Orofacial neuropathic pain and neuralgia in older adults
Orofacial Neuropathic Pain and
Neuralgia in Older Adults
HERMAN OSTROW SCHOOL OF DENTISTRY OF USC
Disclosure Information
Orofacial Neuropathic Pain and Neuralgia in Older Adults
Phuu Han
Continuing Medical Education committee members and those involved in the planning of this CME Event have no financial relationships to disclose.
I have no financial relationships to disclose
I will discuss off label use and/or investigational use of the following medications in my presentation.
Tricyclic antidepressants, Clonazepam, Oxcarbazepine, Lamotrigine, Gabapentin, Pregablin and Topiramate.
Orofacial Neuropathic Pain
Zakrzewska JM. J Headache Pain. 2013 Apr 25;14(1):37.
Common Neuropathic Orofacial Pain
Trigeminal NeuralgiaHerpes Zoster and Post-Herpetic NeuralgiaBurning Mouth Syndrome (BMS)
Zakrzewska JM. J Headache Pain. 2013 Apr 25;14(1):37.
Trigeminal Neuralgia - Epidemiology
• Annual incidence 4 – 13 per 100,000 people• Most frequently seen neuralgias in the elderly• Peak age of onset 50 - 60 years and incidence
increase with age
• Male : Female – 1 : 1.7• Most commonly involved V2 and/or V3 division• V1 division is involved in <5% of patient
Trigeminal Neuralgia IASP 2013, Trigeminal Neuralgia; UpToDate.com Topic 5283 Version 17.0
Trigeminal Neuralgia - Classic
A. At least three attacks of unilateral facial pain fulfilling criteria B
B. Occuring in one or more divisions of the trigeminal nerve, with
no radiation beyond the trigeminal distribution
Pain has at least three of the following characteristics:1.
recurring in paroxysmal attacks lasting for a fraction of a
second to 2 minutes2.
electric shock-like, shooting, stabbing or sharp in quality
precipitated by innocuous stimuli to the affected side of the
No clinically evident neurological deficit
D. No better accounted for by another ICHD-3 diagnosis
The international Classification of Headache Disorders, 3rd Edition (beta version). Cephalagia 2013; 33: 629.
Trigeminal Neuralgia - Classic
• Classical trigeminal neuralgia, purely paroxysmal• Classical trigeminal neuralgia with concomitant persistent
(Atypical trigeminal neuralgia; trigeminal neuralgia type 2)
A. Recurrent attacks of unilateral facial pain fulfilling criteria for 13.1.1 Classical trigeminal neuralgia
B. Persistent facial pain of moderate intensity in the affected area
C. Not better accounted for by another ICHD-3 diagnosis.
Trigeminal Neuralgia - Classic
Usually unilateral but it may rarely occur bilaterally
Following a painful paroxysm there is usually a refractory periodduring which pain cannot be triggered.
In some cases a paroxysm may be triggered from somatosensorystimuli outside the trigeminal area, such as a limb, or by othersensory stimulation such as bright lights, loud noises or tastes.
The pain often evokes spasm of the muscle of the face on the
affected side (
tic douloureux).
Many, possibly most (80 – 90%), patients with this condition havecompression of the trigeminal root by tortuous or aberrant vessels.
Classical trigeminal neuralgia is usually responsive, at least initially,to pharmacotherapy.
Painful trigeminal neuropathy attributed to
MS Plaque
A. Head and/or facial pain with the characteristics of Classical
persistent facial pain, but not necessarily unilateral
B. Multiple sclerosis (MS) has been diagnosedC. An MS plaque affecting the trigeminal nerve root has been
demonstrated by MRI or by routine electrophysiologicalstudies (blink reflex or trigeminal evoked potentials)indicating impairment of the affected trigeminal nerve(s)
D. Not better accounted for by another ICHD-3 diagnosis.
The international Classification of Headache Disorders, 3rd Edition (beta version). Cephalagia 2013; 33: 629.
Painful trigeminal neuropathy attributed to
space-occupying lesion
A. Unilateral head and/or facial pain with the characteristics
concomitant persistent facial pain and fulfilling criterion C
B. A space-occupying lesion, and contact between the lesion
demonstrated by imaging
C. Pain has developed after contact occurred between the
lesion and the trigeminal nerve, or led to its discovery
D. Not better accounted for by another ICHD-3 diagnosis.
E.g Acoustic neuroma, meningioma, epidermoid cyst,
aneurysm or AV malformation
The international Classification of Headache Disorders, 3rd Edition (beta version). Cephalagia 2013; 33: 629.
Secondary/Sympomatic
• There may be sensory impairment in the distribution
of the appropriate trigeminal division.
demonstrates refractory period after a paroxysm.
• May not respond to pharmacologic treatment.
Pretrigeminal neuralgia
• Pretrigeminal neuralgia unnecessary dental
The international Classification of Headache Disorders, 3rd Edition (beta version). Cephalagia 2013; 33: 629.
Trigeminal Neuralgia – Clinical Examination
• History• Clinical examination – Cranial nerve examination• Characteristics of symptomatic TN
•
presence of sensory deficit
• age of onset
• first division involvement
•
bilateral involvement
• unresponsiveness to treatment
•
abnormal blink reflexes
• Additional examination – CT, MRI, MRA ( up to 15% of patients with TN), Evoked potential • Treatment – Pharmacologic, Botulinum Toxin Injection, Surgical (Peripheral or central)
Trigeminal Neuralgia IASP 2013, Trigeminal Neuralgia; UpToDate.com Topic 5283 Version 17.0
Trigeminal Neuralgia – Pharmacological Treatment
Initial Dosage
Target Dose
Dose Increase
Schedule
100-200 mg/2 days
Transfer from regular
300 – 600 mg/week
25 – 60 mg/week
300 mg/1 – 2 days
50 mg/ 2 – 3 days
Orofacial Pain and Headache (2008) Mosby (ELSEVIER) Pg. 265 and
Am Fam Physician. 2009 Jun 1;79(11):1001-1002
Trigeminal Neuralgia - Treatment
Trigeminal Neuralgia - Treatment
Neurosurg Clin N Am. 2014 Oct;25(4):751-762.
Case - Trigeminal Neuralgia
Acute Herpes Zoster (Shingle):
• Caused by VZV• 30% lifetime risk of developing zoster• Affects adults older than 50 years• Severity and incidence increase with age (age related decline in cell-
mediated immunity)
• Risks : immunosuppression, advanced age, malignancy, chronic kidney
or lung disease, HIV infection etc
• 50% of patients over age 85 years will have an episode of herpes zoster
Painful Trigeminal Neuropathy Attributed to
Acute Herpes Zoster
A. Unilateral head/or facial pain lasting <3 months and fulfilling
B. Either or both of the following:
1. herpetic eruption has occurred in the territory of a trigeminalnerve branch or branches2. varicella zoster virus DNA has been detected in the CSF by PCR
C. Evidence of causation demonstrated by both of the following:
1. pain preceded the herpetic eruption by < 7 days2. pain is located in the distribution of the same trigeminal nervebranch or branches
D. No better accounted for by another ICHD-3 diagnosis
The international Classification of Headache Disorders, 3rd Edition (beta version). Cephalagia 2013; 33: 629.
Painful Trigeminal Neuropathy Attributed to
Acute Herpes Zoster
• Affects the trigeminal ganglion in 10–15% of cases.
• Ophthalmic division being singled out in some 80% of
patients. (Only Intra-oral lesions can also occur)
• Rarely, pain is not followed by an eruption or rash (zoster
sine herpete).
• Burning, stabbing/shooting, tingling or aching, and
accompanied by cutaneous allodynia
• Herpes zoster is common in immunocompromised patients
The international Classification of Headache Disorders, 3rd Edition (beta version). Cephalagia 2013; 33: 629.
Painful Trigeminal Neuropathy Attributed to
Acute Herpes Zoster
• CN V1 dermatome, ipsilateral forehead, and upper eyelid
When lesions are found in the CN V1 dermatome
• Presence of orbital edema is an ophthalmologic emergency• Nasociliary branch involvement, with vesicles at the tip of
the nose, can indicate that eye involvement is present (theHutchinson rule). A slit-lamp examination is done to identifycorneal findings.
• Ophthalmic herpes may be associated with IIIrd, IVth and
VIth cranial nerve palsies.
• Signs of meningeal irritation and meningitis must be
Jude E, Chakraborty A. N Engl J Med 2005;353:e14.
Painful Trigeminal Neuropathy Attributed to
Acute Herpes Zoster
• CN V2 – Ipsilateral cheek, the lower eyelid, side of the nose,
upper eyelid, upper teeth, mucous membrane of the nose,nasopharynx, the tonsils and the palate.
• CN V3 - involvement include the side of the head, the external
ear and external auditory canal, the lower lip, and a portion ofthe oral mucosa.
• Only the oral mucous membrane can involved with no
Am Fam Physician. 2008 May 1;77(9):1307-1309 •
Early pre-eruptive herpetic pain can stimulate a severetoothache and result in unnecessary oral surgical or dentaltreatment
The international Classification of Headache Disorders, 3rd Edition (beta version). Cephalagia 2013; 33: 629.
Facial Neuropathy Caused by Acute Herpes Zoster
• Burning and itching pain of the
affected areas and may be extremelybothersome.
• Pale or light purple scars or skin
changes may be present
• Herpes zoster oticus (Ramsay Hunt
• CN VII – Facial Palsy
• CN IX, X and XI, (XII) – Jugular
Cohen JI. N Engl J Med 2013;369:255-263
Cohen JI. N Engl J Med 2013;369:255-263
Post-herpetic Trigeminal Neuropathy
A. Unilateral head/or facial pain persisting or recurring for 3
months and fulfilling criterion C
B. History of acute herpes zoster affecting a trigeminal nerve
branch or branches
C. Evidence of causation demonstrated by both of the
following:1. pain developed in temporal relation to the acuteherpes zoster2. pain is located in the distribution of the sametrigeminal nerve branch or branches
D. No better accounted for by another ICHD-3 diagnosis
The international Classification of Headache Disorders, 3rd Edition (beta version). Cephalagia 2013; 33: 629.
Post-Herpetic Neuralgia (PHN)
A. Damage to the nervous system
1) Deafferentation2) Peripheral and/or central sensitization3) Myelin destruction4) Inflammation5) Signalling errors in the brain
B. As many as 20% (9-34%) of patients with Singles develop
C. More prevalent in elderly >60 years of age
D. PHN incidence : Risks : older age, greater acute pain,
greater rash severity, ophthalmic location of rash
Journal of Pain Research 2014: 7; 125-132.
Johnson RW, Rice AS. N Engl J Med 2014;371:1526-1533.
Suggested therapeutic ladder for treatment of post-herpetic neuralgia
Gan EY, Tian EA, Tey HL. Am J Clin Dermatol. 2013;14(2):77-85. Massengill JS, Kittredge JL. J Pain Res. 2014;7:125-32.
Prevention of Post-Herpetic Neuralgia
- Childhood vericella vaccine
- VZ vaccines – FDA approved for individuals >= 50 years of age
◦ Life attenuated vaccine◦ >14 times more potent than vericella vaccine◦ subcutaneously as a single dose◦ Activates specific T-cell production◦ Prevents viral reactivation◦ Reduced the overall incidence of shingles by 51% and the incidence of PHN by 67%. ◦ The efficacy (reduction in risk of herpes zoster) was higher in the younger age group (60-69
years; vaccine efficacy was 64%) than in the older age group (older than 70 years; vaccine efficacy was 38%).
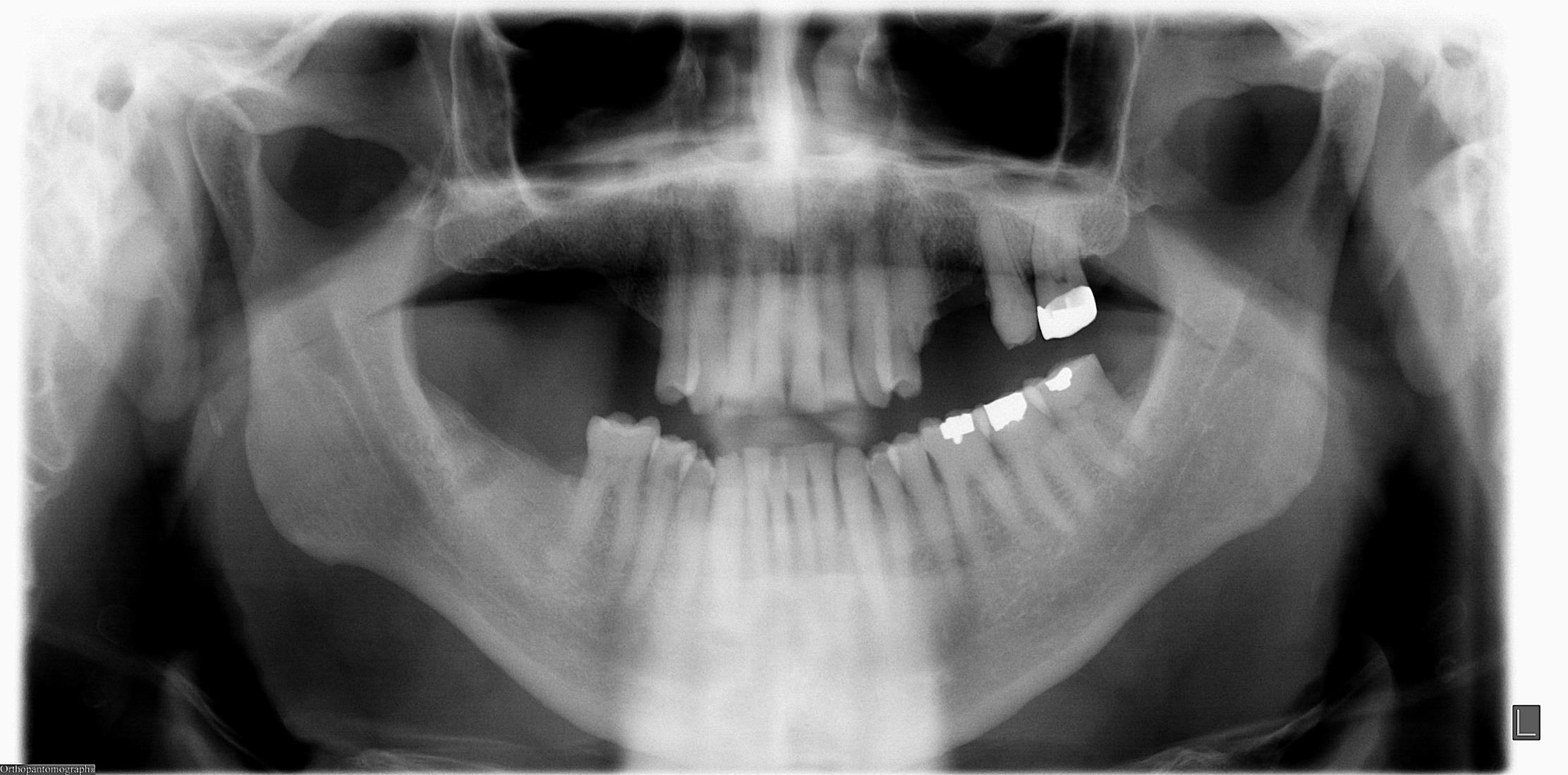
Case - Post-Herpetic Neuralgia
• 55 YO female patient
• Pain on the lower left posterior gingiva
• Constant burning pain started after cleaning
• Still painful for more than one month
• Good dentition, good hygiene
Burning Mouth Syndrome (BMS)
• Burning sensation of the oral mucosa in the absence of clinically apparent mucosal
• Positive sensory symptoms : burning pain, dysgeusia, dysestheisa, dry mouth• Negative sensory symptoms: loss of taste and paresthesia• Affects the tongue (tip and lateral borders, anterior two third), lips, hard and soft
palate, alveolar ridges
• Common in Female of 5th to 7th decades with female : male ratio of 3:1 to 16:1• Around menopause ( 3 years before and 12 years after the onset of menopause)• Prevalence: 0.7 – 7% of general population, up to 12 – 18% in post menopausal women
Klasser GD et al. J Am Dent Assoc. 2013;144(10):1135-42, Sun A et al. J Oral Pathol Med. 2013;44:649-655.
Burning Mouth Syndrome
A. Oral pain fulfilling criteria B and C
B. Recurring daily for >2 hours per day for >3 months
C. Pain has both of the following characteristics:
1. burning quality
2. felt superficially in the oral mucosa
D. Oral mucosa is of normal appearance and clinical
examination including sensory testing is normal
E. Not better accounted for by another ICHD-3
The international Classification of Headache Disorders, 3rd Edition (beta version). Cephalagia 2013; 33: 629.
Burning Mouth Syndrome
International Association for the Study of Pain (IASP)
"Burning pain of the tongue or other oral mucous membranepersisting for at least four months and associated with normaloral mucosa and normal laboratory findings."• Burning sensation of the tongue or other oral mucosa• Usually bilateral• Associated with dysgeusia, dry mouth and denture intolerance
Klasser GD, Pinto A, Czyscon JM, Cramer CK, Epstein J. J Am Dent Assoc. 2013;144(10):1135-42.
Classification and subtypes
• Three types according to clinical oral pain pattern
• Type 1 (35%) : pain free waking, burning sensation develop in
late morning and gradually increasing in severity during the day,reaching peak intensity by evening, usually linked to systemicdisorders such as nutritional deficiency, diabetes mellitus
• Type 2 (55%) : continuous symptom thorough out the day,
difficult to sleep, usually associated with psychological disorders
• Type 3 (10%) : intermittent symptoms with pain free periods
during the day, associated with allergic reactions
Sun A et al. J Oral Pathol Med. 2013;44:649-655
Classification and subtypes
• Scala et al.
• Primary (essential or idiopathic with no organic cause)
• Secondary (local, systemic or psychological factors)
• Three types according to pathophysiology of primary burning
• Small diameter fiber neuropathy (50 – 65%)
• Subclinical lingual, mandibular or trigeminal system pathology (20 – 25%)
• Central pain related to hypofunction of dopaminergic neurons in basal
ganglia (20 – 40%)
Sun A et al. J Oral Pathol Med. 2013;44:649-655
Burning Mouth Syndrome
Altered structure and function in the hippocampus and medial prefrontal cortex in patients with burning mouthsyndrome
9 healthy control and 9 Clinical Type 1 BMS patients
Record pain, anxiety and depression ratings
Measured gray matter volume (GMV), white matter and resting state functional MRI
Patients had increased GMV and lower FA in the hippocampus (Hc), and decreased GMV in the medial prefrontalcortex (mPFC).
rsfMRI revealed altered connectivity patterns in different states of pain/burning
mPFC-Hc connectivity was higher in BMS patients than control subjects for the afternoon but not the morningsession.
Evidence supporting aberrant structure and function in the medial prefrontal cortex and Hippocampus, andimplicate a circuit involving the these brain structures in regulating mood and depressive symptoms in BMS.
Khan SA, Keaser ML, Meiller TF, Seminowicz DA. PAIN 155 (2014) 1472–1480.
Burning Mouth Syndrome
Psychological Factors
Zakrzewska JM. J Headache Pain. 2013;14(1):37.
Burning Mouth Syndrome
Suarez P, Clark GT. J Calif Dent Assoc. 2006;34(8):611-22.
Suarez P, Clark GT. Chapter 14 pg. 241-242 in Dionne, R., & Clark, G. T. (2012). Orofacial Pain : A Guide to Medications and Management.
Suarez P, Clark GT. Chapter 14 pg. 241-242 in Dionne, R., & Clark, G. T. (2012). Orofacial Pain : A Guide to Medications and Management.
Burning Mouth Syndrome
- Cognitive behavior therapy (one/week for 12 – 15 weeks)
- Alpha-lipoic acid (600mg/day) more effective if combine with
psychotherapy- Clonazepam (0.25 to 0.5mg topical or systemic once a day to three
Notes◦ Systemic clonazepam should not be use in older patients with fall risks◦ Very long duration of action
Sun A et al. J Oral Pathol Med. 2013;44:649-655.
Zakrzewska JM et al. Cochrane Database Syst Rev. 2005 Jan 25;(1):CD002779.
Zakrzewska JM. Multi-dimensionality of chronic pain of the oral cavity and face. J Headache Pain. 2013 Apr 25;14(1):37.
Thank you!
Source: http://www.centerfororalhealth.org/images/events/2015_symposium/presentationslides/8-Han.pdf
Investigación Captopril por vía oral y sublingual en pacientes con urgencia hipertensiva Captopril orally and sublingually in patients with hypertensive urgency 1Arquimides Mackelin Ortega Vázquez, 2Norma Elena Corona Amador. 1Adscripción: UMF 56 León; Guanajuato. 2Adscripción: HGZ/UMF 21 León; Guanajuato. Resumen Introducción La Urgencia hipertensiva se presenta generalmente en enfermos con hipertensión arterial sistémica. El 1% de los pacientes hipertensos tendrán crisis hipertensiva de la cual el 76% será Urgencia hipertensiva y 24% emergencia ( Papaduopulos D,2010). Objetivo Evaluar si el Captopril sublingual es mejor para el control de la urgencia hipertensiva que el captopril vía ora en los pacientes atendidos en urgencias de la UMF 56 de Julio a Diciembre del 2013. Material y métodos Se realizó un estudio cuasi experimental, el tamaño de la muestra se calculó de la diferencia entre dos proporciones, con un nivel de confianza del 95%, con 40 pacientes en cada uno de los grupos (sublingual Vs oral); por casos consecutivos y de forma aleatoria se asignó al grupo oral o sublingual, en ambos casos se administró molida la tableta de captopril. La población de estudio fueron los derechohabientes que acudieron al servicio de urgencias de UMF 56 de Julio a Diciembre del 2013, y que cumplieron los criterios de diagnóstico de urgencia hipertensiva. Resultados Captopril molido sublingual mostro mayor rapidez en cuanto el control de la Tensión Arterial Media ≤ 100mmHg y disminución TAM ≥ 20%, Comparando los promedios de control de las TAM de ambos grupos encontramos una diferencia estadísticamente significativa de P= 0.0035. Conclusión Observamos que el 16.25% de la muestra desconocía ser hipertenso. El 82.35% (42 pacientes) de los pacientes descontrolados son manejados con un anti-hipertensivo. Encontramos una relación directamente proporcional del índice de masa corporal y al grado de descontrol de hipertensión a su ingreso.
1st Annual Newsletter Dear Sir or Madame, It is my pleasure to present the First Annual Newsletter concerning the IntelliDrug project - the project which addresses the need of new, less invasive and more controlled drug delivery. The outcome of IntelliDrug is an intra-oral device, which will provide new therapeutic opportunities for people suffering from chronic diseases and drug addiction.

