAIDs (celecoxib or
indomethacin) for 2
To continue, here is the third rat study
weeks post-op. The animals were then
(Dimmens et al 2009) where the Achilles
sacrificed after 2, 4 and 8 weeks and their
tendons of 60 rats were not only cut, but a 3
rotator cuff tendons were biomechanically
mm segment of the tendon was fully cut out
and histologically analyzed. There were
and left unrepaired. Post-injury, the rats were
significantly lower rotator cuff failure
given one of two NSAIDs (parecoxib or
loads in the rabbits who received the
indomethacin) or placebo for one week. After
NSAIDs and in fact 5 of the tendons in the
2 weeks when the rats were sacrificed, they
NSAID group completely failed to heal
found that those who received NSAIDs had
whereas all the tendons in the control group
impaired tendon healing and had
Collagen
significantly lower Achilles tendon tensile
maturation was significantly poorer in the
strength when compared to the control
NSAID group at 4 and at 8 weeks post-op.
group. Relative to the control group, the
Here is a quote from the paper published in
diameter of the tendons were reduced in
the American Journal of Sports Medicine,
both NSAID groups.
".nonsteroidal anti-inflammatory drugs
significantly
healing. If the results of this study are
verified in a larger animal model, the
common practice of administering non-
steroidal anti-inflammatory drugs after
rotator cuff repair should be reconsidered."
(Cohen et al 2006)
Despite all the above-mentioned animal
studies, the most recent literature review on
this topic concludes that there is insufficient
evidence to support that NSAIDs may have a
In the most recent and fourth study, once
detrimental effect on soft-tissue healing;
again rats received surgical rotator cuff
however there is clear evidence that some
repairs. They showed that those given
NSAIDs have an inhibitory effect on bone
NSAIDs (meloxicam) between 11-20 days
healing (Chen & Dragoo 2013).
after post-op had significantly reduced
Here a sample study (O'Connor et al 2009)
As typically observed in human studies,
where 67 rabbits received fibula osteotomies
within one week post injury, those who
and were then allocated to receive either
received NSAIDs had more functional
placebo medications or NSAIDs (iboprofin
recovery however after 4 weeks the NSAID
or rofecoxib). After 6 weeks the rabbits were
group had a greater deficit in their muscular
sacrificed and they clearly demonstrated that
force generation when compared to the
compared to the placebo
untreated controls.
received
This study demonstrated that although
NSAIDs had significantly
NSAIDs provided short-term improvements
higher percentage of non-
in the initial week following the injury, after
4 weeks the rabbits treated with NSAIDs had
torsional
mechanical
significantly decreased torque and tension
strength.
production of their effected muscles. Once
again, this study concluded that a brief
And to quote the paper published in The
course of NSAIDs did provide short-term
Journal of the American Academy of
benefit but it was a decrement in long-
Orthopaedic Surgeon,
term muscle function.
"When fracture healing or spine fusion is
Here is a direct quote from the above-
desired, nonsteroidal anti-inflammatory
mentioned paper published in The Journal of
drugs should be avoided." (Dahners et al
Bone and Joint Surgery,
"By suppressing the initial inflammatory
Here is the only experimental study I could
reaction, the NSAID permits improved
find on the effects of NSAIDs on muscle
performance in early time-periods but
healing (Mishra et al 1995). This time rabbit
appears to suppress the stimulus that may
be needed for cellular remodeling in longer
experimentally induced eccentric contraction
muscle injuries, simulating an eccentric
overload injury of the hamstrings or
A review paper (Ziltener et al 2010)
gastrocnemius muscle that frequently occurs
published in the Annals of Physical and
in athletes (e.g. sprinters).
Rehabilitation Medicine written by sports
medicine physicians states,
Following the induced muscle injury, half the
rabbits received NSAIDs (iboprofin) two
"We do not recommend their use (NSAIDs)
times a day for six days and the other half
for muscle injuries".
served as the control (natural healing). The
rabbits' muscles were histologically and
Considering all the aforementioned studies
structurally analyzed at one week and 4
and review papers one may question why
weeks post injury.
there is still controversy over the use of NSAIDs on soft-tissue injuries. Simple: animal studies hold limited value in medicine and human trials have not yet demonstrated the same adverse effects on tissue healing as the speculation has not yet been researched.
As one can appreciate, due to obvious ethical reasons
experimentally induced injuries followed by in vivo histological examination of the injured muscle, tendon, or ligament is not possible. However, the one human study that is worth mentioning here involved 364 Australian army
sustained ankle sprains
Anterior Drawer Test (Ankle): With the tibia
(Slatyer et al 1997).
and fibula stabilized, the talus is drawn forward and the degree of laxity is noted and compared
to the contra-lateral side.
injury the recruits were randomized to receive
on day 1, 3, 7 and 14. Initially following the
either NSAIDs (piroxicam) or placebo. Not
ankle sprains the patients in both groups
surprisingly they clearly demonstrated that
(NSAID and placebo) had similar ankle
those who took the NSAIDs experienced
laxity using the anterior drawer test.
significantly less pain, more rapid functional
However at day 3, 7 and 14 the patients
endurance. The mean number of military
treated with NSAIDs had significantly
training days lost was 2.7 from the NSAID
greater ankle instability than the placebo
group and 8.5 from the placebo groups,
group. After 3 days, 74% of the patients
which proved NSAIDs to be a cost-effective
given placebo had a reversal of their ankle
instability test where their anterior drawer
test became negative, compared to 28% of
If you simply finish reading the paper based
those taking NSAIDs demonstrated the same
on these facts then case closed, a physician is
reversal. After 14 days, the reversal of the
perfectly justified in prescribing NSAIDs for
anterior drawer test was seen in 97% of the
a patient with an ankle sprain and the injured
patients given placebo compared to 78% of
athlete would be crazy not to take NSAIDs
those taking NSAIDs.
considering it clearly reduces pain and
improves function. The study then boldly
Compared to the placebo group, the patients
concludes that, NSAIDs should form an
given NSAIDs had significantly less ROM
integral part in the management of acute
ankle sprains. (Note: Study funded by Pfizer Pty Lt)
inversion at 7 and 14 days. Ironically those
treated with NSAIDs subjectively reported
Let's hold on here though. Could the short-
greater swelling at 7 days, 14 days, 3
term decreases in pain and improvements in
months and 6 months post injury.
function with NSAIDs be at the expense of
the injured soft-tissue in the long-term?
Interestingly there were no
differences between the
placebo and NSAID group
emphasize the ankle instability and range of
with respect to recovery
motion (ROM) findings that were measured
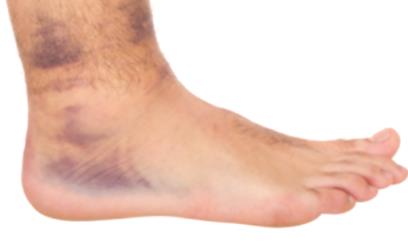
from ankle bruising.
Although the study reports that the recurrence rate was 25% within the 6 months of the study, regrettably they did not analyze the difference in recurrence between the two groups. It is hypothesized that since the patients in the NSAID group had reduced pain, they may have resumed activity prematurely thereby explaining the increased swelling, loss of mobility and greater ligamentous laxity.
movement(s) in the right direction(s)
performed at the optimum intensity and
Here is a quote from another paper pushed in
frequency may be potentially more effective
The Open Rehabilitation Journal;
in both short and long-term in individuals
post acute soft-tissue injuries.
"…NSAIDs are no longer recommended for
chronic soft-tissue (ligament) injuries, and
The follow-up to this paper will review the
their use is cautioned in athletes who have
evidences supporting physical therapists /
ligament injuries." (Hauser et al 2013)
physiotherapists as the ideal health care
providers with the ability to effectively
"In the case of acute ligament injuries,
evaluate and efficiently prescribe the
NSAIDs should be used for the shortest
optimum daily exercise / movement program
time possible, if used at all" (Hauser et al
musculoskeletal injuries.
I will make a confession that this has been a very biased paper where I have selectively
References:
presented the studies that show the potential
1. Chechik O1, Dolkart O, Mozes G, Rak O, Alhajajra F,
negative side of NSAID usage. However,
Maman E. Timing matters: NSAIDs interfere with the late proliferation stage of a repaired rotator cuff tendon
from an unbiased view, thus far there is still
healing in rats. Arch Orthop Trauma Surg. 2014
Apr;134(4):515-20.
completely dismiss the use of NSAIDs to
2. Chen MR1, Dragoo JL. The effect of nonsteroidal anti-
treat acute soft-tissue injuries.
inflammatory drugs on tissue healing. Knee Surg Sports
Traumatol Arthrosc. 2013 Mar;21(3):540-9.
In conclusion, considering the undeniable
3. Chung JW1, Zeng Y, Wong TK. Drug therapy for the
cardiovascular and GI risks in the use of
treatment of chronic nonspecific low back pain: systematic review and meta-analysis. Pain Physician.
NSAIDs, and taking into account the
2013 Nov-Dec;16(6):E685-704.
potential hindrance to tissue recovery, we
4. Cohen DB1, Kawamura S, Ehteshami JR, Rodeo SA.
must continue to question the ever growing
Indomethacin and celecoxib impair rotator cuff tendon-
use of NSAIDs in those post acute soft-tissue
to-bone healing. Am J Sports Med. 2006 Mar;34(3):362-9.
5. Dahners LE1, Mullis BH. Effects of nonsteroidal anti-
inflammatory drugs on bone formation and soft-tissue
On a more positive note, there is mounting
healing. J Am Acad Orthop Surg. 2004 May-
evidence that EXERCISE and PHYSICAL
Jun;12(3):139-43.
ACTIVITY have anti-inflammatory benefits.
6. Dimmen S1, Engebretsen L, Nordsletten L, Madsen JE.
Therefore instead of immediately reaching
Negative effects of parecoxib and indomethacin on
for the NSAID bottle, perhaps the correct
tendon healing: an experimental study in rats. Knee Surg Sports Traumatol Arthrosc. 2009 Jul;17(7):835-9.
7. Ferry ST, Dahners LE, Afshari HM, Weinhold PS. The
low back pain. Cochrane Database Syst Rev. 2008 Jan
effects of common anti-inflammatory drugs on the
healing rat patellar tendon. Am J Sports Med. 2007
20. Singh Gurkirpal, MD, "Recent Considerations in
Aug;35(8):1326-33.
Nonsteroidal Anti-Inflammatory Drug Gastropathy",
8. Griffin G1, Tudiver F, Grant WD. Do NSAIDs help in
The American Journal of Medicine, July 27, 1998, p.
acute or chronic low back pain? Am Fam Physician.
2002 Apr 1;65(7):1319-21.
21. Slatyer MA1, Hensley MJ, Lopert R. A randomized
9. Hauser RA, E.E. Dolan, H.J. Phillips, A.C. Newlin, R.E.
controlled trial of piroxicam in the management of acute
Moore and B.A. Bentham Ligament Injury and Healing:
ankle sprain in Australian Regular Army recruits. The
A Review of Current Clinical Diagnostics and
Kapooka Ankle Sprain Study. Am J Sports Med. 1997
Therapeutics The Open Rehabilitation Journal, 2013, 6,
Jul-Aug;25(4):544-53.
22. Warden SJ1, Avin KG, Beck EM, DeWolf ME,
10. Hunt RH1, Choquette D, Craig BN, De Angelis C,
Hagemeier MA, Martin KM. Low-intensity pulsed
Habal F, Fulthorpe G, Stewart JI, Turpie AG, Davis P.
ultrasound accelerates and a nonsteroidal anti-
inflammatory drug delays knee ligament healing. Am J
cyclooxygenase-2
Sports Med. 2006 Jul;34(7):1094-102.
traditional NSAIDs? Can Fam Physician. 2007
23. Wolfe M. MD, Lichtenstein D. MD, and Singh
Jul;53(7):1177-84.
"Gastrointestinal
11. Hupperets MD1, Verhagen EA, van Mechelen W. Effect
Nonsteroidal Anti-inflammatory Drugs", The New
of unsupervised home based proprioceptive training on
England Journal of Medicine, June 17, 1999, Vol. 340,
recurrences of ankle sprain: randomised controlled trial.
No. 24, pp. 1888-1889.
BMJ. 2009 Jul 9;339:b2684.
24. Ziltener JL1, Leal S, Fournier PE.Non-steroidal anti-
12. Jones P1, Lamdin R. Oral cyclo-oxygenase 2 inhibitors
inflammatory drugs for athletes: an update. Ann Phys
versus other oral analgesics for acute soft tissue injury:
Rehabil Med. 2010 May;53(4):278-82, 282-8.
systematic review and meta-analysis. Clin Drug
Investig. 2010;30(7):419-37.
13. Klenerman L, et al The prediction of chronicity in
patients with an acute attack of low back pain in a general practice setting. Spine. 1995 Feb 15;20(4):478-84.
14. McGettigan P1, Henry D. Use of non-steroidal anti-
inflammatory drugs that elevate cardiovascular risk: an examination of sales and essential medicines lists in low-, middle-, and high-income countries. PLoS Med. 2013;10(2):e1001388.
15. Mishra DK1, Fridén J, Schmitz MC, Lieber RL. Anti-
inflammatory medication after muscle injury. A treatment resulting in short-term improvement but subsequent loss of muscle function. J Bone Joint Surg Am. 1995 Oct;77(10):1510-9.
16. O'Connor JP1, Capo JT, Tan V, Cottrell JA, Manigrasso
MB, Bontempo N, Parsons JR. A comparison of the effects of ibuprofen and rofecoxib on rabbit fibula osteotomy healing. Acta Orthop. 2009 Oct;80(5):597-605.
17. Pattanittum P1, Turner T, Green S, Buchbinder R. Non-
steroidal anti-inflammatory drugs (NSAIDs) for treating lateral elbow pain in adults. Cochrane Database Syst Rev. 2013 May 31;5:
18. Pattanittum P1, Turner T, Green S, Buchbinder R. Non-
steroidal anti-inflammatory drugs (NSAIDs) for treating lateral elbow pain in adults. Cochrane Database Syst Rev. 2013 May 31;5:CD003686.
19. Roelofs PD1, Deyo RA, Koes BW, Scholten RJ, van
Study summaries are available on www.aptei.com "Clinical Library" accessible by APTEI Report subscribers
Tulder MW. Non-steroidal anti-inflammatory drugs for
To request a copy of this article simply email [email protected]
Source: http://www.aptei.ca/wp-content/uploads/NSAID-Paper-2014-3.pdf
Reducing Maternal Mortality in Tanzania: Health Facility Assessment in Kigoma Summary Health Facility Assessment of Emergency Obstetric & Neonatal Care Services (EmONC) in Kigoma Region, Tanzania: Selected Findings Tanzania has the fourth highest number of maternal deaths in Sub-Saharan Africa and the sixth highest in the world (World Health Organization, 2014). The
Original article Epidemiological Studies on Strongyloides stercoralis at Dilla District, Ethiopia Feleke Eriso Parasitologist, Department of Biology, Dilla University, Dilla, Ethiopia Corresponding Author Background and study aim: Some Results: In the study a total of 710 student Feleke Eriso








